Knowledge of mothers with children age 1 to 24 months on diaper dermatitis management and associated practice in a referral Hospital in Northern Ghana: a cross sectional study
Gbeti Collins, Abdul-Wahab Inusah, Mubarick Nungbaso Asumah, Peter Gyamfi Kwarteng, Shamsu-Deen Ziblim, Peter Dzomeku
Corresponding author: Mubarick Nungbaso Asumah, Department of Global and International Health, School of Public Health, University for Development Studies, Tamale, Ghana 
Received: 04 Mar 2022 - Accepted: 21 May 2022 - Published: 25 May 2022
Domain: Pediatrics (general),Public health
Keywords: Diaper dermatitis, diaper rash, Ghana, infants, knowledge, management
©Gbeti Collins et al. PAMJ-One Health (ISSN: 2707-2800). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Gbeti Collins et al. Knowledge of mothers with children age 1 to 24 months on diaper dermatitis management and associated practice in a referral Hospital in Northern Ghana: a cross sectional study. PAMJ-One Health. 2022;8:5. [doi: 10.11604/pamj-oh.2022.8.5.34112]
Available online at: https://www.one-health.panafrican-med-journal.com/content/article/8/5/full
Research 
Knowledge of mothers with children age 1 to 24 months on diaper dermatitis management and associated practice in a referral Hospital in Northern Ghana: a cross sectional study
Knowledge of mothers with children age 1 to 24 months on diaper dermatitis management and associated practice in a referral Hospital in Northern Ghana: a cross-sectional study
![]() Gbeti Collins1,
Gbeti Collins1, ![]() Abdul-Wahab Inusah2,
Abdul-Wahab Inusah2, ![]() Mubarick Nungbaso Asumah2,3,&, Peter Gyamfi Kwarteng4, Shamsu-Deen Ziblim5,
Mubarick Nungbaso Asumah2,3,&, Peter Gyamfi Kwarteng4, Shamsu-Deen Ziblim5, ![]() Peter Dzomeku6
Peter Dzomeku6
&Corresponding author
Introduction: diaper dermatitis is found to be the most common skin condition among children below 24 months. Though it is generally less fatal, it could elevate into a severely painful condition with possible bacterial and fungal infestation requiring a critical medical attention. The study assessed the knowledge of mothers with children in the diaper-wearing age on diaper dermatitis management and associated practice in a referral hospital in Northern Ghana.
Methods: the study employed the facility-based cross-sectional study design. A total of 456 mothers with infants aged 1-24 months were recruited using the systematic sampling technique. Data was collected using a structured questionnaire and analyzed using SPSS version 25. A p-value <0.05 was considered statistically significant.
Results: only a few (23.5%) of the respondents had good knowledge on diaper management with 76.5% reporting poor knowledge. Mothers used baby powder (47.0%), zinc oxide that contained barrier cream baby oil (28.0%), Vaseline (16.0%), baby lotion (16.0%) to prevent diaper dermatitis. Employment status (p=0.011), attachment of diaper to babies (p=0.041), drying methods used after cleaning a child (p=0.039) and substance used to clean infants after bowel movement (p=0.011) were significantly associated with knowledge of diaper dermatitis. Mothers who were full-time homemakers were 1.76 times more likely to have good knowledge in diaper management compared to mothers engaged in economic activities (COR=1.76; Cl (1.14-2.73)).
Conclusion: the study showed a low knowledge of diaper dermatitis. Most mothers resort to powder to prevent diaper dermatitis. We recommend that the Ministry of Health, and all health agencies to as a matter of urgency design a framework on the dissemination of reliable information on diaper dermatitis prevention and management.
