Improving access, quality and efficiency in health care delivery in Nigeria: a perspective
McKing Izeiza Amedari, Ifunanya Carista Ejidike
Corresponding author: McKing Izeiza Amedari, Department of Preventive and Community Dentistry, Obafemi Awolowo University Teaching Hospitals Complex, Ile-Ife, Osun State, Nigeria 
Received: 03 Feb 2021 - Accepted: 05 May 2021 - Published: 07 May 2021
Domain: Health economy,Health information system management,Health system development
Keywords: Access, quality, corruption
©McKing Izeiza Amedari et al. PAMJ-One Health (ISSN: 2707-2800). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: McKing Izeiza Amedari et al. Improving access, quality and efficiency in health care delivery in Nigeria: a perspective. PAMJ-One Health. 2021;5:3. [doi: 10.11604/pamj-oh.2021.5.3.28204]
Available online at: https://www.one-health.panafrican-med-journal.com/content/article/5/3/full
Perspective 
Improving access, quality and efficiency in health care delivery in Nigeria: a perspective
Improving access, quality and efficiency in health care delivery in Nigeria: a perspective
&Corresponding author
Providing equitable access to health care for every Nigerian is central in the country's National Health Act. But the Nigerian Health System ranks poorly in terms of access and quality just as the country also ranks poorly on Transparency International's Corruption Perception Index. The problem of lack of access to quality health care is linked with wasteful use of primary care services at referral centres. In the rural communitieswhere the burden of disease morbidity and mortality is high, efficient health expenditure and service utilization is plagued by the absence of adequately functioning Primary Health Centers (PHCs), poor or inadequate cost sharing schemes and due to corrupt practices in the health sector. In order to curb these issues, policy options such as revamping the PHC and prioritizing the delivery of a basic minimum package of health care are useful to consider. Furthermore, the implementation of strong actions to tackle corruption in the health sector will improve access to care and health outcomes and it does not incur extra financial investment. This is achievable through improvement in public financial management and limiting corruption by making right choices in resource allocation towards pro-poor interventions. Similarly, well designed package of services and prioritization of primary care making best use of human resource will be beneficial. This is relevant to the Nigerian health system, leveraging the country's decentralized administration and strengthening community health committees' role in ensuring accountability and transparency at the PHCs. Finally, considering the role community health committees play in driving demand in rural communities, the National Primary Health Care Development Agency (NPHCDA) can coordinate the development of a joint action plan for health care delivery between these committee(s) and each respective PHC facility. This will promote efficient use of resources and facilitate access to quality health care at each facility.
Nigeria is placed at 142 out of 195 countries according to a Lancet report´s ranking of health systems performance using healthcare access and quality as its criteria. Nigeria also ranks poorly based on the World Bank's Universal Health Coverage Service Coverage Index [1,2]. Although access to healthcare for all Nigerians through the basic minimum package of health services is backed by the National Health Act, the package has faced huge challenges in dissemination and implementation as several State Governments are lagging in operationalizing it at ward levels [3,4]. Furthermore, there is underutilization and bypassing of the primary health care facilities, as people prefer to use the hospitals. The gate keeping function of the PHC is made redundant mainly due to ineffective linkages between the different tiers of the health system. In many cases, patients prefer to visit the secondary and the tertiary health centers, but they are more expensive and this worsens health care accessibility especially among the poor in the society [5-7].
