Does knowledge of danger signs influence use of maternal health services among rural women? Findings from Babati Rural district, Northern Tanzania
Edwin Joseph Shewiyo, Minael Gad Mjemmas, Faidha Haruna Mwalongo, Ester Diarz, Sia Emmanueli Msuya, Beatrice John Leyaro
Corresponding author: Edwin Joseph Shewiyo, Institute of Public Health, Department of Community Health, Kilimanjaro Christian Medical University College (KCMUCo), Moshi, Tanzania 
Received: 26 Jul 2020 - Accepted: 29 Nov 2020 - Published: 14 Jan 2021
Domain: Obstetrics and gynecology,Health Research,Maternal and child health
Keywords: Obstetric danger signs, knowledge, skilled birth attendance, birth preparedness and complication readiness, antenatal care
©Edwin Joseph Shewiyo et al. PAMJ-One Health (ISSN: 2707-2800). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Edwin Joseph Shewiyo et al. Does knowledge of danger signs influence use of maternal health services among rural women? Findings from Babati Rural district, Northern Tanzania. PAMJ-One Health. 2021;4:4. [doi: 10.11604/pamj-oh.2021.4.4.25206]
Available online at: https://www.one-health.panafrican-med-journal.com/content/article/4/4/full
Research 
Does knowledge of danger signs influence use of maternal health services among rural women? Findings from Babati Rural district, Northern Tanzania
Does knowledge of danger signs influence use of maternal health services among rural women? Findings from Babati Rural district, Northern Tanzania
![]() Edwin Joseph Shewiyo1,&, Minael Gad Mjemmas1, Faidha Haruna Mwalongo1, Ester Diarz2,3, Sia Emmanueli Msuya1,2,4, Beatrice John Leyaro2
Edwin Joseph Shewiyo1,&, Minael Gad Mjemmas1, Faidha Haruna Mwalongo1, Ester Diarz2,3, Sia Emmanueli Msuya1,2,4, Beatrice John Leyaro2
&Corresponding author
Introduction: increasing knowledge on obstetric danger signs (DS) among pregnant women and their fhmilies is one of the interventions targeted to reduce maternal and newborn mortality. It is expected that knowledge in DS will lead to early care seeking once complications occur among women or newborns. Health care providers are required to educate women on DS of obstetric emergency during pregnancy, delivery and immediate-post-delivery. This study aimed to determine the level of knowledge on danger signs among rural women and its effect on antenatal care visits, birth preparedness and complication readiness (BPCR) and on use of skilled birth attendance (SBA) during childbirth.
Methods: community-based analytical cross-sectional study was conducted in July 2019 among women who delivered in the past 24 months in two wards at Babati Rural district, Tanzania. Questionnaire was used for data collection. Odds Ratio was used to assess association between knowledge on danger signs with use of services during pregnancy and childbirth.
Results: a total of 372 women were enrolled, with mean age of 28.5 years (S.D 7.2). All the women attended antenatal care at least once during pregnancy, 65.3% attended ANC 4 or more visits, 85.2% of women were assisted by SBA during childbirth, and 13.7% of the women had birth preparedness and complication readiness plan. Overall, 272 (73.1%) women reported that they were counseled about obstetric danger signs during antenatal clinic visits, but only 32% could mention three or more DS of obstetric and newborn emergency. Overall good knowledge of DS and knowledge of obstetric danger signs during pregnancy were significantly associated with 4 or more ANC visits and birth preparedness and complication readiness but not with SBA use during childbirth.
Conclusion: majority of women were counseled on DS during pregnancy, however more than three quarters (68%) had low knowledge. Women who were knowledgeable on danger signs during pregnancy attended 4+ ANC visits and prepared for birth and its complications. There is a need of designing alternative models of engaging women during education counseling sessions so that they may have a higher retention of knowledge not only of danger signs but for other maternal and newborn health issues.
