Knowledge, attitude and practice towards COVID-19 among people living with HIV/AIDS attending State Specialist Hospital Maiduguri, Borno State, Nigeria
Muktar Musa Shallangwa, Honesty Iwenya, Shuaibu Saidu Musa, Emery Manirambona, Muhammad Aisha Hameed, Don Eliseo Lucero-Prisno III
Corresponding author: Shuaibu Saidu Musa, Department of Nursing Science, Ahmadu Bello University, Zaria, Nigeria 
Received: 11 Apr 2022 - Accepted: 13 Jul 2022 - Published: 18 Jul 2022
Domain: HIV epidemiology,Community health,Global health
Keywords: Knowledge, attitude, practice, HIV, people living with HIV, state specialist hospital Maiduguri, COVID-19, Borno State, North East, Nigeria
©Muktar Musa Shallangwa et al. PAMJ-One Health (ISSN: 2707-2800). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Muktar Musa Shallangwa et al. Knowledge, attitude and practice towards COVID-19 among people living with HIV/AIDS attending State Specialist Hospital Maiduguri, Borno State, Nigeria. PAMJ-One Health. 2022;8:10. [doi: 10.11604/pamj-oh.2022.8.10.34815]
Available online at: https://www.one-health.panafrican-med-journal.com/content/article/8/10/full
Research 
Knowledge, attitude and practice towards COVID-19 among people living with HIV/AIDS attending State Specialist Hospital Maiduguri, Borno State, Nigeria
Knowledge, attitude and practice towards COVID-19 among people living with HIV/AIDS attending State Specialist Hospital Maiduguri, Borno State, Nigeria
![]() Muktar Musa Shallangwa1,
Muktar Musa Shallangwa1, ![]() Honesty Chukwudi Iwenya2,
Honesty Chukwudi Iwenya2, ![]() Shuaibu Saidu Musa3,4,&,
Shuaibu Saidu Musa3,4,&, ![]() Emery Manirambona5, Muhammad Aisha Hameed6, Don Eliseo Lucero-Prisno III7,8
Emery Manirambona5, Muhammad Aisha Hameed6, Don Eliseo Lucero-Prisno III7,8
&Corresponding author
Introduction: in order to control and prevent the spread of COVID-19, people must have adequate knowledge, a positive attitude, and practice basic preventive procedures towards the disease. This study aims to determine the KAP towards COVID-19 among PLHIV undergoing clinical-outpatient follow-up at SSHM.
Methods: a hospital-based cross-sectional study was conducted to determine knowledge, attitude and practice (KAP) towards COVID-19 among 344 participants, who were selected using a simple random sampling technique from 4th January to 25th February 2022. A pretested and structured interviewer-administered questionnaire was used for data collection. Results were summarized in frequencies and percentages. The Chi-square test was used to determine factors influencing KAP.
Results: among the 344 participants that were enrolled in the study, adequate knowledge and positive attitude scores (≥75 correct answers) towards COVID-19 were reported in 72.4% and 62.5% of the participants, respectively. Most of the respondents (82%) were not practising basic preventive procedures against COVID-19. Knowledge and attitude scores were significantly associated (p<0.05) with gender, age, marital status and educational status, while practice score was significantly associated (p<0.05) with gender, marital status, educational status, employment status and time since HIV diagnosis. There was moderate positive correlation (r=0.60) between knowledge and attitude scores, while there was a low positive correlation (r=0.23) between knowledge and practice scores and attitude and practice scores, respectively.
Conclusion: people living with HIV have adequate knowledge, a positive attitude and poor practice towards COVID-19. Therefore, in order to mitigate coronavirus infection among People Living with HIV/AIDS (PLHIV), health talks at ART service delivery points should incorporate information on COVID-19 preventative strategies.
