Determinants of emergency contraceptive utilization among female tertiary students in the middle belt of Ghana, West Africa
Mustapha Hallidu, Issah Sumaila
Corresponding author: Issah Sumaila, Department of Public Health, Kintampo Municipal Hospital, Ghana Health Service, Bono East, Ghana 
Received: 11 Jun 2022 - Accepted: 02 Sep 2022 - Published: 09 Sep 2022
Domain: Gynecology, Obstetrics and gynecology
Keywords: Emergency, contraceptives, utilization
©Mustapha Hallidu et al. PAMJ-One Health (ISSN: 2707-2800). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Mustapha Hallidu et al. Determinants of emergency contraceptive utilization among female tertiary students in the middle belt of Ghana, West Africa. PAMJ-One Health. 2022;9:4. [doi: 10.11604/pamj-oh.2022.9.4.35866]
Available online at: https://www.one-health.panafrican-med-journal.com/content/article/9/4/full
Research 
Determinants of emergency contraceptive utilization among female tertiary students in the middle belt of Ghana, West Africa
Determinants of emergency contraceptive utilization among female tertiary students in the middle belt of Ghana, West Africa
&Corresponding author
Introduction: Emergency Contraceptives (ECs) are after-coital contraceptive methods used before implantation. These give females in the sexually active age group the opportunity to prevent unplanned pregnancies after refusing to patronize a contraceptive before unprotected sexual intercourse or when a regular contraceptive fails and or when raped. Higher education students fall under the sexually active age category and form a higher risk group for unplanned pregnancy because of inadequate utilization of ECs. The aim of this study was to identify the determinants of ECs utilization among female tertiary students in the Middle Belt of Ghana, West Africa.
Methods: institutional-based descriptive cross-sectional study design was used with quantitative method in collecting the data from 28th March 2022 to 18th April 2022. A total of 535 female tertiary students were recruited using simple random proportionate sampling technique. Data were collected using structured questionnaires and entered into Stata version 15 and analyzed descriptively and inferentially using Chi-squared test. A conventional p<0.05 was considered statistically significant.
Results: out of the 535 respondents that were interviewed, majority (426 (79.6%) were aware of ECs. However, only 44 (9.4%) had good knowledge of ECs utilization. All respondents who were affiliated to traditional religion had poor knowledge. About half of 279 (52.1%) indicated they ever utilized ECs and 200 (71.7%) of these said the efficacy of ECs was between 75-99%. Regarding barriers to ECs utilization, 333 (20.5%) indicated ECs cause infertility and 330 (20.4%) mentioned the fear of being seen by others. All Chi-square test of associations of demographic characteristics and knowledge on ECs were not statistically significant (p≥0.05).
Conclusion: the study reported that ECs utilization among female tertiary students was quite low despite majority being aware of them. Most of them had poor knowledge on ECs utilization, even though majority had not experienced unplanned pregnancies. Further reproductive health and family planning education and promotion initiatives directed on the utilizations of ECs, their efficacies and typology are needed, especially among future health professionals who will later educate other young adults.
Contraception is the application of non-natural methods or equipment to avoid unplanned pregnancy as a result of unprotected sexual intercourse. This could be achieved either by the man or woman, however, must be targeted towards comfort, privacy and freedom to select and plan for intentional pregnancies [1]. Contraception is a common practice amongst females during their motherhood periods [2]. Emergency Contraceptive (EC) is an after-coital contraceptive technique used before implantation, providing women with a second option to prevent unintentional pregnancies after failing to utilize a contraceptive before unprotected copulation or when a regular contraceptive fails and or when raped [3,4]. Emergency Contraceptive (EC) is not supposed to be considered a contraceptive method to be applied on a regular basis [5]. They are composed of an increased dose of the same active ingredients which regular birth control pills have [6]. The mechanism of action of EC is preventing pregnancy, inhibiting or delaying ovulation, but not avoiding implantation of zygotes. The drug does not cause abortion or embryo damage; it should be added also that, EC does not provide protection against sexually transmitted infection (STI) [5,7]. ECPs have 75% - 85% chances of preventing unplanned pregnancies, whilst combination of ECPs and IUDs can prevent almost 99% of unplanned pregnancies [8]. Unplanned pregnancies are of public health concern across the globe, accounting for 44% of all pregnancies with 74 million in low and middle income nations (LMIN) [4]. Each day, an estimated 1,000 women die from avoidable factors influenced by pregnancy and childbirth [4]. Adolescents encounter an elevated danger of complications and mortalities as a result of unintended pregnancy as compared to older women [4]. The World Health Organization (WHO) predicts that at least 33% of all women seeking hospital care for difficulties influenced by abortions are less than 20 years [4]. In sub-Sahara Africa (SSA), almost 29.1% of all pregnancies are unplanned, with 35.8% in Ghana [9]. About 600,000 women mortalities are recorded as a result of pregnancy-related causes [9]. Unplanned pregnancies contribute to 25 million unsafe abortions and 47,000 maternal mortalities annually [10]. In 2018, 101 unplanned pregnancies happened per 1000 women between the ages of 15 - 44 years and 42% of all the pregnancies were unintended [3].