It is estimated that about 830 women die from pregnancy or childbirth-related complications around the world every day. Almost all of these deaths (99%) occurred in low-resource settings, and most could have been prevented [1,2]. While MMR has declined by 47% from 1990-2015, many sub Saharan African (SSA) countries have unacceptably high MMRs [3]. Tanzania, a country in East Africa has shown lack of progress in reducing the MMR. According to the Tanzania Demographic and Health Survey of 2015-2016 the estimated MMR was 556 per 100,000 live births which is higher than the MMR recorded in TDHS of 2010 which was 454 per 100,000 live births [4,5]. WHO estimates that 15% of all pregnancies will end with life-threatening complications and prediction of which women will end with complications is poor [6]. About 73% of all maternal deaths are due to direct obstetric causes which includes; hemorrhage that account for 27.1% of deaths, hypertensive disorders 14%, sepsis 10.7%, unsafe abortion 7.9%, embolism 3.2% and all other direct causes of death 9.6% [7]. Majority of these deaths can be prevented with timely access to quality emergency obstetric care (EmOC). Several factors have been cited to influence access to EmOC. Key among them is lack of fully functional EmOC facilities, poor skills of providers, socio-economic factors, distance, and lack of knowledge about obstetric danger signs which results in delay in seeking timely care for obstetric complications [8-10]. The three delays that affects maternal mortality in SSA including Tanzania includes delay in deciding to seek care, delay in reaching to seek care on time, and delay in receiving adequate treatment. The major causes for first delay are lack of awareness and knowledge about obstetric danger signs and consequence to decide to seek care among mothers and community [11-13].
Danger signs of obstetric emergency are warning signs and symptoms that women encounter during pregnancy, child birth and immediately after delivery that signifies a life-threatening complication [14,15] According to WHO and JHPIEGO, the key danger signs during pregnancy include: severe vaginal bleeding, symptoms and signs of severe preeclampsia like swollen hands or face, severe headache and blurred vision, convulsions/fits, and cessation of fetal movement to mention a few. Among the key danger signs during labor and childbirth include: severe vaginal bleeding, prolonged labor (>12 hours), convulsions, retained placenta, the key danger signs during the postpartum period include: severe vaginal bleeding, foul-smelling vaginal discharge and high fever [16]. It is important, to know these warning signs for women and health care providers in order to rule out serious complications and initiate treatment immediately [14]. In Tanzania the prevalence of knowledge of danger signs of obstetric emergency have shown to vary greatly from 7.4% to 57.8% [8,17-20]. Furthermore, the proportion of women with knowledge of danger signs among women is shown to be higher in urban setting (57.8%) [20], compared to rural settings (7.4%), (14.8%) [8,17]. Knowledge of DS in other SSA countries and Asia ranged from 26% - 61% [21-25].
Studies done in other SSA countries; Nigeria, Ethiopia, and Uganda have shown that women knowledge of obstetric danger signs influenced health care seeking behavior. A study in Gambia showed that lack of ability to identify danger signs during pregnancy by women was reported to result in delays in accessing obstetric care [26]. Others have shown knowledge of danger signs was associated with higher odds of attending for 4+ ANC visits, more likely to have better birth preparedness and complication readiness and higher SBA use during delivery compared to women with no or low knowledge [9,18,25,27,28]. Previous studies on obstetric danger signs in Tanzania have assessed prevalence of DS and its association with maternal socio-demographic and economic factors [8,18,19]. Only one study linked knowledge of DS and service utilization [20]. The concern is, does knowledge of danger signs influence use of maternal health services among rural women? Hence the aim of this study was to assess women's knowledge of danger signs of obstetric complications and its effect on 4 or more ANC visits, in having birth preparedness and complication readiness plan and in SBA use during childbirth at Babati rural, Manyara region, northern Tanzania.
Study design and site: the study was a community-based cross sectional study. Recruitment and data collection was conducted in July 2019, at Babati Rural district, situated in Manyara region in the northern Tanzania among women who had delivered within previous 24 months. Manyara region is divided into six districts which are Babati Rural, Babati Urban, Hanang, Kiteto, Mbulu and Simanjiro district. The administrative capital of the district is Babati town, 172 kilometers south of Arusha City. The Babati Rural district covers an area of 5,460 kilometers square, with a total population of 312,392 of which males are 158,804 and females are 153,588 according to the 2012 census report. Their main economic activities are small scale farming of maize and potatoes, livestock keeping and fishing business. Babati Rural district has 25 wards with 102 villages and 68,968 households. The district has 35 dispensaries, 7 health centers and 8 private hospitals. According to TDHS of 2015-2016, Manyara region has poor maternal and newborn indicators compared to the national level. For example; 45% of women had four or more ANC visits, skilled attendance during childbirth is at 48% and newborns receiving postnatal care within 48 hours was 26%, which is low compared to the National average of 4+ ANC visits of 51%, SBA use of 64% and PNC use of 34% respectively [5].