HIV infection remains a major global public health concern despite all the progress made in its treatment, and expansion of prevention strategies. As of 2020, around 37.7 million people lived with HIV infection worldwide, with 1.5 million newly diagnosed cases in 2020 [1]. In Nigeria, The Nigerian National HIV/AIDS Indicator and Impact Survey (NAIIS) of 2018 reported the prevalence of HIV at 1.4%, with 1.9 million people living with HIV (PLHIV). Although the prevalence was reported to be lower in the North Eastern Zone of the country (1.1%), Borno state had a prevalence of 1.3%, thus being categorized among states with medium prevalence [2]. While advances have been made to control and end the HIV epidemic, the coronavirus disease 2019 (COVID-19) pandemic has impelled those advances [3]. Coronavirus disease 2019 (COVID-19) is a highly infectious and acute respiratory disease caused by Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2), which is transmitted to humans through direct or indirect contact and/or feeding on infected animals with clinical manifestations similar to viral pneumonia such as fatigue, fever, shortness of breath, cough and other complications [4]. The World Health Organization (WHO) declared the disease a global pandemic on 11th March 2020, with 450,229,635 million cases and 6,019,085 deaths globally as of 11th March 2022 [5]. In Nigeria, the first case of COVID-19 was detected in Lagos State on 27th February 2020 and spread across the country. In Borno State, there were 254,861 confirmed cases and 3,142 deaths as of 11th March 2022 [6]. The impact of HIV infection on severity and mortality associated with COVID-19 is limited and conflicting in the literature. However, the World Health Organization report confirmed that HIV infection is a significant independent risk factor for severe/critical COVID-19 at hospital admission and in-hospital mortality [7]. The concern that PLHIV are more at risk for severe COVID-19 assumes that they are more likely to be immunocompromised, especially those with low CD4 cell count, high viral load, advanced disease, and those not on antiretroviral therapy (ART) [8]. Therefore, it becomes necessary to adopt additional measures to prevent PLHIV from contracting COVID-19.
Currently, there is no universal treatment for COVID-19. However, vaccines are available and offer hope for ending the pandemic, although prevention remains the best option for controlling this pandemic by reducing transmission. Despite the paucity of information regarding the safety of the COVID-19 vaccines in PLHIV, available information indicates that the COVID-19 vaccines recommended by WHO are safe for PLHIV and could benefit from COVID-19 vaccination [9]. The WHO has recommended that all PLHIV, regardless of their immune status, be included in COVID-19 vaccination and that countries should consider them as a priority group according to their epidemiological context [10]. In order to control and prevent the transmission of COVID-19, people need to have adequate knowledge about the disease, a correct attitude and employ good practices against the virus [11]. The information on the KAP of the population is essential in identifying gaps, improving the quality of services, and doing strategic planning for program purposes [12]. Having average knowledge of COVID-19 and a correct attitude towards adherence to government prevention and control measures is key to preventing COVID-19 [13]. To the best of our knowledge, this is the first research about KAP towards COVID-19 among PLHIV in Nigeria. Therefore, this study aims to assess the KAP of PLHIV undergoing clinical-outpatient follow-up at SSHM towards COVID-19. We expected that the outcomes of this study would unveil gaps that are useful for authorities in decision-making and the development of interventions towards bridging the gaps.
Study design: a hospital-based cross-sectional study was conducted among PLHIV undergoing clinical-outpatient follow-up at United States President´s Emergency Plan For AIDS Relief (PEPFAR) clinic in State Specialist Hospital Maiduguri (SSHM) from 4th January to 25th February 2022.
Study setting and population: State Specialist Hospital Maiduguri is a secondary-level referral hospital within the Maiduguri metropolis, with a total of 17 wards and three outpatient clinics. The hospital currently has a total of, 3309 PLHIV on treatment at the time of this research. The study participants included in this study are solely PLHIV undergoing clinical-outpatient follow-up at SSHM. Participants needed to meet the following inclusion criteria: being aware of their HIV status, being under clinical-out-patient monitoring at SSHM, and being 15 years of age or older.
Data resource and measurement
Data collection tool: a structured interviewer-administered questionnaire prepared in the English language and adapted from the WHO COVID-19 recommendations and relevant published articles [3,13-15].
Data collection: data collection was conducted by three research assistants. Socio-demographic characteristics and other variables such as knowledge, attitude and practice towards COVID-19 were collected by the data collection tool. A total of 12 questions were used to assess knowledge, with the answer being "yes" or "no" or "I do not know". A correct answer was given 1 point, and an incorrect answer/do not know was given 0 point. Respondents who scored greater than, or equal to 9, were considered to have "adequate knowledge". The attitude of the participants towards COVID-19 was assessed by eight questions, which were answered as "yes" or "no" or "I do not know". Participants who scored greater than or equal to six correct answers (75%) from the eight scored attitude questions were considered to have a "positive attitude" towards COVID-19. Similarly, the participants' practice towards COVID-19 was also assessed by eight questions, answered as "yes" or "no". Participants who scored greater than or equal to 6 correct answers (75%) from the eight scored practice questions were practising COVID-19 prevention measures. To ensure the reliability of the questionnaire, a pilot study was conducted among 20 randomly selected PLHIV at SSHM, who were excluded from participating in the main study. The pretested and validated questionnaire was then administered to the research participants.
