Determinants of Delivery Site's Preferences Among Women in East Africa: Case Study In Ishaka Municipality, Western Uganda
Jean Kakule Muhongya, Bives Mutume Vivalya, Patrick Kambale Saasita, Ssemakula Edward
Corresponding author: Jean Kakule Muhongya, Allied Health Department, Kampala International University, Western Campus, Po Box 71 Bushenyi, Uganda 
Received: 13 Jun 2020 - Accepted: 18 Nov 2020 - Published: 20 Nov 2020
Domain: Community health,Health promotion,Maternal and child health
Keywords: Determinants, delivery sites, traditional birth attendance, Ishaka Municipality, Uganda
©Jean Kakule Muhongya et al. PAMJ-One Health (ISSN: 2707-2800). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Jean Kakule Muhongya et al. Determinants of Delivery Site's Preferences Among Women in East Africa: Case Study In Ishaka Municipality, Western Uganda. PAMJ-One Health. 2020;3:12. [doi: 10.11604/pamj-oh.2020.3.12.24295]
Available online at: https://www.one-health.panafrican-med-journal.com/content/article/3/12/full
Research 
Determinants of Delivery Site's Preferences Among Women in East Africa: Case Study In Ishaka Municipality, Western Uganda
Determinants of Delivery Site's Preferences Among Women in East Africa: Case Study In Ishaka Municipality, Western Uganda
Jean Kakule Muhongya1,2,&, Bives Mutume Vivalya3,4, Patrick Kambale Saasita5, Ssemakula Edward2
&Corresponding author
Introduction: It has acknowledged that delivered at traditional birth attendance can increase mortality death. Epidemiological studies have identified poor quality of care as being at greater risk of increasing the home delivery. This study aimed to explore pregnant women's factors associated with the site of delivery.
Methods: a community based cross-sectional study was conducted in Ishaka municipality using an established questionnaire based on real lifetime realities seen in maternal health facilities, The measure of association was odds ratios and 5% level of statistical significance, and the 95% confidence intervals was measured for all the above analyze.
Results: ratio between delivery in health facility and delivery at home was 4.5/1. The factors associated with the women's choice of delivery were the available health center, the level of education attained, the affordable friendly services, and the behavior of the health workers (p<0.05). The result revealed that having unpaid health fees and hospitality of health were predictors for choosing antenatal healthcare facility.
Conclusion: quality of antenatal health care associated to social work attitude of health practitioners determined the choice of site´s delivery. This study confirms that in rural settings, promoting of funded maternal healthcare is a core of delivery´s site preference.
Delivery´s site preference is major determinant of pregnancy outcomes. Its many consequences are usually harmful for the family [1]. Maternal death, one of complications of childbirth, has risen three fourth times than the expected by 2015 [1, 2]. The World Health Organization (WHO) estimated that about 536,000 women died during delivery procedure, mostly from pregnancy and delivery preventable complications [3]. Evidences illustrated that more than 50% of maternal death occurred in health facilities or at home; either monitored by traditional birth attendant or poor trained health workers [3,4]. To date, WHO policies and countries have implemented strategies to prevent the maternal and newborn death including the access to qualified health workers, the prevention and management of postpartum hemorrhage, promotion of family planning, the antenatal care and child protective services [5-7]. However, few studies found that quality of care is commonly impaired in developing countries. These concerned studies suggested the poor access to health facilities and the low socioeconomic status were the main cause of maternal mortality [6-7]. In sub-Saharan countries, studies showed that nearly 78% of pregnant women lacked basic input needed by midwives during childbirth. Additionally, the lack of trained attendance contributed to poor maternal and infantile outcomes during delivery [5,8]; significant proportion of mothers still delivers at home with or without health workers [9]. However, studies showed that childbirth complications were common in rural settings, and in low-income health facilities [1-3]. Few studies illustrated the relationship between the preference of site of childbirth site and the maternal and newborn outcomes [10-12]. Promoting delivery in health facilities has shown positive outcomes in reducing reduce maternal mortality in many low-income countries like Ethiopia and Uganda [13]. Additionally, protected delivery practices and antenatal health care are among the most effective health interventions for preventing maternal morbidity; and mortality and for identifying threats to the mother and unborn baby´s health status, as well as for counseling on birth preparedness, delivery care and family planning options after the birth [14,15]. Despite the antenatal health care, the deliveries at TBA and at home remains reported with delivery complications [16]. The choice of home or TBA deliveries compared to health facility deliveries is due to unknown factors. Moreover, there is no tangible study conducted to investigate the determinants of site of child delivery [17]. This study aimed to explore the factors associated with the choice of childbirth sites in Ishaka municipality.
