Assessment of COVID-19 vaccination-related knowledge, attitude and barriers among healthcare professionals working at governmental hospitals in South Gondar Zone, Ethiopia
Teklie Mengie Ayele, Endeshaw Chekol Abebe, Zelalem Tilahun Muche, Melaku Mekonnen Agidew, Yohannes Shumet Yimer, Getu Tesfaw Addis, Nega Dagnaw Baye, Achenef Bogale Kassie, Muluken Adela Alemu, Tesfagegn Gobezie Yiblet, Gebrehiwot Ayalew Tiruneh, Samuel Berihun Dagnew
Corresponding author: Teklie Mengie Ayele, Department of pharmacy, College of Health Sciences, Debre Tabor University, Debre Tabor, Ethiopia 
Received: 30 Jul 2022 - Accepted: 22 Oct 2022 - Published: 26 Oct 2022
Domain: Medicinal chemistry, Pharmacology, Toxicology
Keywords: Attitude, barriers, COVID-19 vaccine, health care professionals, knowledge
©Teklie Mengie Ayele et al. PAMJ-One Health (ISSN: 2707-2800). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Teklie Mengie Ayele et al. Assessment of COVID-19 vaccination-related knowledge, attitude and barriers among healthcare professionals working at governmental hospitals in South Gondar Zone, Ethiopia. PAMJ-One Health. 2022;9:15. [doi: 10.11604/pamj-oh.2022.9.15.36583]
Available online at: https://www.one-health.panafrican-med-journal.com/content/article/9/15/full
Research 
Assessment of COVID-19 vaccination-related knowledge, attitude and barriers among healthcare professionals working at governmental hospitals in South Gondar Zone, Ethiopia
Assessment of COVID-19 vaccination related knowledge, attitude and barriers among health care professionals working at governmental hospitals in South Gondar Zone, Ethiopia
![]() Teklie Mengie Ayele1,&,
Teklie Mengie Ayele1,&, ![]() Endeshaw Chekol Abebe2,
Endeshaw Chekol Abebe2, ![]() Zelalem Tilahun Muche3, Melaku Mekonnen Agidew2, Yohannes Shumet Yimer1, Getu Tesfaw Addis1,
Zelalem Tilahun Muche3, Melaku Mekonnen Agidew2, Yohannes Shumet Yimer1, Getu Tesfaw Addis1, ![]() Nega Dagnaw Baye4, Achenef Bogale Kassie1, Muluken Adela Alemu1, Tesfagegn Gobezie Yiblet1,
Nega Dagnaw Baye4, Achenef Bogale Kassie1, Muluken Adela Alemu1, Tesfagegn Gobezie Yiblet1, ![]() Gebrehiwot Ayalew Tiruneh5,
Gebrehiwot Ayalew Tiruneh5, ![]() Samuel Berihun Dagnew1
Samuel Berihun Dagnew1
&Corresponding author
Introduction: with COVID-19 vaccines being developed concurrently, it is clear that inadequate knowledge and poor attitudes among communities around the world provide a significant obstacle and continue to prevent the complete population from being immunized against highly contagious illnesses. The study's objective was to evaluate the knowledge, attitude, and barriers that healthcare professionals have towards the COVID-19 vaccine.
Methods: a descriptive cross-sectional study was conducted through a self-administered questionnaire that was disseminated to health care professionals working in the South Gondar zone hospitals, in South Gondar Zone, Ethiopia. SPSS Statistics Version 25 was used to enter and evaluate the data that were gathered. To ascertain the relationship between independent and outcome variables, binary logistic analysis was performed.
Results: a total of 450 respondents participated in the survey, and 90% of them completed and returned. The majority of the participants (94.44%) were aware of the COVID-19 vaccination. More than half of them (56.22%) had experience with COVID-19 treatment, and 54.7% had sufficient knowledge about COVID-19 immunization. The importance of the vaccine in maintaining population COVID-19 immunization coverage and in reducing COVID-19 incidence to prevent the onset of new epidemics, respectively, was positively viewed by more than two-thirds (74.43%) and 84.4% of the respondents, respectively. Furthermore, only 6.6% of respondents approved of pharmaceutical companies' advertising of the COVID-19 vaccine.