Sample size: the sample size was calculated using Cochran´s formula [16] at a 95% confidence level, where Z is taken at 1.96.
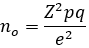
Prevalence is assumed to be 50% as there was no similar study in the study area and margin of error (e) was taken as 5%. Using the formula, the sample size was obtained as 384. Since the target population in the study is less than 10000, the sample size was further adjusted using Cochran´s correction formula.
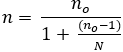
Where n is the corrected sample size, now is the uncorrected sample size, and N is the population size. Using this correction formula, the final sample size obtained was 344. The study participants were then selected using a simple random sampling technique.
Data analysis: data were entered in protected Microsoft Excel, 2016, and after double typing and random manual checks in order to ensure the validity of the data entered, the databank was exported to and analysed using IBM Statistical Package for Social Science (SPSS) (Version 26). Results were summarised in frequencies and percentages. The Chi-square test was used to explore the association between the independent variables of the study and KAP scores, and p-values were considered significant at values less than or equal to 0.05.
Ethical consideration: ethical clearance to conduct this study was obtained from the ethical review and clearance committee of State Specialist Hospital Maiduguri. The study participants were only registered after the aim and objectives of the study were clearly explained to them and their informed consent for the study and its publication was obtained.
Socio-demographic analysis: a total of 344 people living with HIV/AIDS participated in this study. The socio-demographic characteristics of the participants are shown in Table 1. The majority, 242(70.3%), were females, and most of the participants, 202 (58.7%), were 25 years and above. Of the total respondents, 174 (50.6%) were married, 126 (36.6) were literate and only 70 (20.3) were employed. All the participants were currently receiving ART and the majority of them, 194 (56.4%), were diagnosed with HIV greater than or equal to 5 years ago.
Knowledge about COVID-19 analysis: in the current study, 249 (72.4%) and 95 (27.6%) participants had adequate and inadequate knowledge about COVID-19, respectively. Twelve knowledge questions and the corresponding knowledge scores of the participants about COVID-19 are shown in Table 2. 257 (74.7%) participants knew that the most common clinical symptoms of COVID-19 are fever, dry cough and fatigue. Two hundred and thirty 230 (69.9%) of the respondents believed that only symptomatic individuals have COVID-19 and 133 (38.7%) agreed that HIV infected individuals on regular effective antiretroviral therapy and following preventive measures do not have a higher risk of contracting the coronavirus. The majority of the participants, 319 (92.7%), agreed that COVID-19 spreads when an infected person exhales virus-containing respiratory droplets and tiny particles. 158(45.9%) respondents believed that children and young adults must take precautions to avoid becoming infected with COVID-19. 271(78.8%) of the respondents knew that individuals should avoid going to crowd places and riding public transportations to avoid becoming infected with COVID-19. Most of the respondents, 270 (78.5%), knew that isolation and treatment of COVID-19 infected individuals are efficient approaches to reduce the spread of the virus. The majority of the participants, 312 (90.7%), know that COVID-19 vaccines are available and PLHIV could benefit from COVID-19 vaccination.
Attitude towards COVID-19 analysis: Two hundred and fifteen 215 (62.5%) and 129 (37.5%) of the participants had positive and negative attitudes towards COVID-19, respectively. Eight attitude questions and the corresponding attitude scores of the participants about COVID-19 are shown in Table 3. The majority of the participants, 257(74.7%), believed that COVID-19 is a curable disease and 180 (52.3%) respondents had confidence that Nigeria could win the battle against COVID-19. Most of the respondents, 251 (73%), believed that they would go to the quarantine centre if they developed the sign and symptoms of COVID-19. Two hundred and sixty-nine percent (269 (78.2%) participants agreed that they would report suspected cases to health authorities. One-hundred and forty-four percent (144 (41.9%) participants believed that people infected with HIV and on ART could not be infected with SARS-CoV2. 141 (41%) respondents do not know that the COVID-19 vaccine is safe and effective.