Participants: to carry out this cross-sectional survey, conducted in Ishaka municipality in Bushenyi district, in Uganda; 358 women were interviewed from 01 February to 30 June 2017 in all health facilities with maternity health care services (180) and the community (178 participants). We included all women, aged between 15 and 49 years, who had experienced in pregnancy and delivery found in health facilities and towns (Ishaka, Bushenyi, Kizinda) in Ishaka municipality. This study excluded all women who have been pregnant, who had an active mental or physical illness; or those who did not consent to participate to the current study. The sample size for the study was determined using the sample estimation Kish and Leslie´s formula below [18].
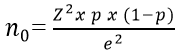
Where: no = sample size p = number deliveries in health facilities = 37% = 0.37 q = number delivered out of established facilities = 63% = 0.63 e = standard error = 5% =0.05 Z&/2= Z value of 95% confidence = 1.96 from the Z-table Substituting the values into the formula: no = 0.37 x 0.63 x (1.96)^2/0.0025 = 358
Procedures: multistage stratified sampling technique with probabilities proportional to size was performed to select the study subjects. Women were simple randomly selected while health workers and other key informants were selected on purpose. Two trained research assistants supervised by the first author collected data of all women with the inclusion criteria for this study using an established questionnaire translated in Runyakore, which included the independent variables which included clinical factors such as age of respondents, size of family, level of education attained; and the dependent variables including home delivered, Traditional Birth Attendants (TBA), neighbourhood clinic, characteristics. The intervening factors were made up by staff absenteeism, staff attitude and distance to the health facility. Voluntary recruitment of study participants was performed during this survey. Informed consent was obtained after fully explaining the details of the study in English and translated in local language. The study received approval from the Academic Board of Bishop Stuart University. An informed consent document from the Research Ethics committee of Bishop Stuart University was signed by the investigator, every participants and witness.
Statistical analysis: the collected data were entered into STATA 13 software. Descriptive and Inferential statistics were used to interpret the study findings. Bivariate logistic regression was carried out. The variables were significant when p-value ? 0.05. The measure of association was correlated to odds ratio.
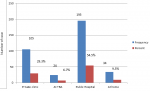
A total of 358 women contributed to the analysis (Table 1). The results show that the mean age was 26. 234 women (65.4%) were married, 74 women (20.7%) single, 45 women (12.6%) separated, and 5 women (1.3%) widowed. 336 women (93.9%) reported to achieve secondary school and 22 (6.1%) attained primary school. 213 women (59.5%) reported to be unemployed. Figure 1 showed that 195 women (54.5%) reported to deliver at public hospital, 105 (29.3%) delivered in private health clinic, 24 (6.7%) reported that the childbirth were conducted at traditional birth attendances, and 34 (9.5%) reported to deliver at home. At baseline, Table 2 shows that 343 women (95.8%) reported to attend antenatal health care clinics during previous pregnancy. Of these, 202 (56.4%) attended public health facilities, 77 (21.5%) went to private health clinics, 50 (14%) reported to attend both private and public; and 14 women (3.9%) reported to attend TBA homes. Also 225 women (62.8%) reported to attend four times the antenatal health care services. The logistic regression analysis shows that 358 had completed data. Concerning the factors associated with the choice of delivery site, the distance between women´s location and health facility, the affordable friendly services, the level of education attained, the access to trained health workers were the predictors of the choice of delivery sites (p<0.05). Additionally, women reported that choosing the site of antenatal health care was guided by the available unpaid health cost. Among the means of reducing maternal death reported by the participants are having available drugs and supplies in the health facilities, having many trained friendly heath workers, providing free mama kit societal behavior changes; promoting maternal health care education, and strengthening the health system.