Almost every modern day parent uses diapers primarily to prevent uri-fecal soiling of child and ensure the child and parental convenience [1]. However, irregular changing of diapers and inappropriate cleaning of the child´s groins (diaper area) can result in the accumulation of fecal matter and urine around the diaper area for unreasonably long periods resulting in a skin inflammatory (irritating rashes) condition known as diaper dermatitis (DD) [2-4]. The condition is usually seen around the groins (covex) such as the buttocks, genitalia, perineum, medial or upper side of the thigh [5] and and around the lower abdomen because of the close contact the diaper’s inner surface has with those areas of the skin. The skin in reaction to irritations forms excess hydration, friction, maceration and sometimes enzymes from fecal enzymes like fecal protease lipase may turn out to be erythematous and scaly, often characterized by papulovesicular or bullous lesions, fissures, and erosions all characterizing diaper dermatitis or rash [5,6]. Diaper dermatitis is found to be the most common skin condition among children below 24 months with children between 8 to 12 months being the worst affected usually due to the introduction of complementary feeding i.e. solid foods [5,7]. Diaper dermatitis is estimated to constitute about 20% of pediatric dermatological cases in health facilities [8]. Though it is generally less fatal, it could elevate into a severely painful condition with possible bacterial and fungal infestation requiring a critical medical attention in infants and a source of worry and anxiety for concerned parents especially [5,9,10].
While most cases of diaper dermatitis can be cured with routine skin care and adoption of diapering hygiene practices, inappropriate hygiene practices such as infrequent cleaning of diaper area with the appropriate substances or materials as well as infrequent change of diapers are largely due to diaper need or low knowledge on diaper management and hygiene practices [5,10]. In Nigeria, Eke and Ibo, [5] found mothers to have insufficient knowledge on basic facts such as identification of the cause, prevention and management of diaper dermatitis among mothers. In the study, just a few (14.6%) of mothers who reported diaper dermatitis changed their baby´s diapers three or more times a day. Knowledge on routine care indicators was found to be generally low [5]. In Bangladesh, knowledge on diaper management practices was found to be a significant predictor of diaper dermatitis as mothers who had knowledge on causes, preventions and adequate practice of cleaning the diaper area during diaper changes reported fewer (24.0%) cases of diaper dermatitis in their infants than those who did not (36.5%) [11]. Kim et al. [12] in Korea reported 59.7% knowledge on diaper dermatitis. Again, inappropriate hygiene practices such as use of talcum powder on diaper rashes (17.1%), rubbing with a dry towel after cleansing (58.0%) and attaching baby diapers tightly (23.9%) were among other unhygienic practices recorded in the study with only 37% of mothers using the ideal skin barrier to prevent diaper dermatitis.
Whereas many children below the age of two years suffer from diaper dermatitis, levels of education and perceived need for education on this subject appear to be low [12] especially in our health facilities as majority (70%) of mothers [12] obtained information related to diaper dermatitis from websites. The situation could be attributed to inadequate literature on the subject. Being the first study in Ghana, the current study determined the knowledge of mothers with children within the diaper-wearing age on diaper dermatitis and related hygiene practice in a referral hospital in Northern Ghana. To address these issues, the following specific objectives were explored: the level of knowledge on diaper dermatitis among the study participant, diaper dermatitis management practices. Also, the study will look at the associated factors with the knowledge of diaper dermatitis management.
Study design and setting: we adopted a facility-based cross-sectional study design to assess knowledge on diaper dermatitis and diaper hygiene practices among mothers with infants aged 1-24 months attending the Child Welfare Clinic (CWC) at the Tamale West Hospital, Northern Region of Ghana from July to September 2021. The facility serves as a referral Hospital for sub-district health facilities, and surrounding district hospitals. The facility runs 24-hourservices and has several units including the CWC where this study was conducted. [CWC is a unit in a hospital that weighs and vaccinates under five (5) years old children with the Ghana Health Service approved vaccines at no cost].
Sampling population: the study included only mothers with 1-24 months old infants attending CWC within the study settings. Infants on admission or severely ill were excluded from the study.
Study variables: the dependent variable was the knowledge of the mothers on diaper dermatitis. The independent variables were the mother´s socio-demographics characteristics (Age, level of education, occupational status, average monthly income, religion, etc), the frequency in the change of diapers, and types of diaper used.
Data resources and management: the data emanating from this study were obtained solely from study participants (primary data).
