Spatial analysis of confirmed Lassa fever cases in Edo State, Nigeria, 2008 - 2014
Owoicho Samuel Amifofum, Dorcas Fadugba, Emmanuel Awosanya, Adebudo Icomiare, Kingsley Evbuomwan, Muhammad Shakir Balogun, Patrick Nguku, Whenayon Simeon Ajisegiri, Amienwanlen Eugene Odigie, Babasola Olugasa
Corresponding author: Owoicho Samuel Amifofum, Nigeria Field Epidemiology and Laboratory Training Programme, Abuja, Nigeria 
Received: 30 Jun 2020 - Accepted: 24 Jun 2021 - Published: 29 Jun 2021
Domain: Epidemiology,Infectious diseases epidemiology,Public health
Keywords: Mastomys, hotspot, spatial analysis, lassa fever, environmental variables
©Owoicho Samuel Amifofum et al. PAMJ-One Health (ISSN: 2707-2800). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Owoicho Samuel Amifofum et al. Spatial analysis of confirmed Lassa fever cases in Edo State, Nigeria, 2008 - 2014. PAMJ-One Health. 2021;5:11. [doi: 10.11604/pamj-oh.2021.5.11.24710]
Available online at: https://www.one-health.panafrican-med-journal.com/content/article/5/11/full
Spatial analysis of confirmed Lassa fever cases in Edo State, Nigeria, 2008 - 2014
Owoicho Samuel Amifofum1,2,&, Dorcas Fadugba2, Emmanuel Awosanya1,2, Adebudo Icomiare1,2, Kingsley Evbuomwan2, Muhammad Shakir Balogun1, Patrick Nguku1, Whenayon Simeon Ajisegiri1, Amienwanlen Eugene Odigie2, Babasola Olugasa2
&Corresponding author
Introduction: lassa fever (LF) is endemic and poses public health threats in Edo State. Identification of primary clusters (hotspot) will help prioritize public health interventions in the state. We investigated retrospective cases of LF to identify primary cluster of the disease for household exposure management.
Methods: we reviewed retrospective data (n = 1400) of LF case-patients at a referral hospital in Edo State from 2008 to 2014 based on World Health Organization case definition for LF. We determined hotspot of confirmed cases on Bernoulli model and evaluated environmental factors in the hotspot: presence of rodent deterrents, proximity of households at 2 km radius to rice farm, rice post-harvest storage facility, refuse dump, forest, hospital and main road using multi-criteria analysis at p < 0.05.
Results: of the reviewed cases, 171 (12.2%) were confirmed case-patients. The median age of confirmed case-patients was 30 years (Q1:16.0 and Q3: 43.5). Of the confirmed case-patients, 101 (59.1%) were male. Hotspot (4.45 km radius; geographic center at 6.717900°N, 6.243500oE) was identified in Esan West LGA. Associated environmental factors included proximities of households to refuse dump (p < 0.001), rice post-harvest storage facility (p = 0.01) and rice farm proximity to households (p = 0.03) were significant to cases in Esan west.
Conclusion: Esan West LGA was identified as a hotspot for Lassa fever, household proximity to refuse dump sites, rice storage facilities and rice farms were associated environmental factors. We recommend improved rice post-harvest storage, distancing rice farms from households and adhering to strict environmental sanitation in Edo State, Nigeria.