Practice towards COVID-19 analysis: the majority of the study participants, 282 (82%), were not practicing basic preventive procedures against COVID-19. Eight practice questions and the corresponding practice scores of the participants about COVID-19 are shown in Table 4. Preventive procedures of avoiding crowds, wearing a face mask when living home, washing of hands frequently and use of hand sanitisers in maintaining hand hygiene, keeping regularly touched objects and surfaces clean and disinfected and social distancing were followed by 162 (47.1%), 124 (36%), 90 (26.2%), 142 (41.3%), and 123 (35.8%) respectively. Most of the respondents, 300 (87.2%), cover their nose and mouth with their elbow or a tissue when coughing or sneezing. Only 88 (25.6%) of the participants have received the COVID-19 vaccine.
Association between independent variables of the study and KAP scores analysis: the association test between the study's independent variables and the knowledge, attitude and practice towards COVID-19 among the participants is described in Table 5. There was a statistically significant association (p<0.05) between the knowledge score and the following variables: sex, age, marital status and educational status. Attitude score was significantly associated (p<0.05) with sex, age, marital status, educational status and time since HIV diagnosis. The sex, marital status, educational status, and time since HIV diagnosis of the respondents were also significantly associated (p<0.05) with practice scores.
Correlation between knowledge, attitude and practice analysis: there was a moderate positive correlation (r=0.60) between knowledge and attitude scores (p=0.000): attitude scores increase with increasing knowledge scores. There was a low positive correlation (r=0.23) between knowledge and practice scores (p=0.000): practice scores increase with increasing knowledge scores. Similarly, there was also a low positive correlation (r=0.26) between attitude and practice scores (p=0.000), as shown in Table 6.
With the novelty of COVID-19 and its clinical and epidemiological ambiguities, a population-level investigation of KAP becomes crucial for effective public health planning, implementation, and management [17]. To our knowledge, this is the first study to assess the KAP on COVID-19 among PLHIV in Nigeria. Of note, most of the study participants are females aged 25 years and above, illiterates and unemployed. The study revealed that the participants' overall knowledge about COVID-19 was high (72.4%). This result is consistent with Dzinamanra et al. [3], which reported high COVID-19 knowledge scores among PLHIV. The possible reason for this could be that the routine COVID-19 health talk is being provided to the PLHIV at the health facility. Furthermore, the information on COVID-19 is widely circulated on various media platforms both locally and internationally. Interestingly, the knowledge scores reported in this study are less than that of a previous study among PLHIV in Rwanda [3], probably because most participants in this study were illiterate and unemployed and might have limited access to necessary devices and the internet to access information on COVID-19. Therefore, ART clinics should intensify COVID-19 health talks during counselling sessions to close this gap. Factors significantly associated with participants' knowledge in the study were: (I) male participants, which is consistent with a previous report in Nigeria [18], (II) married participants, which is consistent with other studies [12,18-20], 25 years and above, which is consistent with a previous report in Jordan [16] and (IV) literacy, which is also congruent with other studies [12,15]. Notably, most participants (91%) knew that the COVID-19 vaccine was now available. This is important since vaccines proved to play a vital role to end the pandemic, and PLHIV could benefit from the vaccination [9].
In terms of attitude, most of the study participants (62.5%) had a positive attitude towards COVID-19. This result is congruent with Ghate et al. [13], which reported a higher positive attitude towards COVID-19 among PLHIV. However, it is dissimilar to a previous report in Rwanda [3] that reported a poorer attitude towards COVID-19 among people living with HIV. This is probably due to differences in participants' environmental characteristics and the timings during which the studies were conducted. Factors significantly associated with participants' attitudes in the study were female participants, married participants, aged 25 and above and literacy. One of the most pressing COVID-19 information needs of the participants was the safety and effectiveness of COVID-19 vaccines, as only 41% of the respondents believe that the COVID-19 vaccine is safe and effective. Therefore, health care workers at ART Clinics should enlighten the PLHIV on the importance of the COVID-19 vaccine, including its safety and efficacy. Although most of the study participants had adequate knowledge and a positive attitude towards COVID-19, this did not translate to the adoption of good preventive COVID-19 related practices as most of the participants (82%) were not practising basic preventive procedures against COVID-19. This finding is not consistent with previous reports about the practice of basic preventive procedures against COVID-19 among PLHIVs in Rwanda [3] and India [13]. It could be due to differences in timings of the study since the two studies were conducted in the earlier stage of the pandemic and also probably due to fewer COVID-19 positive cases reported within Borno state [2], so the residents might believe that they are at a lower risk of contracting the virus as reported in a study among residents of non-Hubei districts in China [21]. Factors associated with practice included: male, unmarried, illiterate, unemployed, and those diagnosed with HIV greater than or equal to 5 years ago. The reasons why these variables are significantly associated with the practice are not very clear and may need to be explored in subsequent studies. It is noteworthy that COVID-19 vaccine uptake among the respondents was very low, as only 25.6% of the participants reported being vaccinated. Considering the recent report from the WHO that confirms that HIV infection is a significant independent risk factor for both severe/critical COVID-19 presentation at hospital admission and in-hospital mortality [7], it is, therefore, crucial for PLHIV to be vaccinated. Future studies should unveil the potential barriers to COVID-19 vaccine uptake among the PLHIVs, in order to enable public health policymakers to make more informed decisions.