Data collection tool: we used a Standardized questionnaire adopted from a similar study in Korea [12].
Data collection procedures: the questionnaire consisted of 5 questions on socio-demographic characteristics, 12 questions on knowledge DD, whilst 8 items were used to assess respondents diaper hygiene management practices. Four nurses fluent in the local language (Dagbani) were recruited and trained on how to use a smartphone with KoboCollect Application installed for the entire data collection exercise. Pre-testing of the instruments was done at a different hospital before the actual data collection began. Data were collected from 456 mothers using a closed-ended questionnaire through face-face exit interviews. To enhance confidence and protect study participants´ confidentiality, the staff of the Child welfare clinic (CWC) of the Tamale West Hospital provided a separated room where the questionnaires were administered. Prior to participation in this study, the respondents were taken through the study protocols. Those who consented voluntarily were then recruited. To increase accuracy, two of the authors (MNA and AI) who are experienced field enumerators devoted time to verify all questionnaires. A trained pediatrician (PGK) who was part of the study supervised the data collection process for consistency. All authors who conducted and supervised the data collection were fluent in English and Dagbani (the predominate local language in Tamale, Northern Region).
Sample size and sampling procedures: we calculated the sample size using a single population proportion formula with an assumption of 50% population proportion (p=0.5) due to the non-existence of similar studies in the study settings. At 95% confidence level, a 5% margin of error and normal population distribution (Z)=1.96 were entered into Raosoft an online sample size calculator [13] to determine the sample size. We adjusted for a 5% non-response rate; thus, the minimum number of participants recruited unto the study was 400. Using the facility’s daily average CWC attendance of 58 (DHIMS data) each day as a sample frame , a maximum of 10 mothers were sampled and interviewed using a systematic sampling technique with 5 as sample interval. To avoid selection bias, the sitting arrangements of the study participants were not altered at any point.
Measurement of study variables: we assessed respondents´ knowledge of diaper dermatitis (DD) using a 12-item closed-ended questionnaire adopted from a previous study [12]. Four of the questions were true statement whilst the remaining were false statements. Respondents were required to say “True”, “False” or “Don´t know” to each of the knowledge questions. We calculated respondents´ knowledge by assigning a one (1) point to the correct answer and zero (0) to an incorrect answer or “Don´t know” responses. From the analysis, cumulative mean score for the 12-item knowledge variables was 4.71±1.62, which was below 6 median score (0-12). The median score was used to determine the knowledge level of the respondents. All those who scored above the median, were classified as having good knowledge, whilst those below were considered as having poor knowledge. Respondents, diaper hygiene management practices were evaluated using an 8-item closed-ended questionnaire. These included; “What type of diapers do you use?”, “How do you clean your child after changing a diaper?”, “How do you attach a diaper to your child?”, “frequency of diaper changes” etc. The study also assessed the socio-demographic characteristic of the respondents, these included the age group, educational level, religious affiliation, employment status, household monthly income and the number of children currently in diapers.
Data analysis: data was downloaded from the KoboToolbox server into Microsoft Excel v2019. All the questions were checked for completeness before being included in the data analysis. Data cleaning and data validation were done in Excel before being transported into SPSS version 25 for analysis. Descriptive statistics were reported using frequency(n), percentage (%), Mean or Standard Deviation (SD) and presented in a form of tables or figures. A Pearson Chi-square test (Bivariate test) was used to determine the association between categorical variables. Only Chi-square variables that were statistically significant at a p-value <0.05 were entered into a multivariate logistic regression model for inferential analysis at p-value <0.05. These criteria for the inclusion into the regression model was done to eliminate possible confounding variables.
Ethical consideration: ethical clearance and approval for the study were obtained from the University for Development Studies (UDS) Research Ethical Review Board. Two senior pediatricians at the Tamale Teaching Hospital reviewed the study protocol and the necessary adjustments were made. An introductory letter introducing the researchers to the hospital was obtained from the Department of Population and Reproductive Health (UDS). Approval was granted by the Hospitals´ Research and Development Committee (RDC)before the commencement of the study. The purpose of the study and confidentiality of respondent´s data were explained to participants. Participation was purely voluntary, and all participants provided their consent before they were interviewed. Finally, this study was conducted in accordance with the principles of the Declarations of Helsinki.