Lassa fever (LF) is a viral haemorrhagic zoonotic disease caused by an arenavirus. Humans get infected with the virus primarily through ingestion of food or food substances contaminated with the excreta of Mastomys natalensis rodent (commonly known as the multimammate rat), which is the natural reservoir for the virus. Human to human transmission is also possible through contact with secretions and excretions of infected persons [1]. Lassa fever (LF) is predominant in West Africa including Sierra Leone, Liberia and Nigeria [2]. It affects 100,000 to 300,000 people every year in this region [3]. There have been several LF outbreaks in various parts of Nigeria and the largest outbreak ever reported was in 2018 which shows an increasing trend in the number of cases and deaths [4]. In 2018, a total of 3016 suspected LF cases were reported from 22 states. Of these cases, 559 were confirmed positive, 17 probable and 2440 negative. The case fatality rate among confirmed cases was 25.6% and 100% among probable cases. All the affected 22 states had at least one confirmed case spreading through 90 Local Government Areas (LGAs). Three of the 22 affected states constituted 83.0% of the confirmed cases: Edo (46%), Ondo (24%) and Ebonyi (13%) states [4]. Edo State is one of the states in Nigeria with high burden of LF cases with occurrence all through the year. The first outbreak of LF in Edo State occurred in Esan West LGA in 1989 [3,5]. Identification of primary spatial clusters have contributed immensely to understanding disease risk behavior as well as help guide and inform prioritization of public health intervention strategies [6]. Studies have indicated that habitat suitability such as agricultural intensification associated with post-harvest grain, storage density on residential areas could significantly influence Mastomys breeding and transmission of the Lassa virus to humans [1,7]. Geographic information system (GIS) and spatial models have been used to gain better understanding about the risk distribution of LF along West Africa sub-region [7]. This study, therefore, aimed at identifying hotspot for confirmed LF cases in Edo State, an endemic LF state, and its´ associated environmental factors in the hotspot.
Study design: a retrospective review of data on LF cases presented at the Irrua Specialist Teaching Hospital, Edo State between 2008 and 2014.
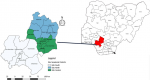
Study location: Edo State is one of the states in the South - south geo-political zone of Nigeria; lying on 05´44 N and 07´34 N latitudes, 05´ 4 E and 06´45 E longitudes (Figure 1), and mostly tropical rain forest. Administratively, it has 3 senatorial zones (Edo North, Edo Central and Edo South), 18 LGAs and 192 wards. The 2018 projected human population for Edo State from the 2006 national population census was 4,600,000. Agriculture is the main occupation of the people [8]. Edo State has 472 health facilities with 55 private health facilities and the Institute for Lassa fever Research and Control situated at Irrua in Esan Central LGA.
Case definition: lassa fever case was established based on the World Health Organization (WHO) definition, 2004.
Suspected case: a suspected case was a person with acute illness of <3 weeks duration, with temperature of 38°C and above, showing no response to effective antimalarial treatment after the first dose and no response to chloramphenicol treatment afters 48 hours [9].
Probable case: a probable case was a person with clinical illness, not laboratory confirmed and was not epidemiologically linked to a confirmed case but with appropriate exposure history.
Confirmed case of LF: a confirmed case of LF was a person that was confirmed in the Laboratory, or that met the clinical illness case defined by the WHO and was not laboratory confirmed case but epidemiological linked to a confirmed case.
Controls: suspected cases that were tested negative in corresponding locations in which confirmed cases were located.
Primary cluster (hotspot): geospatial areas with high prevalence or efficient transmission of disease are known as primary clusters or hotspots.
Data collection: all cases obtained from the retrospective record were reviewed at Irrua Specialist Teaching Hospital, Edo State, a total of 1,400 suspected, probable and confirmed cases. Data on the age, sex, house location and laboratory status were extracted for all laboratory confirmed cases. We visited house locations of confirmed LF case-patients and controls and geographic coordinates of their house locations were obtained using the handheld geographic positioning system (GPS), geographic coordinates were also captured using Google Earth Pro images for geo-positioning. Data on age, sex, number of cases and geo-coordinates in each LGA were line listed on Microsoft Excel spreadsheet. After determining the hotspot for LF cases, an observational check-list was used to assess environmental risk factors of case-patients´ households in the hotspot. We considered environmental risk factors that could favor the breeding and access of mastomys rat such as proximity of household to rice farms, rice post-harvest storage facilities, refuse dump sites and presence of rodent deterrents [7]; and other environmental factors such as proximity of households to forest, main road and hospital facilities. By presence of rodent deterrents: we observed the houses of LF case-patients for absence of cracks and crevices in the windows, doors and walls. All proximities were considered at 2 km radius of the house locations of confirmed LF case-patients to any of the environmental factors considered.