Study population, sampling and data collection procedures: the study population was women who gave birth in the past 24 months prior to the study in Babati Rural district and consented to participate in the study. The study excluded women who are not permanent residents in the study area. Sample size: Sample size for this study was estimated by using the formula for precision;
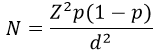
Where N is estimated minimum sample size; Z is confidence level at 95% (standard value is 1.96); P is expected proportion in population based on previous studies (knowledge of at least one danger sign) = 51% [17]; d is precision at 95 % CI = 0.05. The minimum sample that was required for this study was 384 women. Addition of 10% for non-response gave a minimum sample of 422 women delivered within previous 24 months to the study.
Sampling: multistage sampling technique was used to obtain women who participated in the study. The multistage sampling techniques involved the following stages. Stage 1: Babati rural district was selected purposively out of 6 districts of Manyara Region. Stage 2: two wards were randomly selected (Dareda and Magugu) out of 25 wards at Babati Rural district. Stage 3: at Magugu ward, 3 villages, Magugu, Mapea and Matufa, were randomly selected out of 7 villages. At Dareda ward, 4 villages, Bashnet, Gidewali, Maganjwa and seloto were randomly selected out of 12 villages. Stage 4: two hamlets were randomly selected from each village. At Magugu, 6 hamlets, Msimbazi, Majengo A, Majengo B, Mapea A, Mapea B and kwa rangi were randomly selected. At Dareda 8 hamlets, Bermi, Dabir, Endegau, Gisambalang, Mandi, Semak, Daktara, Leodesh were randomly selected. Stage 5: the community health workers developed a list of households with women who have children of 2 years or less, 70 household in each of the villages were randomly selected. Out of the sampling frame and women in those households were invited to participate.
Study procedures: ethical clearance was obtained from the KCMU college Ethical committee before starting the research. The ethical clearance was delivered to District Medical Officer (DMO) of Babati rural, where permission to conduct the study was sought from the DMO office. DMO gave us introductory letter that was presented to Ward and Village leaders. At Magugu and Dareda, permission to cooperate with RCH team was given by the Medical officer in charge at Magugu Health center and Dareda Hospital, and delegated us to the RCH coordinator. The RCH coordinator fhmiliarized us to the RCH clinics and also delegated us to the village chairpersons and village health workers (CHWs). The CHWs developed a list of households with women who have children of 2 years or less, we did a lottery random sampling method selecting 70 household in each of the villages in both Dareda and Magugu wards. At the field starting point was identified at the village with assistance of village chairperson and data was collected from one house to another with aid of CHWs. Data collection started at 9 am in the morning to 6pm in the evening. Before interviewing, the participant was informed of the aims and objectives of the study and was asked for consent to participate in the study. Six undergraduate medical students in their 4th year collected the data after undergoing one day training on data collection. Pre-testing of the tool before the onset of the study was conducted in Moshi Municipal at Majengo Health centre. Five women who delivered in the last 12 months were interviewed to check for consistency, clarity and flow of the questions in the questionnaire.
Data collection tool and methods: a Swahili questionnaire was used to collect information from the participants. The questionnaire had closed and open-ended questions and consists of six sub-sections. The first part collected information on socio-demographic and socio-economic characteristics, second was reproductive and maternal health history, and third part collected information on ANC use, place of delivery and use of skilled birth attendant during the last pregnancy. The fourth section collected information on knowledge of danger signs during pregnancy, labor and childbirths and after delivery, and fifth on having birth preparedness and complication readiness plan for the last pregnancy. Post-natal care practice after delivery was the last section. The interviews were conducted at either participant´s home, or at health facility room depending on the preference of the participant. After finishing data collection verbal observation from the field was shared with the DMO, which will be followed by a full research report of the study after completion.
Data analysis: the data was entered and analyzed using SPSS 20. Before analysis, data was cleaned by running frequency of each variable. Categorical variables were summarized into frequency and percent while continuous variables were summarized using measure of central tendency and their respective measure of dispersion. Odds ratio with their 95% confidence interval were used to measure the strength of association between knowledge of danger signs and 4+ANC visits, having birth preparedness and complication readiness plan and SBA use during childbirth. Multivariable logistic regression analysis was conducted to control for confounders and get independent predictors for ANC 4+, having a BPCR plan and use of SBA. P-value of < 0.05 was considered statistically significant.