Socio-demographics of the respondents: out of the 456 mothers interviewed, 76.3% of them were within the age group of 18-30 years, most of the mothers were without formal educational (30.7%) with only 21.1% attaining tertiary educational status. More than half (61.8%) of the mothers were engaged in economic activities, and majority of mothers (88.4%) interviewed have at least a child using diapers (Table 1).
Respondents´ knowledge concerning diaper dermatitis: majority (86.2%) knew the common skin conditions amongst children, 87.1% identified not changing baby´s diapers frequently as the chief cause of DD. The majority of mothers (77.0%, and 55.5%) knew that some baby wipes containing alcohol and zinc oxide ointment respectively are used to prevent DD. Only 46(10.1%) knew that a sprinkle of talcum powder on a diaper will soak up moisture and help prevent DD was a false statement. Majority (70.7%) of the respondents had a wrong perception that disposable diapers cause DD more than cloth diapers. On the overall knowledge score, 23.5% of the respondents had good knowledge on diaper dermatitis, with 76.5.% reporting poor knowledge (Table 2).
Diaper management practices among the study participants: from the study, 11.6% of mothers wear the infants with plastic underpants, 51.1% of mothers firmly attached diapers to their babies to prevent faeces from leaking out. Most mothers (35.3%) use wet tissue to clean infants after bowel movement, this was followed by 31.6% of mothers using only water to clean the babies after bowel movement. Also, 58.6% of mothers dry their children after cleaning them using natural air, 35.5% uses dry towel to rub babies after cleaning whilst only 5.9% gently pat with dry towel. On the type of diaper used, close to 70% of the mothers reported using only disposable diapers, with 3 mothers reported using cloth diaper only. On the frequency of diapers changes per a day, 52% of mothers changed their babies´ diapers at most 2 times, this was followed by 46% of mothers changing their babies´ diaper 3-4 times daily. The mean cost of diaper in this study was one Ghana Cedis (1± .24) with 27.6% of mothers reporting diaper dermatitis in the last six months as shown in Table 3.
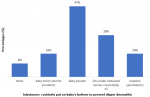
Substances used on infants to prevent diaper dermatitis among respondents: the study showed that the following substance was used to prevent diaper dermatitis; baby powder (47.0%), zinc oxide that contained barrier cream baby oil (28.0%), vaseline (petrolatum) (16.0%), baby lotion (barrier emollient) (16.0%) and 9% do not use any substance (Figure 1).
Association between respondents' socio-demographic characteristics, practice variables and knowledge on diaper management: Table 4 shows the association between socio-demographic variables, respondents´ diaper hygiene practices and knowledge on the management of diapers. The only socio-demographic variables with significant association with knowledge of diaper management was employment status of mothers (X2=6.46, p=0.011). Also, proper attachment of diaper to babies (X2=0.54, p=0.041), drying methods used after cleaning a child (X2=6.50, p =0.039) and substance used to clean infants after bowel movement (X2=13.16, p=0.011) were found to have evidence of statistical association with knowledge of diaper management.
Factors associated with knowledge of diaper management: mothers who were full-time homemakers were 1.76 times more likely to have good knowledge in diaper management compared with mothers engaged in economic activities (COR=1.76; 95% Cl (1.14-2.73)). The remaining variables were not significant with knowledge (Table 5).
The study aimed at determining the knowledge of mothers with children in the diaper-wearing age on diaper dermatitis and related hygiene practice in a referral hospital in Northern Ghana. The findings of the current study showed that there is low knowledge of diaper management among mothers. This is slightly lower than the findings of the study conducted in rural communities of the Kanchipuram District, India, where about 30.0% of mothers had good management of diaper dermatitis [14]. These findings are similar because the studies were conducted in resource constraints environments with the level of literacy being low. Contrary to the above, a study in Korea revealed that 59.7% of mothers had appreciable knowledge on diaper dermatitis management [12]. Korea is a developed country with high awareness of health issues. Comparatively, more respondents in the Korean study were educated than in the current study. The sample size of the current study is two times higher than that of the study in Korea. These reasons could account for the wide differences.