Data analysis: Kulldorff Sat Scan software was used to estimate primary clustered (hotspot) location. Associated environmental factors of LF cases in the hotspot were determined using spatial regression with Geoda software. Eight spatial features were individually tested as predictors of LF cases in the primary clustered area through multi-criterial analysis (MCA) [1]. Spatially lag independent variables were grouped into two subsets to reveal the effects of groups 1 and 2 characteristics separately. Group one examined the effects of environmental variables related to residential areas at proximity of 2 km, while group 2 examined the rodent dynamics related variables. Variables were subjected to regression equation:
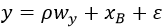
[10,11] where: y is an x by 1 Lassa fever case, wy is referred to as a spatial weights matrix. For each location in the system, it specifies which of the other locations in the system affect the value at that location. This is necessary, since in contrast to the unambiguous notion of a “shift” along the time axis (such as yt-1 in an autoregressive model), there is no corresponding concept in the spatial domain, especially when observations are located irregularly in space. Instead of the notion of shift, a spatial lag operator is used, which is a weighted average of random variables at “neighboring” locations, in conclusion, wy is a spatial weighted matrix of neighboring locations of the regression model, p is the scalar spatial coefficient, wy is an N by 1 weighted matrix of Lassa fever cases, X is an N by k matrix of explanatory variables (X1 forest proximity, X2 Household proximity to main road, X3 Hospital proximity and X4 is human population density). B is a k by 1 vector of parameters, ε is an N by 1 vector of random error terms. Data were analyzed at p < 0.05(11).
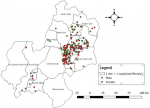
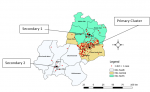
Of the 1,400 case records for LF reviewed; 171 (12.2%) were laboratory confirmed. Of the 171 confirmed cases, 101 (59.1%) were male. Figure 2 showed the spatial distribution of cases by sex. The median age of the confirmed case-patients was 30 years (IOQ: 27.5). Most (32.8%) affected age group was within 25 - 34 years and most (43.2%) of the confirmed case-patients were from Esan West LGA (Table 1). Hotspot (2km radius; geographic centre at 6.717900°N, 6.243500°E) for LF cases was identified in Esan West LGA (p = 0.04 and LLR = 4.23) (Table 2) (Figure 3). Environmental variables related to rodent dynamics that significantly characterized house locations of LF case-patients were proximities of households to refuse dump (p < 0.001), rice post-harvest storage facility (p = 0.01) and rice farm proximity to households (p = 0.03). However, other environmental variables such as proximity of households to forest, main road and hospital facilities were not significantly associated with house locations of LF case-patients (Table 3).
A significant hotspot for LF cases was identified in Esan West LGA, Edo State Nigeria in this study, while Secondary 1 cluster comprises of Etsako west and Secondary 2 clusters were found in Oredo, Ikpoba - okha and Egor Local Government Areas. This is similar to the findings of Igbinosa and Akpade [12,13] who reported LF hotspot in Ekpoma town in Esan West LGA in the same study location. This is an indication of the endemicity of LF virus in Esan West LGA. The identification of hotspot in Esan West LGA finds application in planning and strategic intervention for the effective prevention and control of LF in Edo State [5]. It could also suggest the source of rodent-human contact interface as reported by Karan [14] who highlighted four hotspots for LF among Mastomys natalensis population in Guinea and found a major hotspot around marketplace suggesting the source of Mastomys natalensis to human households in the study location. One of the environmental risk variables related to rodent dynamics that significantly characterized house locations of LF case-patients was proximity of rice post-harvest storage facility. Post-harvest storage facilities for grains have been found to attract rodents especially Mastomys natalensis [1]. Similarly, Olugasa [1] found significant risk association between rice storage post-harvest and LF outbreaks on a rubber plantation in Liberia. Grains such as rice serve as food to rodents and will encourage their presence in the surrounding of the storage facility especially where the hygiene practice is poor and no rodent control is in place. However, rodent-human interface is essential for disease transmission via ingestion of food or food substances contaminated with the excreta of LF infected Mastomys natalensis rodents. During pre-harvest season when the source of food to the rodents are either absent or inadequate, they migrate to households in the proximity in search of food, thus creating the rodent-human interface needed for possible disease transmission. In a study in Sierra Leone, more rodents were trapped within household than the environment and most of the trapped rodents were predominantly Mastomys natalensis [1].