Conclusion: according to the current study, healthcare professionals had a promising view of COVID-19 immunization. However, the overall percentage of positive responses to the attitude questions was only 48.34%. Additionally, more than 76.67% of the respondents reported that if the community does not receive the COVID-19 vaccination, the incidence of the virus will greatly grow. However, only about half of the respondents had adequate knowledge about the COVID-19 vaccination.
A significant cause of morbidity and mortality in the general population is vaccine-preventable illnesses. Vaccinations are widely acknowledged as one of the most effective public health preventive strategies [1]. Globally, the COVID-19 pandemic is posing a threat to the lives of billions of people. Several vaccines are now being developed in laboratories using various sources, such as antibodies and small-molecule medicines. Around the world, this epidemic has had a substantial impact on the economy, human health, and lifestyle choices [2,3]. The most effective way to stop the spread of COVID-19 is to employ several vaccines that are both safe and effective. The Food and Drug Administration (FDA) has authorized the use of the vaccine for emergency purposes, and the vaccine-producing companies are anticipated to provide it [4]. Global demand for an efficient vaccine increases as long as the COVID-19 pandemic's disruptions continue [5]. Additionally, vaccines are prioritized for special populations due to concerns over the monopolization of COVID-19 vaccine supply and distribution by a few developed countries as a result of the vaccine's high production costs, which cannot be covered by low- and middle-income countries [6]. Vaccine hesitation; the refusal, delay, or acceptance of vaccination when there are concerns about its efficacy and safety [7]; as a problem that may have arisen due to several circumstances. Poor vaccination quality, doubts about dosage, religious restrictions, and suspicions about the existence of the live virus in the immunizations are a few of these [8]. According to a study done in Egypt, vaccine hesitancy is widespread among health care professionals and is a serious obstacle to public vaccination acceptance. This study also suggests the urgent need to launch programs to raise public understanding of the value of vaccinations so that they can be expected [9]. For the COVID-19 vaccine, for instance, health care professional education should be given top attention [10].
Individual preference for various COVID-19 vaccines has also been noted in different countries [11]. These findings can serve to influence the planning and development of future public health measures that could boost the acceptance of a COVID-19 vaccination [12]. Therefore, building long-term public trust demands creating effective and efficient intervention mechanisms. Additionally, groups at risk of refusing vaccinations should be the focus of international awareness initiatives [13,14]. When a COVID-19 vaccine is made available, this may aid vaccination awareness campaigns in addressing vaccine doubt. Public trust in the creation, administration, distribution, and promotion of an efficient COVID-19 vaccination The attitudes' of health care proffessionals like the efficiency of the vaccine, the place where it was designed, the kind of vaccine, and the timing of the vaccine production process is highly important [15]. Additionally, attitudes and knowlegde on the dosage and vaccine safety are among the major factors in determining whether a health care professional will embrace the COVID-19 vaccine [16]. Not only the COVID-19 can have detrimental health consequences, but also the poor vaccine interest among health care professionals may negatively affect the quality of life of the population at large [17]. Furthermore, inadvertent administration of numerous doses of the COVID-19 vaccination has also increased public refusals. Multiple doses of the COVID-19 vaccine were seen to cause both local and systemic responses, according to reports from preliminary investigations [18]. A poor level of knowledge has been implicated in the rapid spread of the infection in health facilities and delay of treatment, and may put patients' lives at risk [19]. In most nations, immunization against COVID-19 is optional, thus it's critical to comprehend the present attitudes of the local people before the vaccine program is implemented. However, no research is currently being done in Ethiopia about the attitudes, knowledge, and barriers that healthcare workers have toward the COVID-19 vaccine. The findings may be helpful in suggesting any corrective actions and further interventions in the research region to enhance awareness, attitude, and barriers among healthcare workers.
Study design, setting and period: in this multi-institution-based descriptive cross-sectional study, a self-administered questionnaire was disseminated to health care professionals working in government hospitals in South Gondar zone, Northern West Ethiopia. Data were collected for one month (from February 30, 2022 to March 30, 2022).
Eligibility criteria: only the full-time health care professionals who are available during the data collection period and who are ready to take part in the study were included.
Variables: the independent variables were included in the sociodemographic characterstics (age, sex, proffesion, level of education, and work experience of the health care proffesionals). The dependent variables were the questions or statemets that describe the knowledge, attitude and barrires of COVID-19 vaccination among the health care proffesionals.
Sample size and sampling technique: a single population proportion formula was used to calculate the sample size as follows [20].