Primary health care is set-back due to weak governance and accountability systems, poorly remunerated health care workers, and transparency mechanisms and procurement laws which are weakly enforced. The suggestion that the Nigerian health sector is one of the worst sectors in terms of corrupt rating is plausible given the estimated 25% of the country´s current health expenditure of about 221 per capita in purchasing power lost due to corruption. This includes both private and public health expenditure [8-12]. Notably, where corruption exists, the implementation of actions to ensure effective delivery of health care often fails [12]. This is reflected in the increased cost of health services, stock-out of essential drugs and avoidable mortalities in health facilities, especially at the PHCs in the country [9,13]. The Federal Ministry of Health's ability to effectively superintend the health sector is weakened due to the lack of adequate information on health outcomes, health resources, costs and the utilization of services across the various tiers including the federal, state and local levels [14]. Our considerations on what is needed to position the country for the attainment of the Universal Health Coverage Targets include revamping and positioning of the PHC as an effective gatekeeper in the health system, government prioritization of a benefit package of services and even more importantly, strong actions against corruption to ensure wider delivery of quality health care in Nigeria. Critical to this, are the roles that multiple stakeholders play in the delivery of health care in the country. Stakeholders such as Federal and State Ministries of Health, the Local Government Authorities, the health workers, the National Primary Health Care Development Agency, the State Primary Health Care Development Agency, the Economic and Financial Crimes Commission, and Service Compact with All Nigerians
Revamping and repositioning the primary health centers: globally it is recognized that the PHCs provide an efficient and equitable means of health care delivery due to its pro-poor services [15]. The Nigerian Government thus prioritized revitalization of PHCs spread across the 774 Local Governments as a necessary step towards universal health coverage in the country [16]. Similarly, Government prioritised funding of preventive programs are usually targeted at the PHCs and this includes programs such as immunization, roll back malaria and control of the spread of HIV/AIDS [17]. The WHO advises that investments in PHC will lead to more equity and efficiency in the health system due to the financial protection it offers through cheaper costs of health services [18]. This implies that a policy that seeks to revamp the PHCs to perform its gatekeeping function of attending to more patients will result in more efficient use of resources within the Nigerian health sector. Additionally, considering the statutory transfer of funds via the Basic Health Care Provision Fund (50% of the 1% consolidated revenue for strengthening the PHC) for essential drugs, vaccines, human resource and infrastructure maintenance, unused funds as a result of delayed release of funds, poor uptake or demand can be rolled over [16]. But the level of implementation of this means of funding as well as a corresponding efficient spending remains doubtful. There is a recognizable feasibility gap in the revitalization of the PHCs which could lead to skepticism among stakeholders because of the economic challenges the country faces. The country experienced a recession in 2016-2017, from which it is gradually coming out of and yet again faces the humongous economic impact of the COVID-19 pandemic [16,19].
Government prioritization of the basic minimum package of health services: the National Strategic Health Development Plan II recommends the elimination of financial hardship at the health care provider points through the operation of the National Health Insurance Fund which provides a basic minimum package of health services for all Nigerians [16,20]. The package comprises emergency care, treatment of diabetes, hypertension, routine immunization, care for illnesses among children below five, emergency obstetric and neonatal care, labour and delivery, elective caesarian section and antenatal care. These interventions are to be provided without costs at the points of delivery [21]. The operation of this package through the National Health Insurance Scheme (NHIS) is aimed at reducing health service inequity through its pro-poor operations especially in the rural communities to improve access and quality of care [21]. The scheme is meant to offer progressive universalism in health care delivery, providing minimum services to a larger population. Funding of the NHIS aids the purchase of affordable and effective interventions to be provided by private and public providers for about 60% of the current burden of diseases [14]. This is from the remaining 50% of the basic health care provision Fund (1% of the consolidated revenue fund) [16]. The country's general fiscal space is however about 12% of the Gross Domestic Product, which implies that the Basic Health Care Provision Fund (BHCPF) 0.12% and thus the NHIS receives 0.06%. This size of fiscal space is small when compared with the average for low- and middle-income countries between 20 and 25% [11]. Funding of the scheme should thus be complemented by the larger pool of funds from the general taxes which comprises 14% of the current expenditure [11]. This will increase access to care for the most vulnerable population. It is also more rational to explore more state government involvement in the expansion of the insurance scheme.