Globally, 23 million girls aged between 15 - 19 years have unmet needs for contraception, and 16 million girls give birth before their 16th birthday [11]. Both males and females suffer an unbalanced share of unintended pregnancies, abortions and other dangerous reproductive health complications and to alleviate these challenges EC can be of significant assistance [12]. In Africa, 24% of young female adults have the highest rates of unmet needs for EC, according to WHO [13]. Even though the continent records 29% of all unsafe abortions, it accounts for 62% of unsafe abortions-related to mortalities. The increased rate of unplanned pregnancies because of inadequate access to women´s reproductive health services suggests that most SSA nations have limited access to facilities for family planning and reproductive health rights which to some extent not contribute to the realizing of the United Nations (UN) Sustainable Development Goal 3 (SDG 3) [10]. The incidence of unsafe abortions is 25 million yearly, and 3 out of 4 abortions prevalence in Africa are treacherous, with the dangers of mortalities from abortion highest in Africa [10]. Emergency Contraceptive (EC) is useful to women who have experienced method failures, inappropriate use of contraceptives, sexual assaults or have agreed to unintended and unprotected sexual intercourse [10]. Emergency Contraceptive (EC) is exceptional amongst contemporary contraceptive methods in its capability to avoid pregnancies after unprotected sex [14]. A study has indicated a dearth of knowledge about the existence of EC, its effectiveness, and supply including access to it, its effective deadline and the lack of recognition of the essence for its utilization can impede women from patronizing it [15]. Around 30% - 50% of the young below 30 years have utilized the ECPs at each stage in their lives, however, knowledge regarding this medication is limited [5]. Multiple barriers exist for women to obtain or utilize contraceptives effectively and consistently [16].
Sex education and training these days are poor and in most instances do not include EC [17,18]. Sex education has demonstrated to influence sexual behavior, the latter becoming healthier [19]. In setting of university stages, sex education in EC and sexual health is needed, especially for health professionals who can include sex education in their teaching activities [5,20]. Many young adults, particularly female tertiary students, engage in sexual activities before marriage and intended pregnancies, usually without EC bringing about unplanned pregnancies in most nations [4]. When young adults gain admissions to schools (tertiary) they stay away from their immediate families in rented homes or campus hostels for a long time without direct supervision of their parents. According to a study, adolescents are more likely to interact sexually with different sexual partners because of scanty information and accessible facilities concerning STIs, as they stand the higher risk of becoming pregnant unintentionally [21]. A lot of studies have been carried out on ECs in Ghana, but our scholastic search in the middle belt of Ghana depicted limited literature on the determinants of ECs utilization amongst female tertiary students. Hence, this study was conducted to identify the determinants of ECs utilization amongst female tertiary students in the Middle Belt of Ghana, West Africa.
Study design and setting: descriptive cross-sectional study design was used with quantitative methodology. The study was carried out in the middle belt of Ghana (Bono, Bono East and Ahafo Regions) from March 2021 to April 2022. The study population was female tertiary students in the middle belt of Ghana.
Sampling population: the study included all female tertiary students with valid student identification cards who schooled within the middle belt of Ghana, of sound mind, were willing and agreed to participate in the study. All students outside these criteria were excluded from the study.
Study variables: the dependent variable was EC utilization among female tertiary students. The utilization of EC was determined using a simple question “have you ever used EC before”? This simple question required a simple answer of either “Yes” or “No”. All those who chose “Yes” were regarded as users of ECs. The independent variables were the female tertiary student´s characteristics (age, year of study, field of study, marital status religion, etc).