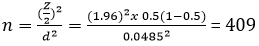
Where n = sample size required; z = standard normal variable at 95% confidence level (1.96); p = population proportion (0.5); d = margin of error (0.0485). With 10% contingency (409*0.1=40.9); the final sample size for this study was (40.9+409) 450. Simple random sampling techniques were used to select the study subjects after proportional allocation of study subjects to each hospital (Figure 1).
Data resource and measurement
Data collection tool: after reviewing pertinent literatures, we adapted an existing pretested structured questionnaire and produced it. Four components made up the questionnaire, which was created by the researchers and covered sociodemographic variables, knowledge, attitude, and barriers.
Control of data quality: external specialists in the subject evaluated the validity of the questionnaire. Surveys were also employed to examine the internal validity of the inquiries in each section of the questionnaire.
Data analysis: the data were entered and analyzed using SPSS Statistics version 25 after being checked for accuracy. In order to depict knowledge, attitude, and barriers linked to COVID-19 vaccination, frequency and percentage were utilized. Participants' knowledge was further classified as adequate if they properly answered every knowledge question and inadequate if they answered one or more of them wrong [21]. To determine any potential relationships between the dependent and independent variables, binary logistic regression was performed. Statistical significance was defined as a p-value of 0.05 or lower. The attitudes of the respondents were assessed using 5-point Likert-type questions. The percentage of positive responses (PPR) used to gauge response rates and the average attitude score were both computed. Using the t-test and one-way ANOVA, the attitudes of the various responder groups were compared. Calculations were made on the frequency and percentage of responses to each COVID-19 vaccine-related barrier.
Ethical considerations: the ethical review board of the college of health science at Debre Tabor University provided a letter of ethical approval. The Declaration of Helsinki's rules were followed. Before the survey, each survey participant gave their written informed consent. Additionally, no personal information about study participants, such as their names or addresses, was included in the data obtained, and data confidentiality was maintained.
Sociodemographic characteristics: a response rate of 90% was achieved with the return of 450 fully completed and signed questionnaires. The average age of the respondents was 31.4 ± 6.2 years, and 54.00% of them were between the ages of 18 and 28. About half of the respondents (57.33 percent) were followers of the orthodox religion, while more than half (70.44%) of the respondents were men. Physicians made up about a third (34%) of the population, and nearly half (47.33%) had five to ten years of employment experience (Table 1).
Knowledge towards COVID-19 vaccination: almost all the participants (94.44%) claimed to be aware of the COVID-19 vaccination. The majority of participants acknowledged the media as a source of information on the COVID-19 vaccine (Table 2). The majority of respondents had no personal or family history of COVID-19 exposure, while more than half (56.22%) admitted to having previously been involved in COVID-19 care. More over two-thirds of respondents (77.78%) said they have received vaccinations at some point in their lives, and the majority of respondents (86.89%) agreed that COVID-19 vaccination should not be required. The majority of respondents (72.00%) reported that they had experienced vaccine side effects, and they were afraid of the recently discovered COVID-19 vaccine side effects. Meanwhile, 53.33% of participants said the scientific evidence at this time does not sufficiently support the link between COVID-19 vaccines and chronic illnesses. More than 76.67% of respondents also said that if the community does not receive the COVID-19 vaccine, the incidence of the virus will increase significantly. Nearly all (92.67%) respondents said that everyone in the community should adhere to the COVID-19 preventive protocols and that the COVID-19 pandemic can be eradicated with vaccination. More than two thirds (79.78%) of participants agreed that people who had recovered from COVID-19 should get the vaccine, and more than half (55.56%) agreed that people with chronic illnesses needed to get the COVID-19 vaccine. Nearly all (96.67%) of the study participants stated that everyone has to receive 2 doses of the COVID-19 vaccine and that the second dosage should be administered 28 days following the first dose (76.67%) (Table 3). Binary logistic analysis was used to find the determinants of the amount of knowledge across participants, after we categorized knowledge based on knowledge score as adequate (right answers for all knowledge questions) or inadequate (at least one inaccurate response). As a result, participants' age, profession, amount of education, and work experience were discovered to be predictive of how much they knew about COVID-19. Compared to pharmacists, nurses, and other professionals, physicians were more likely to have the adequate knowledge (AOR: 1.25 CI: 0.43, 0.72). Additionally, the odd of having adequate knowledge was higher among Master´s Degree holders (AOR 2.43 CI: 0.47, 9.54) compared with respondents having other level of education. The odd of having adequate knowledge was higher in respondents above 40 years of old compared with other age groups (AOR 1.09 CI: 0.26, 4.53). Compared to those who served for 5 years or less, those with five to ten years of service were more likely to have adequate understanding of COVID-19 vaccination (AOR: 2.22; CI 1.21, 3.81 (Table 3).