The state government's prioritization of the basic minimum package through payroll tax financing of social health Insurance is hinged on the constitutional autonomy that the State Governments possess [7]. State governments are expected to commit 0.5-1% of their consolidated fund towards funding of the PHC while 50% passes through the National Health Insurance Fund as a scheme they operate. But currently, the State led scheme is at different stages of operationalization and only 24% of the states have the scheme operationalized. This discrepancy is related to the differences in each State´s pool [16]. Furthermore, operationalizing the scheme involves the agreement between the providers and the insurance scheme (purchasers) on the type of services and tariffs after accreditation is conducted yearly and since accredited facilities which are accredited are the sole selected providers regardless of location, equity will be constrained especially if the facilities are not accessible. To avoid delays which are linked with a bureaucratic central administration, and complaints about deficiencies in service provision while ensuring quality improvement, the decentralization of the administration of the health insurance scheme has been suggested [15].
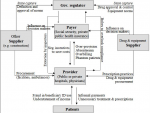
Strong actions against corruption in the Nigerian health sector: a recent systematic review of corruption in the Nigerian health sector [9], identified the most prevalent forms of corruption in the sector. These includes drug malpractices, absenteeism, bribes (informal payments), and embezzlement of money among others (Figure 1). The promulgation of a policy on strong actions against corruption comes at an opportune time with the change in the political climate in the country. The current government is determined to combat corruption and it has been argued that more holistic and transparent measures combined with citizenry involvement will be needed to achieve its objective [22]. Anti-corruption actions in the health sector are supportable activities that countries in Africa have adopted and adapted according to their country context and pressing need. Uganda, Malawi, Tanzania are countries with successful implementation [23]. In Uganda, anti-corruption campaign also influenced government decision such that a separate budget line was approved for the National Medical Stores guaranteeing less fragmentation and fewer bottlenecks for the procurement of medicine with increased resources. Due to weak law enforcement in the country, it was noted that more effort is still needed to enforce sanctioning and follow-up of cases of corruption [23].
The effectiveness of anti-corruption actions through “down-top” approaches have worked in a similar low- and middle-income country, Uganda which also ranks poorly at 137 on the corruption perception scale of transparency international [23,24]. In a project conducted in communities which utilized a PHC, about 50% absenteeism was noted in the facility. The members of the community agreed to develop an action plan to oversee the improvement of health outcomes at the facility and indeed recorded a 30% decrease in infant mortality, a 20% increase in outpatient visit after a year and a 28% infant mortality decrease after 4 years. This impact was largely due to the monitoring of the action plan through informal community censorship and criticisms where necessary but without extra government financial support or drug supply to the facility [25]. Judging the feasibility of a policy against corruption, evidence from literature reveals that specific actions to strengthen governance at the community level through monitoring at public hospitals can effectively check absenteeism [25]. Similarly, with the improvement of remunerations and provision of resources, the incentive to obtain bribes is reduced [9,26].
We believe that by complying with the WHO recommendation of a legal framework and a supportive environment for universal health coverage (UHC) [27,28], Nigeria will need to establish anti-corruption measures that will govern the health sector. This will support the approach of a “top-bottom” approach to governance. Similarly developing joint action plans at community levels will support complementary “bottom-top” approaches. A strict compliance will eliminate the risk of having officials - who assume to be above the rule of law - evade sanctions and dismissals if found culpable. Effective top-down governance of the health sector would be fulfilling the SDG 16.5 Actions against corruption can be implemented in phases like the WHO suggested in the case of good governance for medicines. A standard approach ab initio is to conduct a vulnerability assessment systematically, to determine areas of priority in the health sector and guide strong actions [27]. Tracking and measurement of corruption within the health sector can be followed up using public expenditure and financial accountability indicators as well as public expenditure tracking surveys and reviews [27]. This would also minimize inefficient spending on interventions of low cost-effectiveness and consequently avoid waste.