Sample size and sampling technique: the sample size was computed using the Yamane formula,
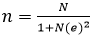
Data collection tools and procedures: a structured questionnaire was used to gather data for this study. The questionnaire was designed after reviewing relevant available literature on determinants of EC utilization [1,3-5,8,10,14,17,23]. The questionnaire was subdivided into sections A, B and C for easy analysis of the data based on the objectives. Section A captured the socio-demographic characteristics of respondents. Section B was on the knowledge and sources of information of respondents on ECs while section C captured respondents´ sexual activities and utilization of ECs. Three separate Google Forms were created with the same questionnaire. Each of the Google Forms was sent to 7 trained data enumerators (4 for STU, 2 for CoHK and 1 for GNMTC) in each region within the study setting. All the 7 data enumerators were subsequently tasked to share the digitized questionnaire with only female students in those selected tertiary institutions who met the inclusion criteria and consented to participate in the study. Interviewers approached the participants, and when they agreed, were asked their WhatsApp numbers to be sent the questionnaire. Those from STU were asked to interview 81 female students each. CoHK and GNMTC data enumerators each interviewed 94 and 63 female´s students, respectively. To ascertain the reliability of the data collection tool, the questionnaire was pre-tested among 50 female tertiary students in the Middle Belt of Ghana. The pre-testing afforded the researchers to modify the questionnaire to illicit the required responses from the participants. Respondents who were available were given access to the questionnaire through WhatsApp contact numbers. The digitized questionnaire was restricted in such a way that multiple responses from the same device were not allowed. Data was collected from February 2022 to March 2022.
Data analysis: after all questionnaires were checked for completeness, 535 questionnaires were considered for analysis. Primary data from Google form was downloaded, cleaned and managed using Microsoft Excel version 16. The data was later exported to Stata version 15 and analyzed. Gender, religion, marital status, educational level were coded as categorical variables. The data was presented in frequencies and percentages. Age was collected as continuous variable and categorized during analysis. The main outcome, knowledge level, was determined using 7 questions. 1 of the 7 questions had a “Yes” or “No” response. The rest had multiple options with multiple correct answers. Each correct answer was coded as “1” with “0” representing a wrong answer. The total correct answers summed up to 17. Any participant who had an aggregate score of at least 14 was considered to have good knowledge on ECs. Those with total score of 13 or less were considered as having poor knowledge on ECs. Descriptive statistics were used to present the proportions on background characteristics of the respondents at the univariate level. The data was presented in frequencies and percentages using tables.
Ethical consideration, registration: the study was carried out in strict adherence to the 1964 Helsinki declaration as revised in 2013 [24]. Approval was obtained from the Bono East Regional Health Directorate Ethical Review Committee, and permissions were also granted by the regional health directorates of the regions and the management of the tertiary institutions of the study settings before data were collected. Informed consents were obtained from the participants before they were allowed to participate in the study. Before a participant could access the electronic questionnaire, a request for consent appeared for the individual to consent to it before proceeding to answer the questionnaire. Anyone who did not consent to it could not access the questionnaire. Adequate information about the study was provided to the participants regarding the aim of the study. Participants were assured and guaranteed of anonymity, privacy and confidentiality. Furthermore, they were guaranteed of data safety and appropriate data usage and storage on the digitized questionnaire. Only participants who consented were recruited into the study. Participants adequately informed their liberties to pull out from the study at any point without any consequences. All participants´ personal identifiers were deleted from the summarised data, ensuring confidentiality.
Socio-demographic characteristics of respondents: a total of 1027 eligible respondents were approached for the study. Out of this, 583 of the respondents agreed and consented to participate in the study. However, only 535 of the questionnaire were complete. Hence, the study used the completed 535 questionnaires filled by female tertiary students in the middle belt of Ghana for the analysis. About half of them (47.1%) were between the age group of 20-24 years. Most (35.7%) were in their third year of study. The majority of the students (76.1%) were in the field of health sciences and a little over half of them (52.9%) were residents. Most (75.5%) were single and the majority (79.8%) subscribed to Christianity (Table 1).
Knowledge on emergency contraceptives: the study established that majority (79.6%) of the students had ever heard of ECs. Out of the 426 students who had ever heard of ECs, 272 (28.8%) of them heard it from health facilities, 258 (27.3%) indicated they heard it from the media while only 78 (8.2%) heard it from their partners. When asked about where to purchase ECs, 596 (67%) of the respondents said they could get it from a pharmacy or licensed chemical shop. Again, 252 (28.4%) indicated the ECs could be obtained from health facilities while 41 (4.6%) said it could be obtained from any shop. About half 464 (51.8%) of the respondents identified pills as EC. Approximately a quarter of the students also indicated that injectable (19.9%) and IUD (19.4%) are ECs. However, only 80 (8.9%) knew implanon is an EC. Majority 396 (74.0%) were of the opinion that the maximum time limit within which to take an EC after unprotected sex is 3 days. About a fifth (18.7%) did not know about it while 39 (7.3%) indicated a maximum of 5 days. Majority (492) of the respondents said ECs are recommended after unprotected sex. This was followed by 265, who indicated that ECs are to be taken when condoms raptures during protected sexual intercourse. Those who indicated ECs should be taken when one is raped were 243 while only 64 of them said it should be taken when one misses a period (Table 2).