Attitude towards COVID-19 vaccination: among those surveyed, 84.44% agreed that it is impossible to prevent COVID-19 without vaccination, while 77.10% said they would encourage others to do the same, and 74% said it is crucial to maintain the population's COVID-19 vaccination coverage in order to prevent the emergence of new epidemics. The majority of respondents, 69.11%, concur that government officials have the authority to require everyone to receive the COVID-19 immunization. Only 7.55% of respondents believed that COVID-19 vaccines are completely effective and have undergone enough safety and effectiveness testing. The overall percentage of positive response to the attitude questions was 48.34% (Table 4). Change in attitude scores across groups of study respondents was assessed by t-test. Consequently, there was significance difference in sex (p<0.05) between female [mean score = 1.48] and male [means score = 2.93] respondents; physician [mean score = 0.98] and pharmacists [means score = 2.99]; nurse [mean score = 3.25] and specialist [mean score = 1.54]; masters [mean score = 0.96] and bachelor [mean score = 2.67]. Likewise, the results from one way ANOVA showed that there was significant difference (p<0.05) across different classes of age group and working experience.
Barrier related to COVID-19 vaccination: the majority of responders (89.11%) did not think the COVID-19 vaccination would halt the pandemic, and 80.67% said they did not need it because they already practiced all preventive measures. Only 58.44% of respondents said that the COVID-19 vaccination was a conspiracy, which is why the vaccine campaign is hampered. In addition, 75.56% of the respondents claimed that whether their family or acquaintances received the COVID-19 immunization had no bearing on them. 51.11% of respondents said that we could start taking vaccines via a different route of administration than injection (Table 5).
According to reports from WHO and Europe, COVID-19 vaccinations have not been associated with any significant safety or effectiveness problems. Therefore, in order to increase vaccination coverage, immunization programs should be created to eliminate obstacles related to the cost and accessibility of vaccines. Additionally, health education and communication from reliable sources are crucial for allaying public concerns about vaccine safety belief [22]. Therefore, developing strategies to offer evidence-based information on the COVID-19 vaccine, such as creating leaflets and white papers, as well as quality control and quality assurance, and combating fake news, are essential for raising public awareness of the vaccine before it is administered to the public [23]. For instance, those with a history of vaccination have shown to comprehend and value the COVID-19 vaccine [15]. To protect themselves from this disease, the majority of Ethiopians rely on natural immunity, herd immunity, and natural home remedies including garlic, vitamins, steam inhalations, and hot water gargling. Their findings are important for providing the public with reliable health information on a variety of platforms. The most effective way to stop the spread of COVID-19 is to employ several vaccines that are both safe and effective. The creation of a revolutionary COVID-19 vaccine appears to be a daunting task. In order to quickly control the disease's spread, the COVID-19 pandemic has made healthcare organizations implement unprecedented infection prevention and control procedures. The latter is a crucial strategy to stop the COVID-19 epidemic from spreading further, and might well change everything as the globe fights the worst fitness catastrophe of the century. There are now over 100 candidates for the COVID-19 vaccine that are in various phases of clinical testing. Through emergency uses authorization (EUA) from their associated health ministry or branch, many countries accelerated the use of the COVID-19 vaccination to the public.
In order to understand the epidemiological dynamics of disease prevention and to ensure the effectiveness, adherence, and success of the immunization program, healthcare workers' knowledge, attitudes, and barriers regarding the COVID-19 vaccine must be taken into consideration. Even with previously established vaccination programs, vaccine resistance continues to be a major obstacle to comprehensive population immunization. We discovered that nearly half of the responders were between the ages of 18 and 28, and nearly half had sufficient knowledge. According to the study, more than half of the respondents were men and had sufficient understanding about the COVID vaccine. When compared to respondents from other professions, the current study also indicated that more than half of physicians were aware of the COVID-19 vaccination, and more than two-thirds of respondents had master's degrees. According to a cross-sectional survey from Jordan by Tamam et al. 66.5% of the respondents agreed or strongly agreed that the vaccination is essential for protecting people against the COVID-19 pandemic [24]. According to a study from the USA by Ada et al. the majority of medical professionals have expressed worries about the COVID-19 vaccine, and roughly 66.5% of the respondents plan to delay the vaccination [25]. More over half (57.5%) of healthcare personnel, according to a different research from Maryland, USA, intended to obtain the COVID-19 vaccine [26]. Moreover, there was a statistically significant difference in respondents' sexes, professional statuses, and levels of education, according to a study in Italy that revealed 75% of healthcare professionals wanted to get immunized against COVID-19 [27]. The findings from these reports are consistent with the current investigation.