Categorization of variables: knowledge on ODS was measured by asking the study participant to mention spontaneously any danger sign she knows either by being told by the health care providers or by experience. If the study participant mentioned at least one key danger sign in each phase (during pregnancy, during delivery and after delivery) or could mention at least three danger signs in any phase (during pregnancy, delivery or immediate post-delivery) were considered to have good knowledge of obstetric DS. A participant who mentioned 1-2 DS was considered to have poor knowledge and the one who could not mention any DS was considered to lack knowledge on obstetric DS. Birth preparedness has 6 components, women were categorized as well prepared if they prepared 3 or more components and not well prepared if they prepared less than 3 components. SBA use during childbirth is reported if a woman reported to be delivered by skilled health providers while assistant with TBA or relatives at home was categorized as lack of SBA use.
Ethics approval and consent to participate: the study was given ethical clearance from Kilimanjaro Christian Medical University Ethical Committee (Certificate number UG 003). Permission to conduct the study was sought from the District Medical Officer of Babati Rural district. Purpose of the study, benefit, right to refuse participation or leaving the study was explained to each participant including illiterate participants where more time was used for explanation before the interviews. The study participants were informed that the data will be kept confidential and only numbers were used in the questionnaires and not personal identifiers. A signed consent was obtained from each participant. In the case of illiterate women, the right thumbprint was used as a signature, and the ethics committee approved the thumbprint forms obtained from the illiterate women (participants). Participants were informed that refusal to participate will not affect services received at health facilities. Partners (3) and parental (1) written consent was sought for 4 women who were < 18 years.
Response rate: a total of 422 women were approached and 372 agreed to participate in the study giving a participation rate of (88.1%). Reasons for refusal to participate were; being busy with other home activities, others were in a hurry to go to other places for their other activities (market/field) and some were not interested with giving out their information.
Socio demographic characteristics of the participants: of the 372 women who were analyzed, their mean (SD) age of was 28.5 (7.1) years. Majority (77.4%) were married, (74.5%) had primary education and more than half (69.1%) were unemployed. Majority of the women (77.5%) use less than one hour to walk to the nearest facility with RCH services. Other background characteristics are shown in Table 1.
Reproductive and maternal health characteristics of the participants: the median (IQR) number of children among 372 study participants was 2 (1-4) children. All participants attended ANC at least once during last pregnancy, whereby majority (68%) had first ANC visit after 12 weeks of gestation age and 65.3% attended more than 4 ANC visits. Majority of the women (85%) delivered their last baby at the health facility. Only 13.7% of participants had birth prepared and complication readiness plan (i.e. prepared 3 or more components of BPCR) (Table 2).
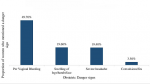
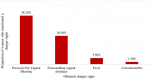
Knowledge of danger signs: a total of 73% of the women reported to be counseled about obstetric danger signs during ANC visits. However, 44%, 70% and 61% of the women could not mention any danger sign of obstetric emergency during pregnancy, childbirth and after delivery, respectively (Table 3). Overall, 32.0% of women had good knowledge on danger signs (were able to mention ≥3 danger signs of obstetric emergency (either during pregnancy, during delivery or after delivery)). The most known danger sign was vaginal bleeding during pregnancy (49.7%) and the least known danger sign is retained products of placenta during delivery (0.8%). Excessive bleeding (29.3%), and prolonged labour (4%) were the most common mentioned danger signs during childbirth. Most known danger signs immediately post-delivery were excessive vaginal bleeding (28.2%) and foul-smelling discharge (16.4%). Other known danger signs during pregnancy, during delivery and after deliver are shown in Figure 1, Figure 2, and Figure 3 respectively.