Overall knowledge level of respondents on ECs: regarding the overall knowledge on ECs, majority (90.6%) of the respondents had poor knowledge. Those who had good knowledge of ECs were only 9.4%.
Respondents sexual activities and utilization of emergency contraceptives: out of the 535 students that were recruited, most (59.2%) had ever had unprotected sex. Majority (73%) of them never had unplanned pregnancy. Out of the 112 respondents who reported having unplanned pregnancy, about half of them (48.5%) attributed it to contraceptive failure while the rest (51.5%) attributed the unplanned pregnancy to forgetfulness to take contraceptives. Again, about half (47.9%) of the respondents indicated they never used ECs while the rest (52.1%) said they ever used it. Majority (71.7%) of the respondent indicated 75-99% as the efficacy rate of ECs. Only 5.4% believed the efficacy rate is <50%. When quizzed about their perceptions of the barriers to ECs use, most (333) of the participants indicated fear of being seen by others. This was followed by 330 respondents, who believed ECs cause abortion. Others (227), attributed the lack of utilization of the ECs to religious disapproval. The number of respondents who think societal disapproval prevents from utilization ECs was 174 (Table 3).
Association of socio-demographic characteristics of respondents with knowledge on ECS: respondents in the age group of 25 - 29 years had the highest percentage of poor knowledge on EC in this study (94.7%). Those who were at least 30 years had the least percentage (83.0%). Respondents in the first (91.1%), third (90.6%) and fourth years (96.8%) had higher percentage of poor knowledge on ECs compared to those in second year (86.4%). The percentage of poor knowledge on ECs among those in the health sciences (91.1%) was slightly higher compared to those in the non-health sciences (88.7%). Those who stayed on campus hostel had (90.0%) poor knowledge on ECs those who stayed in private hostel had (88.0%). The single participants had poor knowledge on ECs (91.3%) compared to those who were married (90.3%). It was found that those co-habiting had slightly good knowledge on ECs (19.2%) compare to the married (9.7%) and single respondents (8.7). With regards to religion, all those who subscribed to traditional religion (100.0%) had poor knowledge on ECs. The Chi-square test of associations showed that the knowledge on ECs among participants had no significant differences (p?0.05) with the demographic variables (Table 4).
Contraceptive utilization is a proxy for women´s empowerment, population growth and development [25]. In this study, majority of the participants had heard of ECs which is consistent with [3,5,6,10,26,27]. Out of those that had heard about ECs, majority indicated health facilities as their sources of information which is in agreement with similar studies conducted by [1,6]. However, findings from this study on the sources of information about ECs are inconsistent with similar studies by [26,28-30]. This could be ascribed to the fact that most of the respondents were Health Sciences students and might have acquired formal means of learning about reproductive health issues (family planning). Again, the open and free discussions on sex and sexuality among female students could be a reason. Hence, their large dependence on the information obtained from their field of practice (health facilities) and formal education in their curriculum. Importantly, majority of the respondents identified pharmacy/licensed chemical shops as where ECs could be obtained from. This is consistent with other studies carried out by [4,8,31,32]. This could be attributed to the fact that respondents´ were students and had all sources of information on ECs at their disposals particularly social media/internet where most students obtain their information from. A fairly significant number of the study participants indicated the various types of ECs available including pills, IUDs, injectable and implanon. This is in agreement with studies carried out by [2,6,10,26-28,33]. This could be credited to the experiences they might have acquired from the utilization of ECs and the availability of information on family planning services and benefits obtained from health facilities. Additionally, majority of the study participants expressed opinions that the maximum recommended time limit to take ECs is within 3 days after unprotected sexual intercourse. This supports different findings from studies established by [27,28,32,34,35]. This could be that they have had formal tuition on that from schools or might have read them from pamphlets/books. Significant insights from this study was also that, majority mentioned that ECs are recommended when an individual engages in unprotected sexual intercourse. This outcome is consistent with that of [23,27,31,32,35-37]. This could be attributed to the reason that, being tertiary students within the reproductive age bracket, they might have been exposed to the practices of ECs or sourced information on that from the media particularly internet.