According to a study conducted in France, Belgium, and portions of Canada that speak French, 79.6 percent of healthcare professionals there would probably advise COVID-19 immunization to their clients and colleagues, and 72.4% of them would unquestionably agree to get it [28]. However, a study carried out in Saudi Arabia by Mazin et al. found that female health care professionals under the age of 40 were more likely to have low levels of knowledge and a negative attitude toward the COVID-19 immunization [29]. This finding also supports our investigation. In addition, a study by Khan Sharun et al. found that while 86.3% of respondents from the public planned to receive the COVID-19 immunization, 13.7% expressed hesitancy due to a number of obstacles. However, only 65.8% of participants said they will get vaccinated as soon as feasible whenever the vaccine is available [30]. Another study from Romania by Padureanu et al. shown that nurses have a more positive attitude about the COVID-19 vaccination [31]. However, research by Alle and Oumer revealed that 64.7 and 66.7%, respectively, of doctors and pharmacists had a high level of attitude toward the COVID-19 vaccination [32]. Additionally, a paper that combined data from several study regions among medical professionals revealed that more than 50% of respondents had a favorable opinion toward the COVID-19 vaccination [33]. Older age, male gender, and being a physician were predictors of healthcare workers' favorable attitudes of the COVID-19 vaccination [26,34]. According to several studies, the level of education has a considerable impact on the attitudes and knowledge of medical professionals toward the COVID-19 vaccination [7,35,36]. These reports are consistent with our investigation, which examined the aforementioned predictors.
Some health professionals are disappointed because their religious beliefs conflict with the belief that receiving the COVID-19 vaccine will protect them against pandemics, thus they choose not to do so and forego the inoculation [37]. In our study, 56.2% of participants were doctors with sufficient understanding about COVID-19 immunization. A prior survey found that 87.5% of respondents were physicians and thought that finding an effective solution would help to lower the likelihood of the COVID-19 pandemic [38]. Additionally, another study from Israel found that age and occupation were strongly related to tendency to receive the vaccine, supporting the need for health care providers to have enough information [39]. According to findings from a prior research, 56% of the respondents said that they had not had the COVID-19 immunization for one reason or another [40]. Healthcare professionals' reasons for not vaccinating against COVID-19 included worries about vaccine safety, intramuscular injection as the route of delivery, efficacy, and mistrust of the government [34]. Furthermore, a survey conducted by medical professionals in Egypt found that the main obstacles to receiving the COVID-19 vaccine were a lack of knowledge about the vaccine's safety and effectiveness, which accounted for 96.8 and 93.2% of the respondents, respectively [41]. Concerns regarding vaccine availability (55%) future vaccine adverse effects (62%) rapid development (72%) pharmaceutical promotion for profit (2%) and a lack of societal trust are among the other important hurdles to COVID-19 vaccination that have been found by the report [42,43]. Finding from these report collectively support the findings from our report on barrier for healthcare professionals against COVID-19 vaccination.
The present study findings showed that respondents had a high level of knowledge on each individual feature of COVID-19 vaccination, but that only around half of respondents had sufficient understanding. Physicians tended to have a positive perspective about the value of vaccination and a negative attitude about pharmaceutical corporations' marketing-driven promotion of COVID-19 immunization. During the COVID-19 immunization campaign, barriers relating to the vaccines' efficacy, quick development, and lack of social trust had a considerable impact on the medical professionals. Additionally, boosting vaccine knowledge, changing attitudes, and removing barriers among medical professionals could enable them to provide a more effective vaccination program for the public.
What is known about this topic
- Regional variations in COVID-19 vaccination selection have also been documented by many nations, including Ethiopia. The public's acceptance of vaccination is hampered by the frequent vaccine reluctance expressed by healthcare providers.
