Reducing COVID-19 mortality in Senegal through community case management
Sylla Thiam, Masserigne Soumaré, Jane Carter
Corresponding author: Sylla Thiam, Sunu Sante Consulting, Hann Bel Air, Dakar, Sénégal 
Received: 08 Mar 2021 - Accepted: 13 Apr 2021 - Published: 15 Apr 2021
Domain: Community health,Global health,Public health
Keywords: COVID-19, deaths, community case management, health workforce
©Sylla Thiam et al. PAMJ-One Health (ISSN: 2707-2800). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Sylla Thiam et al. Reducing COVID-19 mortality in Senegal through community case management. PAMJ-One Health. 2021;4:13. [doi: 10.11604/pamj-oh.2021.4.13.28763]
Available online at: https://www.one-health.panafrican-med-journal.com/content/article/4/13/full
Reducing COVID-19 mortality in Senegal through community case management
&Corresponding author
Like many countries across the world, Senegal is facing a second wave of the COVID-19 pandemic with an increase in hospital admissions and deaths, putting pressure on an already overstretched health workforce. This situation requires new and innovative measures to reverse the trend and avoid overwhelming the health system. Community Case Management is a proven strategy in healthcare that could be a powerful tool in preventing severe cases and reducing deaths related to COVID-19. This proposed strategy is based on early detection of cases and home-based management by community health workers.
Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) was first identified in Senegal on 2 March, 2020, and has now spread widely across the country. Currently, Senegal is experiencing a surge in coronavirus disease 2019 (COVID-19) with case numbers increasing daily [1], putting pressure on health services already overwhelmed by routine services [2]. From February 1-28, 2021, the number of daily admissions into intensive care units (ICU) across the country ranged from 49 to 63 patients, with an average of eight deaths daily. During this period, 242 deaths were reported by the Ministry of Health and Social Action [1,3]. Compared to 411 deaths from March to December, 2020, 460 deaths were reported from January 1 to February 28, 2021, representing 52.8% of all reported COVID-19 deaths (460/871) [1]. The number of COVID-19 related deaths occurring at home is unknown in the absence of diagnostic or post-mortem confirmation. In addition to rising numbers of infections, mortality data suggest diagnostic delay and late management of cases in overwhelmed health facilities. Innovative approaches are urgently needed to reverse this trend. As everywhere in the world, COVID-19 vaccines are a source of hope in Senegal; however, vaccination will be an additional tool that will not preclude the use of barrier measures in the immediate and medium term. Vaccination should help reduce the incidence of severe infections and hospital admissions and its impact will be evident over time; the threat of variants will also need to be considered [4-6]. Therefore, in resource-limited settings, greater focus should be placed on community-level actions.
Community case management (CCM) is a proven strategy that reduces mortality from endemic diseases such as malaria and should be the strategy of choice to reduce severe disease and deaths, and help raise awareness in communities [7,8]. The CCM strategy is based on prompt and effective case management by trained community health workers supported by health professionals, and is the backbone of the Senegalese health system. CCM relieves pressure on health facilities and should drastically reduce the requirement for ICU services by COVID-19> patients [9]. Data on home-based management in the context of COVID-19 is scarce. The limited experiences reported make use of qualified health professionals thereby putting even more pressure on overstretched healthcare workers [9,10]. CCM aims to mobilise communities´ potential to prevent deaths linked to COVID-19. Trained community health workers would be equipped with four essential tools: (i) a thermoflash for temperature reading, (ii) a pulse oximeter to determine blood oxygen saturation (an important indicator of disease severity; (iii) treatment kits; and (iv) a mobile phone.
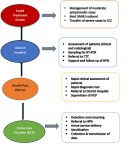
Implementation would be organised at health district level and structured around the Health Post Nurse (HPN) who is in charge of a group of community health workers called Home Care Providers (HCP). HCPs, recruited from their places of residence, serve their own communities. Each HCP is responsible for an area (square of houses, sub-neighbourhood, neighbourhood and village) and would make regular visits to all households twice a week. In each home, people with fever would be assessed using a simplified algorithm based on five symptoms suggestive of COVID-19 disease to classify patients into suspected or non-suspected cases. Suspected cases would be referred to the health post for rapid antigen testing performed by the HPN. Patients with positive test results would be referred to the district hospital for a complete clinical and radiological evaluation, as required. Patients meeting the criteria for home management would be managed at home and followed up by the HCP (Figure 1).
The focus of community monitoring would be detecting danger signs and measuring blood oxygen saturation, with attention to the elderly and those with co-morbidities. In cases of severity or underlying co-morbidities, patients would be referred to the nearest Covid Treatment Centre (CTC). Family members would be educated and also involved in patient follow-up and support. The link between the patient, the HCP, the HPN and the district hospital would be maintained through telephone communication, which will also be used for collecting and transmitting real-time data. This information would enrich the existing national surveillance system through providing real-time community data. Preventive measures and safeguards would be strictly observed at every step. HCPs will be equipped to promote barrier measures within the community during their home visits. This simple, low-cost, long-proven approach based on the primary level of the Senegalese healthcare system would lay the groundwork for routine integration of COVID-19 management into the health system and strengthen the community component that is still under-utilised in current strategies. This strategy could also be applied to other countries with community-based healthcare programmes in place.
The authors declare no competing interests.
All the authors have read and agreed to the final manuscript.
Figure 1: organisation of the COVID-19 community case management strategy and responsibilities across the continuum of care
- Ministère de la Sante et de l´Action Sociale. Riposte à l´épidémie du nouveau Coronavirus, Sénégal: Rapport de Situation n°84 du 1er Mars 2021.
- Elisabeth Paul, Youssoupha Ndiaye, Farba L Sall, Fabienne Fecher, Denis Porignon. An assessment of the core capacities of the Senegalese health system to deliver Universal Health Coverage. Health Policy Open. 2020 Dec; 1:100012. PubMed | Google Scholar
- Ministère de la Sante et de l´Action Sociale du Sénégal. Coronavirus, informations officielles et quotidiennes. 2021.
- Vladislav Izda, Matlock A Jeffries, Amr H Sawalha. COVID-19: a review of therapeutic strategies and vaccine candidates. Clin Immunol. 2021; 222 (2021):108634. PubMed | Google Scholar
- Guido Forni, Alberto Mantovani. COVID-19 vaccines: where we stand and challenges ahead. Cell Death Differ. 2021;28(2):626-639. PubMed | Google Scholar
- Wagner G Dos Santos. Impact of virus genetic variability and host immunity for the success of COVID-19 vaccines. Biomed Pharmacother. 2021; 136:111272. PubMed | Google Scholar
- Sylla Thiam, Julie Thwing, Ibrahima Diallo, Fatou B Fall, Mame B Diouf, Robert Perry et al. Scale-up of home-based management of malaria based on rapid diagnostic tests and artemisinin-based combination therapy in a resource-poor country: results in Senegal. Malar J. 2012;11:334. PubMed | Google Scholar
- Kumanan Rasanathan, Maria Muniz, Salina Baksi, Meghan Kuma et al. Community case management of childhood illness in sub-Saharan Africa - findings from a cross-sectional survey on policy and implementation. J Glob Health. 2014;4(2):020401. PubMed | Google Scholar
- Janice John, Lora Council, Leah Zallman, Jessamyn Blau. Developing an intensive community COVID-19 management strategy: helping our patients access patient-centered care across a continuum of COVID-19 disease needs. NEJM catalyst innovations in care Delivery, May 2020. Google Scholar
- Bob Mash. Primary care management of the coronavirus (COVID-19). S Afr Fam Pract. 2020; 62(1):5115. Google Scholar