Moreover, vital insights from this study concerning the overall knowledge level of the respondents was that majority of the study participants were poorly knowledgeable about ECs. Consistent with that of [5,14,27,29,30,34,35] even though with variations in the rates. However, this finding contradicts different studies conducted by [3,6,13,26]. This may be as a result of the fact that participants have not been exposed to in depth education and promotions of family planning and reproductive health services particularly on ECs. Equally, most of the study participants had unprotected sex before and majority had unintended pregnancy. These findings are not different from those by [36,38-40]. This could be related to the age categories of the study participants. Being in their reproductive ages and sexually active, they might have explored out of curiosity and engaged in unprotected sex resulting to unintended pregnancy. Pertaining to the reasons for their unintended pregnancies, quite a significant number of the respondents expressed that they forgot to take ECs. This is inconsistent with other studies [41,42]. As to whether the respondents had utilized ECs before, nearly half indicated in the affirmative. This outcome supports that of several studies executed in different settings [10,28,34,43]. But it is in variance with similar studies by [8,26,37,44,45] on ECs utilization. It could be inferred that most of the respondents encounter some form of obstacles that impede them from utilizing ECs. Again, there may be limited availability of reproductive health and family planning services or lack of education and promotion in comprehensive education package. Similarly, higher proportion of the study participants were able to identify the efficacy rates of ECs which is in agreement with similar works from [8,15,16]. It is likely they have chanced on relevant information on the efficacy of ECs from publications or advertisements. On the perceptions of the barriers that obstruct the utilization of ECs, the respondents recounted the fear of being seen by others (stigma), ECs cause abortions, religious disapprovals and unavailability of ECs as their major challenges. These perceptions are not different from those discovered in a similar study carried out among university students in Kilimanjaro Tanzania, and other settings that mentioned the fear of side effects, religious unacceptability and the fear of being seen by others (stigmatization) [29,46,47]. This could be attributed to the perceived societal unacceptability of ECs and inadequate information on the benefits of ECs to encourage the public to uptake ECs.
Furthermore, our finding identified that, being less than thirty years old was a determinant of poorer knowledge level on ECs. This is in line with other studies by [6,26,47,48]. But similar studies are in variance with our fallouts [49,50]. Level of education (year of study) was found to be associated with poor knowledge on ECs. This is consistent with [5,47,49]. However, it is inconsistent with a similar study conducted among Portuguese female users of healthcare services on ECs [29]. Residence was a predictor to poor knowledge level on ECs. This finding from our study is in line with that of [50]. Respondents who were health sciences students had a slight poor knowledge level on ECs as against their non-health sciences counterparts. This is inconsistent with a different study from [30]. This may be probably because they were health sciences students there was perceived high expectations from them to have known better on ECs or may be their sources of information on ECs misled them. Participants who were co-habiting had a slight better knowledge on ECs as compared to those married. This outcome from our study is inconsistent with a different work which reported that being single makes one have better knowledge level on ECs [37]. This could be attributed to the perceptions that individuals co-habiting may be careful in preventing unwanted pregnancy and so may be much interested in utilizing or knowing more about the relevance of ECs. Participants who practiced traditional religion had absolutely poor knowledge on ECs. The inference is that, traditionalists may have several forms of preventions against unwanted pregnancies using traditional methods, hence, no need for them to avert their attentions to ECs and their utilizations.
Limitation: questions that had sensitive nature like whether one had ever had protected or unprotected sexual intercourse might produce social desirability bias.
Emergency contraceptive utilization among female tertiary students is low and reproductive health and family planning services, education and promotion initiatives should be tailored towards the utilizations of ECs and their consequential benefits to the user, the society and the nation at large. It is relevant to address the obstacles impeding the users of ECs in utilizing the products; and the information provided on ECs through the various media outlets must be scientifically justified to demystify all forms of misconceptions regarding them. Extensive engagements should be encouraged and all stakeholders should be involved in health promotion activities directed towards improving ECs and their utilizations among the sexually active youth as part of the package of holistic reproductive health in tertiary educational institutions. Again, these health promotion campaigns should make room for people in this age group who are out of tertiary schools. This could improve the knowledge and utilizations of ECs among females in the reproductive age (15 - 49) who are still in or out of tertiary schools. It is also recommended that governments, donors, and the non-governmental sectors should focus on meeting the need for ECs to meet the reproductive health needs of females of reproductive age.
What is known about this topic
- EC is an option to explore after a regular contraceptive has failed, to prevent unintentional pregnancy or after sexual assault;
- EC is not to be used as a regular contraceptive method to be applied on regular basis;
- EC play significant role in alleviating the global increase in unintended pregnancies, abortions and dangerous reproductive health complications.