Strategic actions such as revamping the PHCs and prioritizing the basic minimum package delivery through National and State-driven insurance schemes are important in filling up policy gaps for optimizing health care delivery. But without strong actions against corruption in Nigeria, UHC remains aspirational and not realistic. While revamping PHCs is in line with global recommendations as an efficient route to UHC, the economic realities in the country make it less feasible. Similarly, prioritisation of the basic minimum package through State operationalization of cost-sharing schemes would support wider coverage, but its implementation is delayed at the States. It is a relevant call for action in the Health sector and practicable through an initial vulnerability assessment of the health sector. While more local evidence needs to be generated to guide concrete steps, political support will also be essential in driving this policy by ensuring appropriate sanctions against corrupt practices were necessary to produce a measurable impact.
Recommendations: 1) A measurement of the extent of sector-level involvement in corruption is required. Appropriate tools must be harnessed to assess the impact and to track corruption in the health sector. Tools including assessments of vulnerability, Public Expenditure and Financial Accountability Indicators (PEFA), Public Expenditure Tracking Surveys and Reviews (PERS) are useful. 2) The Ministry of Health to adopt a combination of top-down as well as down-top approaches against corruption. Resistance to a top down approach will be complemented by a corresponding community-led down-top approach with media sensitization campaign for the general public on the awareness of a fight against corruption in the health sector. 3) Multi-sectoral collaboration and partnership with the anti-corruption agencies in the country including the Economic and Financial Crimes Commission (EFCC), Independent Corrupt Practices Commission will be essential in enforcing sanctions against corrupt practices in the health sector. This is to connect the policy to broader policies against corruption in the country. Similarly supporting SERVICOM to effectively carry out its duty of bridging the gap between health care performance and the expectation of patients in health facilities is necessary. 4) Focus on PHC and State Primary Health Care Development Agency (SPHCDA) to oversee the development of strong community engagement and participation at the primary health centers. The following steps: a) Build a community engagement platform: identification of functional PHC in each local government area spread across the geo-political zones in the country. Identification of community health committees at each local government area. These committees, which are important drivers for health care demand, should comprise of a wide spectrum of persons from the respective local government. They should include religious leaders, teachers, chiefs, members of the town's royalty, adolescents, civil society organisation, volunteers from the women's group and men's group. Media campaign and sensitization on the anticorruption movement in each respective local government should be conducted. b) Develop a joint action plan: through an organised series of interactive sessions including focused group discussions between the community health committees and the health workers in the chosen health facility. This will reduce the likelihood of information asymmetry as the major challenges affecting the delivery of quality health services to the local government would be identified. It is important to establish that the solutions to these problems are not dependent on extra funding to the functional PHC. The joint action plan should then be formulated. This plan will highlight what works for efficient delivery of minimum services, who is responsible (the health workers in the health facility) and how this is to be carried out. c) Focus on impact assessment: the SPHCDA will be responsible for developing qualitative and quantitative methods of evaluating changes such as improved health worker presence, medicine availability, patient utilization of services and health outcomes at the health facility.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Figure 1: the multifaceted nature of corruption in the health sector according to Savedoff W.D and Hussmann K as cited by Karren Hussman [27:pg 10]
- Fullman N, Yearwood J, Abay SM, Abbafati C, Abd-Allah F, Abdela J et al. Measuring performance on the Healthcare Access and Quality Index for 195 countries and territories and selected subnational locations: a systematic analysis from the Global Burden of Disease Study 2016. Lancet. 2018 Jun 2;391(10136):2236-2271. PubMed | Google Scholar
- World bank. UHC service coverage index-Nigeria. 2017. Accessed on Jun 3, 2020.
- Federal Government of Nigeria. Second national strategic health development plan 2018-2022. Accessed on May 28, 2020.
- Wright J. Essential Health Services: Nigeria. 2015. Accessed on May 28, 2020.
- Federal Ministry of Health. Saving new born lives in Nigeria: newborn health in the context of the integrated maternal, newborn and child health strategy. 2011. Accessed on May 28, 2020.