Interestingly, our study revealed a significant positive correlation between knowledge, attitude, and practice. This finding is consistent with a previous study among PLHIV in Rwanda [3]. This implies that promoting COVID-19 preventive practices would require promoting knowledge and attitude among the PLHIV. Therefore, educating the PLHIV about COVID-19 will provide them with adequate knowledge to enhance their attitude and encourage them to adopt good preventive COVID-19 related practices, which will ultimately help protect them from getting infected and reduce disease spread. There are limitations to this study. The study was a single-centred study and the sample size was small. Therefore, findings from the study cannot be generalized. Moreover, the respondents may have given socially acceptable answers, which may be different from actual reality. A more objective approach to assessment may have helped curtail this. However, despite these limitations, our study has some important strengths. This is the first study that assessed the KAP of PLHIV on COVID-19 in Nigeria. Therefore, findings from this study could lay a solid foundation for future COVID-19 KAP studies among PLHIV in the country. Furthermore, unlike most KAP studies on COVID-19 in Nigeria, this study was conducted when COVID-19 vaccines were available; therefore, information related to the COVID-19 vaccine, including its uptake, was reported. Finally, our research provides valuable information that will help public health officials make COVID-19-related decisions concerning PLHIV.
The study was conducted to assess the KAP regarding COVID-19 among PLHIV, who are at a higher risk of getting infected with the SARS-CoV-2. Our findings suggest that PLHIV have adequate knowledge, a positive attitude and poor practice towards COVID-19. This study suggests that health education about COVID-19 among PLHIV should be directed more towards less than 25 years females, unmarried people and illiterates. Health talks at ART service delivery points should include information on COVID-19 prevention practices in order to mitigate the infection among PLHIV.
What is known about this topic
- The overallknowledge and attitude in PLHIV towards COVID-19 is high.
What this study adds
- There is a significant positive correlation between knowledge, attitude, and practice towards COVID-19 in PLHIV;
- PLHIV have poor practice towards COVID-19 in Maiduguri, Borno State, Nigeria.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
The authors would like to express their gratitude to the staff of MSSH PEPFAR clinic for their support in this study, the research assistants for the data collection and the PLHIV that participated in the study. This research did not receive any specific grant from funding agencies in the public, commercial, ornot-for-profit sectors.
Table 1: sociodemographic analysis of PLHIV at SSHM, Borno State, Nigeria, 2022
Table 2: knowledge about COVID among PLHIV at SSHM, Borno State, Nigeria, 2022
Table 3: attitude towards COVID-19 among PLHIV at SSHM, Borno State, Nigeria, 2022
Table 4: practice towards COVID among PLHIV at SSHM, Borno State, Nigeria, 2022
Table 5: association between independent variables of the study and KAP scores among PLHIV at MSSH, Borno State, Nigeria
Table 6: correlation between knowledge, attitude and practice among PLHIV at SSHM, Borno State, Nigeria, 2022
- UNAIDS. Global HIV & AIDS statistics - 2021 fact sheet. Geneva; 2021. Accessed Jan 15, 2022.
- Nigeria HIV/AIDS Indicator and Impact Survey. NAIIS national factsheet. Nigeria; 2019. Accessed Jan 15, 2022.