A higher proportion of the caregivers used disposable diapers for their babies. This is consistent with a study in Port Harcourt in Nigeria, where most (44.7%) caregivers reported to be using disposable diapers [5]. The similarities between these two countries (Nigeria and Ghana) are that both countries have disposable diaper usage being highest. However, the use of disposable diapers in Ghana is higher than in Nigeria. Though disposable diapers are expensive, it is convenient and saves productive time. These advantages have led to the increased use of disposable pads. We believe that the disposable diapers and cloth diaper usage come with their attendant problems. This is because those using cloth diapers are expected to wash them with soap and water and dry them before use. Considering this processes of reusable cloth, disposable diapers cannot be said to be expensive. Available literature has shown that disposable diaper usage is often associated with higher education and the economic strength of the household [15,16]. However, it is common knowledge in Northern Ghana that mothers who use disposable diapers always are often said to be lazy mothers. This misconception is fading away as many more rural folks use disposable diapers, as shown in this study.
On the diaper use per day, there is no clear-cut rule on the frequency of diaper use. However, as much as possible, the diapers need to change when the babies soil themselves. Delays in changing the diapers could contribute to dermal dermatitis. That said, the study showed that 27.4% of babies had diaper dermatitis. The reported prevalence of DD is higher than 24.6% reported in a prospective experimental study in the UK [17]. However, the findings of this study are lower than compared to the 36.1% reported prevalence of DD in Thai [18]. A review of literature on the prevalence of DD and its associated factors in Japan pegged the prevalence of DD within the range of 11.5% to 70.6% [19]. The difference in these studies could be attributed to the methodological differences, since there is no standard rule in measuring the DD prevalence. Also, the study was mainly among infants aged 1 to 24 months, whose diaper needs are higher compared to those above 24 months. In the current study, 35.3% and 31.6% used wet tissue (wipes) only and water only respectively to clean the baby after a bowel passage. This is related to a study where 54.1% of mothers report using wet wipes to clean the diaper areas [20]. Blume-Peytavi et al. [21] in a review of literature on diaper dermatitis prevention in infants, revealed that washing the diaper area with baby wipes or water and a wash-cloth had similar effect on diapered skin. However, Adam et al. [22] discovered that a single washing procedure using several treatments such as soap, detergent, wipes, and water had a direct influence on the skin's surface.
Among the neonates, pH in the skin reduces over the first 4 weeks of life, even without the use of wipes or water and washcloth [23]. However, for babies who are more than 4 weeks, the PH values of the skin are considered to be within the normal ranges even after using these cleansing methods (water, wipes, or washcloth) [24,25]. Lavender et al. [25] observed no difference in diaper dermatitis severity among study participants who use wipes and washcloth in a randomised controlled study. Also, there was no difference in diaper dermatitis reported among 44 healthy babies on day 28 between two groups who used baby wipes or a water-moistened washcloth to clean the diaper region for four weeks [23]. Disposal diapers just like sanitary pads have serious waste management issues. Though the current study did not explore these effects, we recommend to researchers with interest in the subject matter to consider exploring the effect of disposable diapers on the environmental health of the population.