What this study adds
- The fear of being seen by others when patronizing ECs remains a major barrier to ECs utilization (stigma);
- � The proportion of health sciences students who had poor knowledge level on ECs were slightly higher as compared to their three colleagues� non-health sciences students;
- Respondents affiliated to traditional religion had 100% poor knowledge on ECs.
The authors declare no competing interests.
Mustapha Hallidu conceived the idea, designed the questionnaire, gathered the data and drafted the manuscript. Data analysis was carried out by Issah Sumaila. All authors contributed intellectually, proofread and approved the final version of the manuscript.
We express our profound appreciations to all participants who willingly agreed to participate in this study. All authors have read and agreed to the final manuscript.
Table 1: socio-demographic characteristics of respondents recruited from the Middle Belt of Ghana from March, 2021 to April, 2022 (N=535)
Table 2: knowledge of the respondents recruited from the Middle Belt of Ghana from March, 2021 to April, 2022 (N=535) on emergency contraceptives
Table 3: respondents recruited from the Middle Belt of Ghana from March, 2021 to April, 2022 (N=535) sexual activities and utilization of emergency contraceptives
Table 4: association of socio-demographic characteristic of respondents recruited from the Belt of Ghana from March, 2021 to April, 2022 with knowledge on emergency contraceptives
- Otobo DD, Adefila J, Mesak D. Knowledge, attitude, perception and utilization of contraceptive amongst reproductive aged adults at the Ghent University Summer School, Belgium: a cross-sectional study. Int J Clin Obstet Gynaecol. 2022;6(1):14-7. Google Scholar
- Kotb MAM, Ragab HM, Elwan YA, Hussein YHH. Oral contraceptive pills use and adverse effects. Egypt J Hosp Med. 2022;86(1):286-90. Google Scholar
- Mamuye SA, Gelaye Wudineh K, Nibret Belay A, Gizachew KD. Assessment of knowledge, attitudes, and practices regarding emergency-contraception methods among female Dangila Hidase high school students, Northwest Ethiopia, 2019. Open Access J Contracept. 2021;12:1-5. PubMed | Google Scholar
- Abera L, Sema A, Guta A, Belay Y. Emergency contraceptive utilization and associated factors among college students in Dire Dawa City, Eastern Ethiopia: a cross-sectional study. Eur J Midwifery. 2021 Jul 16;5:28. PubMed | Google Scholar
- Leon-Larios F, Ruiz-Ferron C, Jalon-Neira RM, Praena-Fernández JM. Nursing students´ knowledge, awareness, and experiences of emergency contraception pills´ use. J Clin Med. 2022 Jan 14;11(2):418. PubMed | Google Scholar
- Fikadu K. Utilization and associated factors of emergency contraception among female college students in Addis Ababa, Ethiopia. Qual Prim Care. 2021;29(1):1-07. Google Scholar
- Evidence T. International Consortium for Emergency Contraception (ICEC) International Federation of Gynecology & Obstetrics (FIGO). How do levonorgestrel-only emergency contraceptive pills (LNG ECPs) prevent pregnancy. Levonorgestrel-only emergency contraceptiv. 2008;(October):18-9.
- Yeboah DS, Appiah MA, Kampitib GB. Factors influencing the use of emergency contraceptives among reproductive age women in the Kwadaso Municipality, Ghana. PLoS One. 2022;17(3):e0264619. PubMed | Google Scholar
- Seidu AA, Ameyaw EK, Ahinkorah BO, Baatiema L, Dery S, Ankomah A et al. Sexual and reproductive health education and its association with ever use of contraception: a cross-sectional study among women in urban slums, Accra. Reprod Health. 2022;19(1):1-10. PubMed | Google Scholar
- Kwame KA, Bain LE, Manu E, Tarkang EE. Use and awareness of emergency contraceptives among women of reproductive age in sub-Saharan Africa: a scoping review. Contracept Reprod Med. 2022;7(1):1-14. PubMed | Google Scholar
- Barchi F, Ntshebe O, Apps H, Ramaphane P. Contraceptive literacy among school-going adolescents in Botswana. Int Nurs Rev. 2022;69(1):86-95. PubMed | Google Scholar
- Tenaw LA. Practice and determinants of emergency contraceptive utilization among women seeking termination of pregnancy in Northwest Ethiopia-a mixed quantitative and qualitative study. PLoS One. 2022;17(2 February 2022):1-10. PubMed | Google Scholar
- Numanovich AI, Abbosxonovich MA. Prevalence of contraceptive use among Kenya coast National Polytechnic students. EPRA Int J Multidiscip Res (IJMR)-Peer Rev J. 2020;(2):198-210. Google Scholar
- Baa-Nyarkoh E. Emergency contraception use among female students at the Accra Technical University. 2019;(10388417):77. Google Scholar
- Capri E, Group W. Emergency contraception. Widely available and effective but disappointing as a public health intervention?: a review. Human reproduction. 2015;30(4):751-60. Google Scholar
- Thomas Jefferson University. Contraception for PCPs 2021. Accesssed Jun 11, 2022.