- Iradukunda PG, Pierre G, Muhozi V, Denhere K, Dzinamarira T. Knowledge, attitude, and practice towards COVID-19 among people living with HIV/AIDS in Kigali, Rwanda. Journal of Community Health. 2021;46(2):245-250. PubMed | Google Scholar
- OladeleJ O, Ajayi EI, Oyeleke OM, Oladele OT, Olowookere BD, Adeniyi BM et al. A systematic review on COVID-19 pandemic with special emphasis on curative potentials of Nigeria based medicinal plants. Heliyon. 2020;6(9):e04897. PubMed | Google Scholar
- World Health Organization. COVID-19 dashboard. Accessed Mar 11, 2022.
- Nigeria Centre for Disease Control. COVID-19 Nigeria. Accessed Mar 11, 2022.
- Bertagnolio S, Thwin SS, Silva R, Ford N, Baggaley R, Vitoria M et al. Clinical features and prognostic factors of COVID-19 in people living with HIV hospitalized with suspected or confirmed SARS-CoV-2 infection. 11th IAS Conference on HIV Science. 2020.
- Shalev N, Scherer M, Lasota ED, Antoniou P, Yin MT, Zucker J et al. Clinical characteristics and outcomes in people living with Human Immunodeficiency Virus hospitalized for coronavirus disease 2019. Clinical Infectious Diseases. 2020;71(16):2294-2297. PubMed | Google Scholar
- Huang X, Yu M, Fu G, Lan G, Li L, Yang J et al. Willingness to receive COVID-19 vaccination among people living with HIV and AIDS in China: Nationwide Cross-sectional Online Survey. JMIR Public Health and Surveillance. 2021;7(10):1-18. PubMed | Google Scholar
- World Health Organization. Coronavirus disease (COVID-19): COVID-19 vaccines and people living with HIV. Accessed Jan 15, 2022.
- Nwagbara UI, Osual EC, Chireshe R, Bolarinwa OA, Saeed BQ, Khuzwayo N et al. Knowledge, attitude, perception, and preventative practices towards COVID-19 in sub-Saharan Africa: a scoping review. PLoS One. 2021 Apr 19;16(4):e0249853. PubMed | Google Scholar
- World Health Organization. Knowledge, attitudes and practices (KAP) surveys during cholera vaccination campaigns: guidance for oral cholera vaccine stockpile campaigns. Working Group on Monitoring & Evaluation, June. 2014:1-41.
- Ghate MV, Shidhaye PR, Gadhe KR, Gurav SG, Deoraj P. Knowledge, attitude and practices towards COVID-19 among people living with HIV in Pune, India: a cross-sectional study. International Journal of Research in Medical Sciences. 2021;9(5):1458. Google Scholar
- WHO. Coronavirus disease (COVID-19) pandemic. Accessed January 15, 2022.
- Al-Smadi AM, Tawalbeh LI, Ashour A, Shajrawi A, Gammoh O, Abu-Al-Rous N. Public knowledge, attitudes and practice about COVID-19 pandemic. Journal of Public Health in Africa. 2021 Jan 29;12(2):1519. PubMed | Google Scholar
- Cochran WG. Sampling techniques (3rd ed.). New York: John Wiley & Sons. 1977.
- Christopher R, Margaret R, Dauda MAD, Saleh A, Ene P. Knowledge, attitudes and practices towards COVID-19: an epidemiological survey in North Central Nigeria. Journal of Community Health. 2021;46(3):457-470. PubMed | Google Scholar
- Ngozichukwu C, Mbachu P, Azubuike CM, InnocentI, Ndukwu CI, Ezeuko AY. COVID-19 infection: knowledge, attitude, practices, and impact among healthcare workers in a South-Eastern Nigerian state. J Infect Dev Ctries. 2020;14(9):943-952. PubMed | Google Scholar
- Tsiga-Ahmed FI, Amole TG. COVID 19: evaluating the knowledge, attitude and preventive practices of healthcare Workers in Northern Nigeria. International Journal of Maternal and Child Health and AIDS. 2021;10(1):88-97. PubMed | Google Scholar
- Abdulrazaq MH, Muhammad FD, IliyasuG, Habib AG. Knowledge, attitude and practice survey of COVID-19 pandemic in Northern Nigeria. PLoS ONE. 2021;16(1): e0245176. PubMed | Google Scholar
- Zhong BL, Luo W, Li HM, Zhang QQ, Liu XG, Li WT. Knowledge, attitudes, and practices towards COVID-19 among Chinese residents during the rapid rise periodof the COVID-19 outbreak: a quick online cross-sectional survey. International Journal of Biological Science. 2020;16(10):1745-1752. PubMed | Google Scholar