Our model also revealed that the presence of rodent deterrents in households was found to be a significant protective factor associated with LF case-patients. Absence of cracks in walls, spaces either through the windows or doors, presence of wire mesh have been reported to be effective in breaking the rodent-human interface needed to provide disease transmission pathways. J. Kay Raymond [15] found the presence of rodent burrows and external hygiene around houses to be directly associated with a history of LF in the household in Sierra Leone. Though, a study in Sierra Leone found no significant difference in households of LF positive cases and controls with respect to housing quality [16]. Other significant environmental variables in our model included rice farms and refuse dumps in proximities of 2 km radius to the house locations of confirmed LF case-patients. Rice farms and refuse dumps sites have been reported to harbour rodents especially Mastomys natalensis because of the availability of food at these sites. However, Karan reported a preponderance of Mastomys natalensis in residential areas in Urban centers in Guinea [14]. Other environmental variables such as proximity of households to forest, main road and hospital facilities were not significantly associated with house locations of LF case-patients. This is similar to the findings of Olugasa in Liberia [1]. Rodent population size is limited by several factors which include food quantity and quality, presence of nesting sites, control activities etc [17]. Esan West LGA was identified as a hotspot for LF. Environmental factors related to rodent dynamics were associated with LF clusters in Edo State and the presence of post-harvest rice storage was observed as a risk factor associated with households of case-patients in the hotspot. Presence of rodent deterrents in some households were protective environmental factors associated with possible existence of Mastomys natalensis that could initiate cases in those households despite the high number of cases recorded. We recommend use of rodent proof rice post-harvest storage facility, distancing of rice farmlands from residential areas and public enlightenment on environmental sanitation in Edo State, Nigeria.
Esan West LGA was identified as a primary cluster for Lassa fever cases in Edo State. Household proximity to refuse dump sites, rice storage facilities and proximity to rice farms were associated environmental factors to lassa fever cases across the clusters.
What is known about this topic
- Edo central senatorial district observed as hotspot of Lassa fever in this study was previously discovered in studies by other Authors like Asogwu et al;
- Poor environmental sanitation and other factors contributed in the presence of rodents in homes where cases of Lassa fever are predominant was already published from previous researches.
What this study adds
- This study further indicated the Local Government Area where the was located in the senatorial district mentioned and could help in policy making by the government to narrowing most of her resources to the most affected community and environs to containing the spread of LF;
- The reviewed periods of hospital cases of Lassa fever in this study and that by other researchers varies;
- Classification of clusters of cases into primary, secondary 1 and Secondary 2 clusters within the various Local Government Areas in Edo State was clearly defined on the attached Maps using Satscan software.
The authors declare no competing interests.
OSA: conceptualized and designed the study, collected, analyzed and interpreted the data and drafted the initial manuscript; FD: contributed in data collection and cleaning; EA: critically guide, reviewed and revised the manuscript; AI: collected data and discuss the result; KE: collected data and took part in writing the background of the study; MSB: critically reviewed and revised the manuscript for important intellectual content; PN: reviewed the manuscript and made recommendation; WSA: critically reviewed the manuscript for intellectual content; AEO: participated in data analysis and reviewed the manuscript; BO mentored me in the entire processess of the research. All the authors have read and agreed to the final manuscript.
I acknowledge the following persons in ensuring the success of this publication: Dr Icomiare Adebudo, Dr Irowa Abiodun, Mrs Oboro Kehinde, Dr Ogunro Bamidele and Dr Chukwuma Umeokonkwo.