Most of mothers use powder on the baby's bottom to prevent diaper dermatitis. This is inconsistent with about 80.0% of mothers using Vaseline to prevent dermatitis in Nigeria [5]. It is not recommended to use Talc powders because it does not form a continuous lipid barrier layer over the skin and block the skin pores [5], producing an ideal environment for diaper rash to develop. That said, the ought to be serious education on the choice of powders used on babies. Zinc oxide and petroleum gel are the time-tested components in diaper creams [5,17]. Only 28.0% of the mothers in the current study were using the recommended diaper creams. The Ghana Health Services and all agencies in health need to provide more information on diaper dermatitis prevention. In the current study, employment status was associated with knowledge. To the specifics, full-time homemakers were 1.76 times more likely to have good knowledge on diaper management compared with mothers engaged in economic activities (COR=1.76; 95% Cl (1.14-2.73)). This current study could not identify other studies to support this finding. We believe that the homemakers are with their babies and provide the diaper needs of the child. Mothers engaged in economic activities do not have enough time for their babies. In most instances, a nanny is employed to take care of the child. This, therefore, explain why mothers who were full-time housemakers demonstrated appreciable knowledge on diaper management compared to those engaged in economic activities.
Limitations: as with all cross-sectional studies, casual effects are not determined. Although, the study was conducted in a referral hospital, generalization of these findings ought to be done with caution.
The study showed a low knowledge of diaper dermatitis. Most mothers resort to powder to prevent diaper dermatitis. The higher proportion of mothers using disposable diapers may have serious environmental health ramifications which has not been explored. Issues of diaper needs and diaper dermatitis is a novel area in Ghana. The study, therefore, recommends researchers with similar interest on the subject to consider exploring more themes such as "the effects of disposable diapers use on environmental health", "factors influencing the use of disposable diapers", "the factors accounting for low knowledge on diaper dermatitis” and “ways to improve management practices of diaper dermatitis among caregivers". In the meantime, we recommend that the Ministry of Health, Ghana Health Services, and all agencies with public health interest to as a matter of urgency design a framework on the dissemination of reliable information on diaper dermatitis, its prevention and management.
What is known about this topic
- Diaper dermatitis is found to be the most common skin condition among children below 24 months;
- Diaper dermatitis is estimated to constitute about 20% of pediatric dermatological cases in health facilities;
- Diaper dermatitis can be cured with routine skincare and adoption of good diapering hygiene practices.
What this study adds
- Only 23.5% of the respondents had good knowledge on diaper dermatitis, with 76.5.% reporting poor knowledge;
- Mothers used baby powder, zinc oxide that contained barrier cream baby oil, Vaseline, baby to prevent diaper dermatitis;
- There are very few literatures on diaper dermatitis, with this study being the first in Northern Ghana.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
We are indebted to the participants who voluntarily decided to share their experiences to enrich this research.
Table 1: socio-demographic characteristics of mothers
Table 2: analysis of respondents knowledge of diaper management
Table 3: management practice of diaper among mothers
Table 4: bivariate analysis of socio-demographic and diaper hygiene practice factors associated with knowledge of diaper management
Table 5: multivariate logistics regression of factors associated with knowledge on diaper management among the 456 mothers
Figure 1: substances routinely put on baby's bottom to prevent diaper dermatitis
- Marcovitch H. Black´s medical dictionary. A&C Black Publishers Limited. 2005;360.
- Williams K, Williams L. Diaper rash relief: common sense remedies and treatments. Int J Pharm Compd. 2011;15:464-70.
- Bolognia J, Jorizzo JL, Rapini RP. Dermatology. 2003. Google Scholar
- Kliegman R. Biologic effects of radiation on children. In: Kliegman RM, Behrman RE, St Jeme J, eds. Nelson textbook of pediatrics. Elsevier, editor. Elsevier Health Sciences; 2016. 3416-3422.
- Eke GK, lbo Opara P. Mothers knowledge and home management of nappy rash in Port Harcourt, Nigeria. Niger Heal J. 2013;13(4):152-7. Google Scholar
- Berg RW. Etiology and pathophysiology of diaper dermatitis. Adv Dermatol. 1988;3:75-98. PubMed | Google Scholar
- Atherton D, Mills K. What can be done to keep babies´ skin healthy. RCM Midwives. 2004 Jul;7(7):288-90. PubMed | Google Scholar
- Philipp R, Hughes A, Golding J. Getting to the bottom of nappy rash. ALSPAC survey team; avon longitudinal study of pregnancy and childhood. Br J Gen Pract. 1997;47(421). PubMed | Google Scholar
- Jordan WE, Lawson KD, Berg RW, Franxman JJ, Marrer AM. Diaper dermatitis: frequency and severity among a general infant population. Pediatr Dermatol. 1986 Jun;3(3):198-207. PubMed | Google Scholar
- Rania D, Kazzi AA. Diaper rash: practice essentials, pathophysiology, etiology. eMedicine Medscape. 2021.