- Jiménez-Iglesias A, Moreno C, García-Moya I, Rivera F. Prevalence of emergency contraceptive pill use among Spanish adolescent girls and their family and psychological profiles. BMC Womens Health. 2018;18(1):1-8. Google Scholar
- Martínez JL, Vicario-Molina I, González E, Ilabaca P. Sex education in Spain: the relevance of teachers´ training and attitudes/educación sexual en España: importancia de la formación y las actitudes del profesorado. Infanc y Aprendiz. 2014;37(1):117-48. Google Scholar
- Morales A, Espada JP, Orgilés M. A 1-year follow-up evaluation of a sexual-health education program for Spanish adolescents compared with a well-established program. Eur J Public Health. 2016;26(1):35-41. PubMed | Google Scholar
- Amengual M de LB, Canto ME, Berenguer IP, Pol MI. Revis�o sistemática do perfil de usuárias de contracepç�o de emergência. Rev Lat Am Enfermagem. 2016;24. Google Scholar
- Mutaru A-M, Asumah M, Ibrahim M, Sumaila I, Hallidu M, Mbemah J et al. Knowledge on sexually transmitted infections (STIs) and sexual practices among Nursing Trainees in Yendi Municipality, Northern Region of Ghana. Eur J Heal Sci. 2021;6(4):33-47. Google Scholar
- Tejada J, Punzalan J. On the misuse of Slovin´s formula. Philipp Stat. 2012;61(1):129-36. Google Scholar
- Jima A, Segni MT, Zergaw A. Assessment of knowledge, attitude and utilization of emergency contraception among unmarried women of reproductive age in Adama, Ethiopia. Heal Sci J. 2017;10(6). Google Scholar
- World Medical Association. Declaration of Helsinki, ethical principles for scientific requirements and research protocols. Bull World Health Organ. 2013;79(4):373.
- Issah H, Salifu A, Awal I. Knowledge of contraceptives, knowledge of types, and identified challenges to contraceptives use among undergraduate nursing students in the University for Development Studies. OALib. 2022;09(03):1-15. Google Scholar
- Mishore KM, Woldemariam AD, Huluka SA. Emergency contraceptives: knowledge and practice towards Its use among Ethiopian female college graduating students. Int J Reprod Med. 2019 Jan 1;2019:9397876. PubMed | Google Scholar
- Nwankwo B, Mohammed M, Usman N, Olorukooba A. Knowledge, attitude and practice of emergency contraception among students of a tertiary institution in Northwestern Nigeria. J Med Basic Sci Res. 2021;2(1):13-28. Google Scholar
- Mbuya EJ, Mkojera EJ, Amour C, Mboya I, Msuya SE. Knowledge, practice and barrier towards emergence contraceptive usage among female University Students at Kilimanjaro Region in Tanzania. 2022;1-14. Google Scholar
- Rodrigues Â, Valentim B, Tavares D, Augusto MJ, Campelo J, Loureiro M et al. Knowledge and patterns of use of emergency oral contraception among Portuguese female users of healthcare services. Acta Med Port. 2021;34(13):30-5. PubMed | Google Scholar
- Kongnyuy EJ, Ngassa P, Fomulu N, Wiysonge CS, Kouam L, Doh AS. A survey of knowledge, attitudes and practice of emergency contraception among university students in Cameroon. BMC Emerg Med. 2007 Jul 17;7:7. PubMed | Google Scholar
- Gonsalves L, Wyss K, Gichangi P, Hilber AM. Pharmacists as youth-friendly service providers: documenting condom and emergency contraception dispensing in Kenya. Int J Public Health. 2020;65(4):487-96. PubMed | Google Scholar
- Mohammed S, Abdulai A-M, Iddrisu OA. Pre-service knowledge, perception, and use of emergency contraception among future healthcare providers in northern Ghana. Contracept Reprod Med. 2019;4(1):1-7. PubMed | Google Scholar
- Audu BM, Kawuwa MB, Mana A, Peter A. Knowledge, attitude and practice of emergency contraception amongst healthcare workers in Idp camps and host community clinics in Jere and Maiduguri Metropolitan Local Government Areas, Borno State. Kanem J Med Sci. 2021;15(1):27-34. Google Scholar
- Feyissa A. Assessment of knowledge, attitude and practice towards emergency contraceptive methods among female students in Abdisa Aga High School, Fiche Town, Northern. International Journal of Chinese Medicine. 2017;1(1):16-23. Google Scholar