Effect of knowledge of danger signs on ANC visits, birth preparedness and SBA use during childbirth: of the 372 women, 65.3% attended ANC for 4 or more visits, 85 % were assisted by skilled health provider during childbirth and 13.7% of participants had birth prepared and complication readiness plan. In crude logistic regression analysis, overall knowledge of danger signs (knowledge of 3+ DS) was not significantly associated with odds of 4+ ANC visits and SBA use, Table 3. On the other hand, the odds of well-prepared BPCR was 2 times significantly higher among those who had overall knowledge of danger signs compared with their counterparts who did not have overall knowledge (OR=2.12; 95%CI= (1.16-3.85)). After controlling for other factors, overall knowledge on danger signs remained significantly associated with having birth preparedness and complication readiness plan, i.e. odds of well-prepared BPCR was 98% higher among those who had overall knowledge of danger signs compared with those who did not have overall knowledge (OR=1.98; 95%CI = (1.05-3.76)). This was not the case for 4+ ANC visits and SBA use. In adjusted analysis, number of pregnancies and gestational age at first ANC visit were independently associated with 4 or more ANC visits. Age of the participants was an important predictor of being well-prepared by having BPCR plan. Level of participants´ education, time to nearest health facility and partner participation during ANC visits were independently associated with SBA use during childbirth (Table 3).
The results of this study show there is universal ANC attendance at least once with 65% attending for 4 or more visits and 85.2 % of women were assisted by SBA during childbirth. Only a third (32%) of women had good knowledge of obstetric danger signs during pregnancy, childbirth and after delivery. Knowledge on danger signs was significantly and positively associated with 4 or more ANC visits and having a birth preparedness and complication readiness plan (BPCR), but not with SBA use. Use of health facilities during childbirth have increased in this setting from 48% shown by Tanzania and Demographic Health Survey (TDHS) of 2015/16 in Manyara region to 85% observed in this study, surpassing the national target of skilled birth attendants of 80% by 2020 [5,29]. Attendance for 4+ ANC visits has improved to 65.3%. SBA use have improved in Tanzania from 51% in 2010 TDHS to 64% in 2015/16. Improvement in ANC 4+ times and SBA use has also been noted in other East African countries i.e. Uganda, Kenya and Rwanda [30]. Key question to follow will be if this improvement in use of health facilities is matched by improvement in quality of services offered to improve morbidity and mortality outcomes.
In this study knowledge of danger signs among women was low (32%) despite that 73.1% of women reporting they were informed about danger signs during ANC visits. Knowledge of danger signs was slightly higher compared with the studies done in rural east Tanzania, rural south Tanzania and central Tanzania where 19%, 7.4%, 18.4% of women respectively knew 3 or more danger signs of obstetric emergency during pregnancy, delivery or after delivery [8,17,18], and higher than studies in Jordan (11.5%) and Uganda (15.2%) [9, 22]. The most spontaneously mentioned danger sign was vaginal bleeding in all phases (during pregnancy, during delivery and after delivery) (49.6%), this is similar to study done in rural Uganda (9.2%) [9]; the reason vaginal bleeding is mentioned in all phases as most commonly recognized as a danger sign may be that it is the most visible sign and the most common cause of maternal death during pregnancy and immediately after delivery hence stressed by providers during counseling sessions [3]. What was alarming was low knowledge retention among women, despite most of them being counseled during ANC visits. The way the counseling or education is done during ANC visits needs to be assessed and different model of imparting information/knowledge is needed to improve retention. Some studies have showed that changing the way health providers provide counseling to the women and move to small group discussions or use of mother to mother groups for discussions and participation of the women improved knowledge retention. Study done in Rwanda among women of reproductive age showed that focused group discussion during ANC visits increased pregnancy-related knowledge [31].
Overall knowledge of obstetric danger signs was not significantly associated with four or more ANC visits. Which was in line with the study done in rural Nigeria where there was no association between antenatal clinic visits and knowledge of obstetric danger signs [27], but differ with studies from Egypt and Ethiopia that showed an association between frequency of ANC attendance and knowledge on danger signs of obstetric emergency [24,32,33]. The cross section design makes it difficult to establish if frequency of ANC visits influence knowledge on danger signs or other way around. However, the need to improve counseling about danger signs during ANC visits in order to influence care seeking when complication arise cannot be over emphasized. Overall knowledge of danger signs was a significant predictor of having a well birth preparedness and complication readiness plan (BPCR) in this study. Studies in Tanzania and Uganda showed that women who were knowledgeable on danger signs during pregnancy were 4 times more likely to be knowledgeable on BPCR compared to those who were not knowledgeable [18,34]. Further, in Uganda [9] and in Ethiopia [35] showed that women who could mention two or more danger signs in any of the phases had 2-3 times higher odds to be prepared for birth and its complications compared to women who could not mention any danger signs. Having BPCR plan have been associated with SBA attendance use for neonatal and maternal complications [9,18,26-28]. This implies that efforts to improve fhmilies and community awareness on danger signs and BPCR are needed in Tanzania.