Table 1: socio-demographic and distribution of confirmed Lassa fever cases by age, gender and LGAs in Edo State, 2008 - 2014
Table 2: spatial cluster of confirmed Lassa fever cases in Edo State, 2008 - 2014
Table 3: multi-factorial characteristics of confirmed LF primary cluster in Esan west Local Government Area, Edo State, 2008 - 2014
Figure 1: map of Nigeria showing the location of Edo State
Figure 2: dot map of confirmed Lassa fever cases by sex distribution in affected Local Government Areas in Edo State, 2008 - 2014
Figure 3: map showing the spatial distribution of confirmed Lassa fever cases in Edo State, 2008 -2014
- Olugasa BO, Dogba JB, Ogunro B, Odigie EA, Nykoi J, Ojo JF et al. The rubber plantation environment and Lassa fever epidemics in Liberia, 2008-2012: a spatial regression. Spat Spatiotemporal Epidemiol. 2014 Oct;11:163-74. PubMed | Google Scholar
- Bond N, Schieffelin JS, Moses LM, Bennett AJ, Bausch DG. A historical look at the first reported cases of Lassa fever: IgG antibodies 40 years after acute infection. Am J Trop Med Hyg. 2013 Feb;88(2):241-4. PubMed | Google Scholar
- Asogun DA, Adomeh DI, Ehimuan J, Odia I, Hass M, Gabriel M et al. Molecular diagnostics for Lassa fever at Irrua Specialist Teaching Hospital, Nigeria: lessons learnt from two years of laboratory operation. Bausch DG, editor. PLoS Negl Trop Dis. 2012 Sep 27;6(9):e1839. PubMed | Google Scholar
- Ilori EA, Frank C, Dan-Nwafor CC, Ipadeola O, Krings A, Ukponu W et al. Increase in Lassa fever cases in Nigeria, January-March 2018. Emerg Infect Dis. 2019 May;25(5):1026-7. PubMed | Google Scholar
- Tobin E, Asogun D, Akpede N, Adomeh D, Odia I, Gunther S. Lassa fever in Nigeria: insights into seroprevalence and risk factors in rural Edo State: a pilot study. J Med Trop. 2015;17(2):51. Google Scholar
- Moise IK, Kalipeni E. Applications of geospatial analysis to surveillance data: a spatial examination of HIV/AIDS prevalence in Zambia. Geo Journal. 2012 Aug 4;77(4):525-40. Google Scholar
- Olugasa B, Dogba J. Mapping of Lassa fever cases in post-conflict Liberia, 2008-2012: a descriptive and categorical analysis of age, gender and seasonal pattern. Ann Afr Med. 2015;14(2):120. PubMed | Google Scholar
- Businessday NG. Edo farmers get N5bn investment for cultivation of over 10,600ha. Accessed July 11, 2020.
- WHO. Lassa Fever - Nigeria. WHO. 2017.
- Anselin L, Syabri I, Kho Y. GeoDa: an Introduction to spatial data analysis. Geogr Anal. 2006 Jan 1;38(1):5-22. Google Scholar
- Anselin L. Spatial econometrics. A Companion to Theoretical Econometrics. 2001.
- Igbinosa E. Detection of clusters and geographical hotspot for Lassa fever in Edo Central Senatorial district of Nigeria: a step into a nation-wide mapping of Lassa fever. Int J Infect Dis. 2016;45:227. Google Scholar
- Akpede GO, Asogun DA, Okogbenin SA, Okokhere PO. Lassa fever outbreaks in Nigeria: expert Rev. Anti Infect Ther. 2018 Sep 2;16(9):663-6. PubMed | Google Scholar
- Karan L, Makenov M, Korneev M, Sacko N, Boumbaly S, Bayandin R et al. Lassa virus in the host rodent mastomys natalensis within urban areas of N´zerekore, Guinea. bioRxiv. 2019;616466. Google Scholar
- Richmond JK, Baglole DJ. Lassa fever: epidemiology, clinical features, and social consequences. BMJ. 2003;327:1271-5. Google Scholar
- Bonwitt J, Sáez AM, Lamin J, Ansumana R, Dawson M, Buanie J et al. At home with mastomys and rattus: Human-rodent interactions and potential for primary transmission of lassa virus in domestic spaces. Am J Trop Med Hyg. 2017;96(4):935-43. PubMed | Google Scholar
- Massawe AW, Makundi RH. The type of farming practice may affect the movement and reproduction pattern of rodents in crop fields: a case study of Mastomys natalensis. J Biol Sci. 2011;11(1):22-30. Google Scholar