- Tamire W, Enqueselassie F. Knowledge, attitude, and practice on emergency contraceptives among female university students in Addis. 1950. Google Scholar
- Ajayi AI, Nwokocha EE, Adeniyi OV, Ter Goon D, Akpan W. Unplanned pregnancy-risks and use of emergency contraception: a survey of two Nigerian Universities. BMC Health Serv Res. 2017;17(1):1-8. PubMed | Google Scholar
- Feleke AE, Nigussie TS, Debele TZ. Utilization and associated factors of emergency contraception among women seeking abortion services in health institutions of Dessie town, North East Ethiopia, 2018. BMC Res Notes. 2019;12(1):4-9. PubMed | Google Scholar
- Nachinab GT. Utilisation of emergency contraception among final year university female students introduction. 2021. Google Scholar
- Aziz Ali S, Aziz Ali S, Feroz A, Saleem S, Fatmai Z, Kadir MM. Factors affecting the utilization of antenatal care among married women of reproductive age in the rural Thatta, Pakistan: Findings from a community-based case-control study. BMC Pregnancy Childbirth. 2020 Jun 10;20(1):355. PubMed | Google Scholar
- Naghavi M, Abajobir AA, Abbafati C, Abbas KM, Abd-Allah F, Abera SF et al. Global, regional, and national age-sex specifc mortality for 264 causes of death, 1980-2016: a systematic analysis for the global burden of disease study 2016. Lancet. 2017;390(10100):1151-210. PubMed | Google Scholar
- JTD, LY. Knowledge, attitude and practice of emergency contraceptive among undergraduate female college students: a cross-sectional study. Austin J Obstet Gynecol. 2021;8(5). Google Scholar
- Karim SI, Irfan F, Saad H, Alqhtani M, Alsharhan A, Alzhrani A et al. Men´s knowledge, attitude, and barriers towards emergency contraception: a facility based cross-sectional study at King Saud University Medical City. PLoS One. 2021;16(4 April):1-19. Google Scholar
- Nagendran PS, Godakandage SP. Prevalence of unplanned pregnancies and their family planning preferences among antenatal clinic attendees in Thimbirigasyaya Divisional Secretariat Division. Sri Lanka J Obstet Gynaecol. 2021;43(3):144. Google Scholar
- Barbian J, Kubo CY, Balaguer CS, Klockner J, Costa LMV da, Ries EF et al. Emergency contraception in university students: prevalence of use and knowledge gaps. Rev Saude Publica. 2021;55:74. PubMed | Google Scholar
- Ofogba LE, Adeyemo F, Agofure O. Perceived barriers influencing uptake of contraceptives among female undergraduates in a Nigerian University. 2022;25(2010). Google Scholar
- Chan MC, Munro S, Schummers L, Albert A, Mackenzie F, Soon JA et al. Dispensing and practice use patterns, facilitators and barriers for uptake of ulipristal acetate emergency contraception in British Columbia: a mixed-methods study. C open. 2021;9(4):E1097-104. PubMed | Google Scholar
- Abdulai A-M. Determinants of EC utilization among the youth in the Tamale Municipality - a cross-sectional study. Texila Int J Public Heal. 2021;9(1):113-7. Google Scholar
- Tesfaw A, Berihun H, Molla E, Mihret G, Feleke DG, Chanie ES et al. Level of knowledge and practice of female healthcare providers about early detection methods of breast cancer at Debre Tabor Comprehensive Specialised Hospital: a cross-sectional study. Ecancermedical science. 2021 Jul 19;15:1268. PubMed | Google Scholar
- Sreedevi A, Vijayakumar K, Najeeb SS, Menon V, Mathew MM, Aravindan L et al. Pattern of contraceptive use, determinants and fertility intentions among tribal women in Kerala, India: a cross-sectional study. BMJ Open. 2022;12(4):e055325. PubMed | Google Scholar
- Ezenwaka U, Mbachu C, Okeke C, Agu I, Ezumah N, Onwujekwe O. Socio-demographic and economic determinants of awareness and use of contraceptives among adolescents in Ebonyi State, South-east, Nigeria The sexual and reproductive behaviours of Study setting and study design. Afr J Reprod Health. 2021;25(3):21-9. Google Scholar