- Abimbola S, Oyedeji R. How tertiary hospitals can strengthen primary health care in Nigeria. Niger Med J. 2014;55(6):519-528. PubMed | Google Scholar
- Okpani A, Abimbola S. Operationalizing universal health coverage in Nigeria through social health insurance. Niger Med J. 2015;56(5):305-335. PubMed | Google Scholar
- Garuba HA, Kohler JC, Huisman AM. Transparency in Nigeria's public pharmaceutical sector: perceptions from policy makers. Globalization and health. 2009 Dec 1;5:14. PubMed | Google Scholar
- Onwujekwe O, Orjiakor CT, Hutchinson E, McKee M, Agwu P, Mbachu C et al. Where do we start? Building consensus on drivers of health sector corruption in Nigeria and ways to address it. Int J Health Policy Manag. 2020 Jul;9(7):286-351. PubMed | Google Scholar
- World Health Organization. The world health report: health systems financing: the path to universal coverage. Accessed 2020 Jun 5, 2020.
- World Health Organization. Health accounts. Accessed Jul 18, 2020.
- Tormusa DO, Idom AM. The impediments of corruption on the efficiency of healthcare service delivery in Nigeria. Online Journal of Health Ethics. 2016;12(1):3. Google Scholar
- Bruckner T. The ignored pandemic: how corruption in healthcare service delivery threatens Universal Health Coverage. Transparency International UK, London. 2019. Accessed on May 28, 2020.
- Hafez R. Nigeria health financing system assessment. 2018. Accessed on Jul 6, 2020.
- Resilient & Responsive Health System. Strategic purchasing for universal health coverage: a critical assessment. The Nigerian Formal Sector Social Health Insurance Programme (Fsship). 2016. Accessed on Jun 5, 2020.
- Federal Republic of Nigeria. Implementation of the SDGs: a national voluntary review. Eradication of poverty and promoting prosperity in a changing world. 2017. Accessed on June 5, 2020.
- Uzochukwu B. Case study from Nigeria Primary Health Care Systems (Primasys) Primary Health Care Systems (Primasys). 2018. Accessed on Jun 4,2020.
- Fore HH, Gurría JÁ. Primary health care on the road to universal health coverage: 2019 monitoring report. Accessed on Jan 20, 2021.
- Ozili PK, Arun T. Spillover of COVID-19: impact on the global economy. SSRN Electron J. 2020 Mar 31. Google Scholar
- Federal Government of Nigeria. Second national strategic health development plan 2018-2022. 2018. Accessed on Jan 20, 2021.
- Basic Healthcare Provision Fund. Guidelines for the administration, disbursement, monitoring and fund management of the basic healthcare provision fund. 2016. Accessed on Jan 20, 2021.
- Onya Rr, Elemanya Av. Analysis of president Buhari's anti-corruption policy: a reality or an illusion. International Journal of Advanced Academic Research Social and Management Sciences. 2016;11(2):82. Google Scholar
- UNDP. Fighting corruption in the health sector methods, tools and good practices. 2011. Accessed on Jan 20, 2021.
- Transparency International Uganda. Accessed on May 31, 2020.
- Björkman Nyqvist M, De Walque D, Svensson J. Experimental evidence on the long-run impact of community-based monitoring. American Economic Journal: Applied Economics. 2017 Jan;9(1):33-69. Google Scholar
- Onwujekwe O, Dike N, Uzochukwu B, Ezeoke O. Informal payments for healthcare: differences in expenditures from consumers and providers perspectives for treatment of malaria in Nigeria. Health policy. 2010 Jun 1;96(1):72-79. PubMed | Google Scholar
- Hussmann K. Addressing corruption in the health sector securing equitable access to health care for everyone. 2011. Accessed on Jun 1, 2020.
- World Health Organization. Integrating a focus on anti-corruption, transparency and accountability in health systems assessments. 2018. Accessed on Jan 20, 2021.