- Sadique Z, Begum NF, Sarker MFR, Bhuyian MNI, Kamruzzaman M. Mothers´ knowledge about diaper rash and preventive measures in Bangladesh. Dhaka Shishu Hosp J. 2020;36(1):39-45. Google Scholar
- Kim JS, Jeong YS, Jeong EJ. Knowledge of diaper dermatitis and diaper hygiene practices among mothers of diaper-wearing children. Child Heal Nurs Res. 2019;25(2):112-22. PubMed | Google Scholar
- Raosoft. Sample size calculator. 2020.
- Prithiba G, Priya K, Rekha R, Rebekahal R, Joseph VM. Assessment of knowledge of mothers regarding diaper rashes in infants in a selected rural community, Kanchipuram District, Tamil Nadu, India. Med Leg Updat. 2020;20(2):58-60. s Google Scholar
- Agestika L, Sintawardani N, Hamidah U, Nyambe S, Yamauchi T. Pattern of child faeces management and disposable diaper usage among under-fives in an urban slum of Bandung, Indonesia. J Water, Sanit Hyg Dev. 2022. Google Scholar
- Leaska M. Solid waste management of disposable diaper sanitation and the connection to environmental awareness for women in Zanzibar. SIT. 2016. Google Scholar
- Price AD, Lythgoe J, Ackers-Johnson J, Cook PA, Clarke-Cornwell AM, Phipps FM. The BaSICS (Baby Skin Integrity Comparison Survey) study: a prospective experimental study using maternal observations to report the effect of baby wipes on the incidence of irritant diaper dermatitis in infants, from birth to eight weeks of age. Pediatr Neonatol. 2021;62(2):138-45. PubMed | Google Scholar
- Sukhneewat C, Chaiyarit J, Techasatian L. Diaper dermatitis: a survey of risk factors in Thai children aged under 24 months. BMC Dermatol. 2019;19(1):1-6. PubMed | Google Scholar
- Yokoyama M, Haruna M, Yonezawa K, Sasagawa E, Hikita N. A review of the prevalence and factors associated with the development and prevention of diaper dermatitis in infants. J Japan Acad Midwifery. 2020;34(2). Google Scholar
- Ersoy-Evans S, Akinci H, Doğan S, Atakan N. Diaper dermatitis: a review of 63 children. Pediatr Dermatol. 2016;33(3):332-6. PubMed | Google Scholar
- Blume-Peytavi U, Hauser M, Lünnemann L, Stamatas GN, Kottner J, Garcia Bartels N. Prevention of diaper dermatitis in infants-a literature review. Pediatr Dermatol. 2014;31(4):413-29. PubMed | Google Scholar
- Adam R, Schnetz B, Mathey P, Pericoi M, De Prost Y. Clinical demonstration of skin mildness and suitability for sensitive infant skin of a new baby wipe. Pediatr Dermatol. 2009;26(5):506-13. PubMed | Google Scholar
- Garcia Bartels N, Massoudy L, Scheufele R, Dietz E, Proquitté H, Wauer R et al. Standardized diaper care regimen: a prospective, randomized pilot study on skin barrier function and epidermal IL1 in newborns. Pediatr Dermatol. 2012;29(3):270-6. PubMed | Google Scholar
- Visscher MO. Recent advances in diaper dermatitis: etiology and treatment. Future Medicine. 2009. Google Scholar
- Lavender T, Furber C, Campbell M, Victor S, Roberts I, Bedwell C et al. Effect on skin hydration of using baby wipes to clean the napkin area of newborn babies: assessor-blinded randomised controlled equivalence trial. BMC Pediatr. 2012;12(1):1-9. PubMed | Google Scholar