In this study knowledge of obstetric danger signs, was not associated with the use of SBA during childbirth. The results are contrary to studies done in Mtwara Tanzania, Nigeria, and Ethiopia, which showed that women with knowledge of obstetric danger signs had increased odds of SBA use [8,27,36,37]. SBA use was high in this setting (85%) and other factors apart from knowledge, i.e. secondary education and shorter distance to health facility predicted SBA use. In Babati rural 48.1% women reported to use less than 30 minutes to walk to the nearest health facility, this may have contributed to the use of SBA during delivery because of easy access to a health facility. The study had some limitations that need to be considered when interpreting the results. The study enrolled women who delivered within 24 months prior to the study hence some women may had difficulty remembering the danger signs, this may lead to underestimation proportion of women with good knowledge on danger signs. Also, the study mostly enrolled women who have a live child of 2 years or younger. We have missed women with negative outcomes like stillbirth, miscarriages thus under estimate the prevalence of use of maternal health services. But on the other hand this was a community-based study hence the information obtained from this study reflect the reality in the level of knowledge on danger signs in the rural Tanzanian communities.
The study observed that, majority of women attended antenatal care and were counseled on danger signs, however women had low knowledge of obstetrics danger signs. Good knowledge of danger signs during pregnancy increased the odds of 4 or more ANC visits and being prepared for birth and its complications. We recommend that there is a need to assess how counseling is given to women during antenatal and postnatal care given low level of knowledge on danger signs despite universal attendance for ANC once and a third attending for four or more times. Alternative approaches of teaching women during ANC should be explored by providers. One of such methods maybe peer to peer counseling or group discussions where women would get an opportunity to ask questions and give their thoughts which will ensure their active participation unlike the model of just direct teaching currently used. Other ways of addressing the educating and information sharing with women can be through use of e-health or SMS messages as more than 80% of Tanzanians have mobile phones [5].
What is known about this topic
- Knowledge of danger signs among women is shown to be higher in urban setting (57.8%). Compared to rural settings (7.4%);
- Studies done in Tanzania have linked knowledge of obstetric danger signs with socio-demographic and economic factors but poorly linked it with utilization of health services like use of skilled birth attendants, and antenatal care for better maternal outcomes.
What this study adds
- There is good antenatal coverage in the study area (rural area) and majority of women are counseled on danger signs of obstetric emergencies however there is still low knowledge on danger signs of obstetric emergencies hence new ways suggested on counselling women since majority of them have achieved only formal education (primary level);
- Women who were knowledgeable on danger signs of obstetric emergencies during pregnancy had higher odds of attending antenatal care clinic and being prepared for birth and its complications.
The authors declare no competing interests.
EJS, MGM, FHM, BJL and SEM contributed to the design of the study. EJS, MGM and FHM collected the data. EJS, MGM, FHM, EJD and SEM analyzed the data. EJS, MGM, FHM, EJD and SEM interpreted the results. EJS, MGM, FHM prepared the manuscript and all the other authors reviewed the manuscript critical input before submission. All authors read and approved the final manuscript.
We would like to give our sincere thanks to women who participated in the study. We also thank the district health management team for permission to conduct the study in the district. We also give our thanks to the District Medical Officer of Babati Rural, Dr Madama B. Hossea for his contribution on details and information about his district as well as community health workers and ward leaders who helped during house to house interviews.
Table 1: background characteristics of the study participants in Babati rural district (N=372)
Table 2: reproductive and maternal health characteristics of the study participants in Babati rural district (N=372)
Table 3: logic regression for the effect of knowledge of danger signs on 4+ ANC visits, well-prepared BPCR and SBA use during delivery among women in Babati rural district (N=372)
Figure 1: danger signs mentioned by women during pregnancy in Babati rural district (N=372)
Figure 2: danger signs mentioned by women during childbirth in Babati rural district (N=372)
Figure 3: danger signs mentioned by women after delivery in Babati rural district (N=372)
- Alkema L, Chou D, Hogan D, Zhang S, Moller AB, Gemmil A et al. Global, regional, and national levels and trends in maternal mortality between 1990 and 2015, with scenario-based projections to 2030: a systematic analysis by the UN Maternal Mortality Estimation Inter-Agency Group. Lancet. 2016 Jan 30;387(10017):462-74. PubMed | Google Scholar
- WHO. Maternal mortality fact sheet. Health topics, maternal and child health. World Health Organization; 2018. Accessed Feb 15 2019.