What this study adds
- The degree of awareness and attitude in Ethiopia has been linked to the rapid spread of the virus in healthcare facilities, the delay in receiving treatment, and may even endanger the lives of patients. Additionally, COVID-19 vaccination barriers such a lack of public awareness, political subterfuge, religious beliefs, and the usage of conventional medicine were to blame for the low level of knowledge and negative attitude among medical professionals regarding the COVID-19 vaccine.
The authors declare no competing interests.
All authors made substantial contributions to conceptualization, data curation, formal analysis, investigation, methodology, project administration, resources, software, supervision, validation, visualization, writing the original draft; writing review and editing and gave final approval of the version to be published. All the authors have read and agreed to the final manuscript.
The authors thank the study participants for their cooperation during the data collection time. Moreover, we would like to extend our sincere thanks to South Gondar Zone Health Office staff for their valuable information. Finally, we are grateful to all research assistants.
Table 1: socio-demographic characteristics of study participants (n=450)
Table 2: COVID-19 vaccination related knowledge among Health care professionals working at governmental hospitals in South Gondar Zone, Ethiopia
Table 3 predictors of extent of knowledge about COVID-19 vaccination among health care professionals working at governmental hospitals in South Gondar zone hospitals, Ethiopia
Table 4: COVID-19 vaccination related attitude among health care professionals´ working at governmental hospitals in South Gondar Zone, Ethiopia
Table 5: barriers that hinder COVID-19 vaccination among health care professionals working at governmental hospitals in South Gondar Zone, Ethiopia
Figure 1: schematic presentation of the sampling procedure
- Andre FE, Booy R, Bock HL, Clemens J, Datta SK, John TJ et al. Vaccination greatly reduces disease, disability, death and inequity worldwide. Bull World Health Organ. 2008;86(2):140-6. PubMed | Google Scholar
- Kwok KO, Li KK, Wei WI, Tang A, Wong SYS, Lee SS. Influenza vaccine uptake, COVID-19 vaccination intention and vaccine hesitancy among nurses: a survey. Int J Nurs Stud. 2021;114:103854. PubMed | Google Scholar
- García LY, Cerda AA. Contingent assessment of the COVID-19 vaccine. Vaccine. 2020;38(34):5424-9. Google Scholar
- Mahase E. COVID-19: vaccine candidate may be more than 90% effective, interim results indicate. BMJ. 2020 Nov 9;371:m434. PubMed | Google Scholar
- Sharma O, Sultan AA, Ding H, Triggle CR. A review of the progress and challenges of developing a vaccine for COVID-19. Front Immunol. 2020 Oct 14;11:585354. PubMed | Google Scholar
- Yamey G, Schäferhoff M, Hatchett R, Pate M, Zhao F, McDade KK. Comment ensuring global access to COVID-19 vaccines. The Lancet. 2020;2019(20):2019-20. PubMed | Google Scholar
- Verger P, Dubé E. Restoring confidence in vaccines in the COVID-19 era. Expert Rev Vaccines. 2020;19(11):991-3. PubMed | Google Scholar
- Burki TK. The Russian vaccine for COVID-19. Lancet Respir Med. 2020;8(11):e85-6. PubMed | Google Scholar
- Hussein AA, Galal I, Makhlouf NA, Makhlouf HA, Abd-Elaal HK, Kholief Karima MS et al. A national survey of potential acceptance of COVID-19 vaccines in healthcare workers in Egypt. MedRxiv. 2021 Jan 1. Google Scholar
- Chuanxi F, Zheng W, Sen P, Shunping L, Xiaohui-Sun PL. Acceptance and preference for COVID-19 vaccination in health-care workers (HCWs) Chuanxi Fu. MedRxiv, 2020;2962(548). Google Scholar
- Gust DA, Darling N, Kennedy A, Schwartz B. Parents with doubts about vaccines: which vaccines and reasons why. Pediatrics. 2008;122(4):718-25. PubMed | Google Scholar