- WHO, UNICEF, World Bank, UNFPA, United Nations Population Division. Trends in maternal mortality: 1990 to 2015. World Health Organization; 2015. Accessed Feb 16 2019.
- NBS, ICF Macro. Tanzania Demographic and Health Survey 2010. National Bureau of Statistics and ICF Macro, Dar es Salaam, Tanzania, 2011.
- TDHS. Tanzania demographic and health survey and malaria Indicator Survey 2015-2016. National Bureau of Statistics, Dar es Salaam, Tanzania and Rockville, Maryland, USA: MoHCDGEC, MoH, NBS, OCGS, and ICF; 2015-2016.
- WHO UNFPA, UNICEF, AMDD. Monitoring emergency obstetric care a handbook. Geneva, Switzerland: World Health Organization; 2009. Accessed Feb 25 2019.
- Say L, Chuo D, Gemmill A, Tuncalp O, Moller AB, Daniels J et al. Global causes of maternal death: WHO systematic analysis. Lancet Global Health. 2014;2(6):e323-333. PubMed | Google Scholar
- Mpembeni R, Killewo J, Leshabari M, Massawe S, Jahn A, Mushi D et al. Use pattern of maternal health services and determinants of skilled care during delivery in Southern Tanzania: implications for achievement of MDG-5 targets. BMC Pregnancy and Childbirth. 2007 Dec 6;7:29. PubMed | Google Scholar
- Kabakyenga K, Ostergren P, Turyakira E, Pettersson K. Knowledge of obstetric danger signs and birth preparedness practices among women in rural Uganda. Reproductive Health Journal. 2011;8:33. PubMed | Google Scholar
- Ameh C, Msuya S, Hofman J, Raven J, Mathai M, van den Broek N. Status of emergency obstetric care in six developing countries five years before the MDG targets for maternal and newborn health. PLoS One. 2012;7(12): e49938. PubMed | Google Scholar
- Thaddeus S, Maine D. Too far to walk: maternal mortality in context. Journal Social Science Med.1994;38(8):1091-1110. PubMed | Google Scholar
- Mbizvo M, Say L. Global progress and potentially effective policy responses to reduce maternal mortality. International Journal of Gynecology and Obstetrics. 2012 Oct;119 Suppl 1:S9-12. PubMed | Google Scholar
- Gabrysch S, Campbell OMR. Still too far to walk: literature review of the determinant of delivery service use. Journal BMC Pregnancy and Child Birth. 2009;9:34. PubMed | Google Scholar
- WHO. Managing complications in pregnancy and childbirth: a guide for midwives and doctors. Geneva, Switzerland: World Health Organization; 2003. Accessed Mar 12 2019.
- WHO. Recommendations on antenatal care for a positive pregnancy experience. World Health Organization; 2016. Accessed Mar 15 2019.
- JHPIEGO. Monitoring birth preparedness and complication readiness: tools and indicators for maternal and newborn health programs. Baltimore, Maryland: John Hopkins Program for International Education in Gynecology and Obstetrics; 2004.