- Kreps S, Prasad S, Brownstein JS, Hswen Y, Garibaldi BT, Zhang B et al. Factors associated with US adults´ likelihood of accepting COVID-19 vaccination. JAMA Netw open. 2020;3(10):e2025594. PubMed | Google Scholar
- Dror AA, Eisenbach N, Taiber S, Morozov NG, Mizrachi M, Zigron A et al. Vaccine hesitancy: the next challenge in the fight against COVID-19. Eur J Epidemiol. 2020;35(8):775-9. PubMed | Google Scholar
- Leng A, Maitland E, Wang S, Nicholas S, Liu R, Wang J. Individual preferences for COVID-19 vaccination in China. Vaccine. 2021 Jan 8;39(2):247-254. PubMed | Google Scholar
- Redd DS, Jensen JL, Hughes SJ, Pogue K, Sloan-Aagard CD, Miner DS et al. Influences on attitudes regarding potential COVID-19 vaccination in the united states. Vaccines. 2020;8(4):1-14. PubMed | Google Scholar
- Karlsson LC, Soveri A, Lewandowsky S, Karlsson L, Karlsson H, Nolvi Set al. Fearing the disease or the vaccine: the case of COVID-19. Pers Individ Dif. 2021;172:110590. Google Scholar
- Padron-Regalado E. Vaccines for SARS-CoV-2: lessons from other coronavirus strains. Infect Dis Ther. 2020 Jun;9(2):255-274. PubMed | Google Scholar
- Folegatti PM, Ewer KJ, Aley PK, Angus B, Becker S, Belij-Rammerstorfer S et al. Safety and immunogenicity of the ChAdOx1 nCoV-19 vaccine against SARS-CoV-2: a preliminary report of a phase 1/2, single-blind, randomised controlled trial. Lancet. 2020 Aug 15;396(10249):467-478. PubMed | Google Scholar
- Hoffman SJ, Silverberg SL. Delays in global disease outbreak responses: lessons from H1N1, Ebola, and Zika. Am J Public Health. 2018;108(3):329-33. PubMed | Google Scholar
- Yousif W Wahed A, Mamdouh E, Mona H, Ahmed I. Assessment of knowledge, attitudes, and perception of health care workers regarding COVID-19, a cross-sectional study from Egypt. J Community Health. 2020 Dec;45(6):1242-1251. PubMed | Google Scholar
- Tesfaye ZT, Yismaw MB, Negash Z, Ayele AG. COVID-19-related knowledge, attitude and practice among hospital and community pharmacists in Addis Ababa, Ethiopia. Integrated Pharmacy Research & Practice. 2020;9:105. PubMed | Google Scholar
- Wang J, Jing R, Lai X, Zhang H, Lyu Y, Knoll MD et al. Acceptance of COVID-19 vaccination during the COVID-19 pandemic in china. Vaccines. 2020;8(3):1-14. PubMed | Google Scholar
- Rzymski P, Borkowski L, Drąg M, Flisiak R, Jemielity J, Krajewski J et al. The strategies to support the COVID-19 vaccination with evidence-based communication and tackling misinformation. Vaccines. 2021;9(2):1-9. PubMed | Google Scholar
- El-Elimat T, AbuAlSamen MM, Almomani BA, Al-Sawalha NA, Alali FQ. Acceptance and attitudes toward COVID-19 vaccines: a cross-sectional study from Jordan. PLoS One. 2021;(816):1. PubMed | Google Scholar
- Gadoth A, Halbrook M, Martin-Blais R, Gray A, Tobin NH, Ferbas KG et al. Assessment of COVID-19 vaccine acceptance among healthcare workers in Los Angeles. Ann Intern Med. 2021 Jun;174(6):882-885. PubMed | Google Scholar
- Shaw J, Stewart T, Anderson KB, Hanley S, Thomas SJ, Salmon DA et al. Assessment of US healthcare personnel attitudes towards coronavirus disease 2019 (COVID-19) vaccination in a large university healthcare system. Clin Infect Dis. 2021;73(10):1776-83. PubMed | Google Scholar
- Ledda C, Costantino C, Cuccia M, Maltezou HC, Rapisarda V. Attitudes of healthcare personnel towards vaccinations before and during the COVID-19 pandemic. Int J Environ Res Public Heal. 2021 Mar 8;18(5):2703. PubMed | Google Scholar
- Verger P, Scronias D, Dauby N, Adedzi KA, Gobert C, Bergeat M et al. Attitudes of healthcare workers towards COVID-19 vaccination: a survey in France and French-speaking parts of Belgium and Canada, 2020. Eurosurveillance. 2021 Jan;26(3):2002047. PubMed | Google Scholar