- Pembe A, Urassa D, Carlstedt A, Lindmark G, Nystrom L, Darj E. Rural Tanzanian women´s awareness of danger signs of obstetric complications. BMC Pregnancy and Childbirth. 2009;9:12. PubMed | Google Scholar
- Urassa D, Pembe A, Mganga F. Birth preparedness and complication readiness among women in Mpwapwa district, Tanzania. Tanzania Journal of Health Research. 2012;14(1):1-7. PubMed | Google Scholar
- Bintabara D, Mpembeni RNM, Mohamed AA. Knowledge of obstetric danger signs among recently-delivered women in Chamwino district, Tanzania: a cross-sectional study. BMC. 2017;17(1):276. PubMed | Google Scholar
- Mwilike B, Nalwadda G, Kagawa M, Malima K, Mselle L, Horiuchi S. Knowledge of danger signs during pregnancy and subsequent healthcare seeking actions among women in Urban Tanzania. BMC Pregnancy and Childbirth. 2018;18(1):4. PubMed | Google Scholar
- Hoque M, Hoque M. Knowledge of danger signs for major obstetric complications among pregnant KwaZulu-Natal women implications for health education. Asia-Pacific J Publ Health. 2011;23(6):946-56. PubMed | Google Scholar
- Okour A, Alkhateeb M, Amarin Z. Awareness of danger signs and symptoms of pregnancy complication among women in Jordan. International Journal of Gynecology and Obstetrics. 2012;118(1):11-4. PubMed | Google Scholar
- Duysburgh E, Ye M, Williams A, Sie A, Massawe S, Williams J et al. Counselling on and women´s awareness of pregnancy danger signs in selected rural health facilities in Burkina Faso, Ghana and Tanzania. Tropical Medicine and International Health. 2013;18(12):1498-1509. PubMed | Google Scholar
- Maseresha N, Woldemichael K, Dube L. Knowledge of obstetric danger signs and associated factors among pregnant women in Erer district, Somali region, Ethiopia. BMC Women´s Health. 2016;16:30. PubMed | Google Scholar
- Geleto A, Chonjenta C, Musa A, Loxton D. Women´s knowledge of obstetric danger signs in Ethiopia (WOMEN´s KODE): a systematic review and meta-analysis. Systematic Reviews. 2019 Feb 25;8(1):63. PubMed| Google Scholar
- Jammeh A, Sundby J and Vangen S. Barriers to emergrncy obstetric care services in perinatal deaths in rural Gambia: a qualitative in-depth interview study. ISRN Obstetric and Gynecology. 2011;01(03):94-103. PubMed | Google Scholar
- Doctor H, Findley S, Cometto G, Afenyadu G. Awareness of critical danger signs of pregnancy and delivery preparations for delivery and utilizations of skilled birth attendants in Nigeria. Journal of Health Care for the Poor and Underserved. 2013;24(1):152-170. PubMed | Google Scholar
- Solomon A, Amanta N, Chirkose E, Badi M. Knowledge about danger signs of pregnancy and associated factors among pregnant women in Debra Birhan Town, Central Ethiopia. Science Journal of Public Health. 2015;3(2)269.
- MOHSW. The national road map strategic plan to accelerate reduction of maternal, newborn and child deaths in Tanzania 2008-2015. Dar es Salaam, Tanzania: Ministry of Health and Social Welfare; 2014. One Plan, RCHS, Directorate of Preventive Services. 2014.
- Ruktanonchai CW, Nilsen K, Alegana VA, Bosco C, Kajeguka ACS, Matthews Z et al. Temporal trends in spatial inequalities of maternal and newborn health services among four east African countries, 1999-2015. BMC Public Health. 2018;18(1):1339. PubMed | Google Scholar
- Musabyimana A, Lundeen T, Butrick E, Sayinzoga F, Rwabufigiri BN, Walker D et al. Before and after implantation of group antenatal care in Rwanda: a qualitative study of women´s experiences. Reproductive Health Journal. 2019;16(1):90. PubMed | Google Scholar
- Rashad W, Essa R. Women´s awareness of danger signs of obstetrics complications. Journal of American Science. 2010;6(10)1299-1306. Google Scholar
- Amenu G, Mulaw Z, Seyoum T, Bayu H. Knowledge about danger signs of obstetric complications and associated factors among post-natal mothers of Mechekel District health centers East Gojjam Zone, Northwest Ethiopia. Scientifica. 2016;1-7. Google Scholar
- Mbalinda S, Nakimuli A, Kakaire O, Osinde M, Kakande N , Kaye D. Does knowledge of danger signs of pregnancy predict birth preparedness? A critique of the evidence from women admitted with pregnancy complications. Health Research Policy and Systems. 2014;12:60. PubMed | Google Scholar
- Debelew G, Afework M, Yalew A. Factors affecting birth preparedness and complication readiness in Jimma Zone, Southwest Ethiopia: a multilevel analysis. Pan African Medical Journal. 2014;19:272. PubMed | Google Scholar
- Tadese F, Ali A. Determinants of use of skilled birth attendance among mothers who gave birth in the past 12 months in Raya Almata District, North East Ethiopia. Clinics Mother Child Health. 2014;11:2.
- Tura G, Afework M, Yalew A. The effect of birth preparedness and complication readiness on skilled care use: a prospective follow-up study in Southwest Ethiopia. Reproductive Health. 2014;11:60. PubMed | Google Scholar