- Barry M, Temsah MH, Aljamaan F, Saddik B, Al-Eyadhy A, Alenezi S et al. COVID-19 vaccine uptake among healthcare workers in the fourth country to authorize BNT162b2 during the first month of rollout. Vaccine. 2021 Sep 24;39(40):5762-576. PubMed | Google Scholar
- Sharun K, Rahman CF, Haritha CV, Jose B, Tiwari R, Dhama K. COVID-19 vaccine acceptance: beliefs and barriers associated with vaccination among the general population in India. J Exp Biol Agric Sci. 2020 Jan 1;8(Spl-1-SARS-CoV-2):S210-8. Google Scholar
- Padureanu V, Bogdan M, Subtirelu MS, Padureanu R, Turcu-Stiolica A, Petrescu F et al. Perceptions of COVID-19 vaccination among healthcare professionals in Romania. Medical-Surgical Journal-Revista Medico-Chirurgicala. 2020;124(3):454-60. Google Scholar
- Alle YF, Oumer KE. Attitude and associated factors of COVID-19 vaccine acceptance among health professionals in Debre Tabor comprehensive specialized hospital, North Central Ethiopia; 2021: cross-sectional study. Virus Disease. 2021;32(2):272-8. PubMed | Google Scholar
- Hajure M, Tariku M, Bekele F, Abdu Z, Dule A, Mohammedhussein M et al. Attitude towards COVID-19 vaccination among healthcare workers: a systematic review. Infect Drug Resist. 2021;14:3883-97. PubMed | Google Scholar
- Li M, Luo Y, Watson R, Zheng Y, Ren J, Tang J et al. Healthcare workers´ (HCWs) attitudes and related factors towards COVID-19 vaccination: a rapid systematic review. Postgrad Med J. 2021;0:1-7. PubMed | Google Scholar
- Shekhar R, Sheikh AB, Upadhyay S, Singh M, Kottewar S, Mir H et al. COVID-19 vaccine acceptance among health care workers in the united states. Vaccines. 2021;9(2):1-18. PubMed | Google Scholar
- Elharake JA, Shafiq M, Cobanoglu A, Malik AA, Klotz M, Humphries JE et al. COVID-19 vaccine acceptance among health care workers in the kingdom of Saudi Arabia. Int J Infect Dis. 2021;109:286-93. PubMed | Google Scholar
- Muhamadi L, Edith N, James W, Museene SK, Peterson SS et al. Lack of trust, insufficient knowledge and risk denial; an in-depth understanding of health workers barriers to uptake of the COVID-19 vaccine at Iganga Hospital Eastern Uganda, and Mengo Hospital Kampala Uganda. medRxiv. 2021;1-19. Google Scholar
- Elhadi M, Alsoufi A, Alhadi A, Hmeida A, Alshareea E, Dokali M et al. Knowledge, attitude, and acceptance of healthcare workers and the public regarding the COVID-19 vaccine: a cross-sectional study. BMC Public Health. 2021;21(1):1-21. PubMed | Google Scholar
- Zaitoon H, Sharkansky L, Ganaim L, Chistyakov I, Srugo I, Bamberger E. Evaluation of Israeli healthcare workers knowledge and attitudes toward the COVID-19 vaccine. Public Health Nurs. 2022 Mar;39(2):415-422. PubMed | Google Scholar
- Cvjetkovic SJ, Jeremic VL, Tiosavljevic DV. Knowledge and attitudes toward vaccination: a survey of Serbian students. J Infect Public Health. 2017;10(5):649-56. PubMed | Google Scholar
- Saied SM, Saied EM, Kabbash IA, Abdo SA. Vaccine hesitancy: beliefs and barriers associated with COVID-19 vaccination among Egyptian medical students. J Med Virol. 2021;93(7):4280-91. PubMed | Google Scholar
- Khankeh HR, Farrokhi M, Khanjani MS, Momtaz YA, Forouzan AS, Norouzi M et al. The Barriers, challenges, and strategies of COVID-19 ( SARS-CoV-2 ) vaccine acceptance: a concurrent mixed-method study in Tehran City, Iran. Vaccines (Basel). 2021 Oct 28;9(11):1248. PubMed | Google Scholar
- Kumari A, Ranjan P, Chopra S, Kaur D, Kaur T, Upadhyay AD et al. Knowledge, barriers and facilitators regarding COVID-19 vaccine and vaccination programme among the general population: a cross-sectional survey from one thousand two hundred and forty-nine participants. Diabetes Metab Syndr Clin Res Rev. 2021;15(3):987-92. PubMed | Google Scholar