The aim of the current study was to investigate the factors that influenced the choice of place of delivery among pregnant women in Ishaka municipality. The findings of this study revealed that women delivered at health facilities 4.5 more than they delivered at home. Also, the results shows that the site of childbirth is directed by the available and the affordability of health care services, the level of education attained; the presence of trained midwives and doctors, and the behavior of the health workers. The results showed that 93.9% of participants attained secondary school level. This is consistent with the findings of Lau et al. [19] who showed a high level of education among delivered women. The explanation could be the fact that Ishaka municipality is an environment with available schools and university. Majority of participants were peasants. This is similar to the findings of many studies, given that the economic activities of the interviewed women were analyzed according to the major broad economic activities namely; peasant farming, business and formal employment implying salaried job [20-22]. This results revealed that 82.1% of participants delivered at health facilities This is in contrast with the results of Ababulgu et al. who showed 61.9% of the studied population gave birth at home [20]. Ababulgu studied the delivery site preference among child-bearing women.
Four point one percent of participants did not attend antenatal health care visits. This is in contrast with the result of Ewunetie et al. [21] who found a high prevalence of unintended antenatal visits. The low socioeconomic statues and the long distance to attend health facilities could explain this difference. The results revealed that attending antenatal clinic at a site contributed to the choice of delivery site. This is in contrast with the findings of Lau et al. who suggested a high quality of care to attracted patients and pregnant women [23]. The delivery preferable sites were selected according to its availability to offer free healthcare services, distance in kilometers and hours taken, presence of trained health workers and hospitality of the health workers at the facility. This is in concordance with the findings of Ababulgu et al. Deliveries by the private health providers are considered to be conducted by poor skilled attendants [19]. The means reported by the participants to prevent the mortality death were the available drugs and supplies in the health facilities; need of more trained friendly heath workers, providing free mama kit, societal behavior changes, promoting maternal health care education; and strengthening the health system. This is consistent with the findings of many studies [16,18]. Evidenced showed that the availability of trained health workers is an s important factor of quality of care [1]. The strengthening of this study is its importance to make available community-based view of maternal health services in Uganda rural settings. This basic information ought to prevent maternal and perinatal deaths due poor antenatal and prenatal health care. The limitation to the study is due to its cross-sectional model which is not important to assess the effect-cause relationship.
This study has shown that delivery´s choice of site is mainly determined by the access to equipped health facilities with trained workers, socioeconomic status, and the level of education attained. Personal difficulties and relevant attitudes lead to prefer delivery site, either at home or at health facilities. Further studies should be carrying out to evaluate the associated between the behavior of midwives and doctors; and the choice of delivery site. Efforts involved in improving of the knowledge of the prevention maternal and newborn deaths should give a true picture of service delivery and strengthen the public-private partnership. Additionally, the reference system services are mostly required to the earliest access to the health facilities.
What is known about this topic
- Maternal mortality is public health problem in Uganda due to childbirth carried out by non trained health practitioners;
- The deliveries at TBA and at home remains reported with delivery complications Hospitals or health facilities still having issues of equipment and lack of trained health workers;
- Antenatal care services associated with poor access to health facility lead the choice of delivery site for a pregnant woman.
What this study adds
- The funding of childbirth fees, the hospitality of trained health workers and the available antenatal care are predictors of choice of delivery site;
- The lack of reference system in rural health settings increases the childbirth at Traditional birth Attendants maternity;
- Reduction of maternal death sets up close implementation of maternal and children care by the government and its partners. Thus, this article represents an alarm to the government and health workers to made priority "safe mother".
The authors declare no competing interests
Kakule Muhongya Jean designed the study, collected, and analyzed the data and draft. Ssemakula Edward and Bives Mutume Vivalya analyzed the data and draft the manuscript. Patrick Kambale Saasita, and Ssemakula Edward were involved on intellectual review of the manuscript. All authors read and approved the final manuscript.
I am grateful to God for having enabled me to live. I extend my appreciation to my family for the continuous encouragements. I acknowledge Ass. Prof. Kazibwe Francis my supervisor and Prof. Edward Ssemakula the joint supervisor at Bishop Stuart University for all the invaluable moral support and academic guidance acknowledge the research assistants who helped me in collecting data with dedication. I thank the women who participated in the study are thanked tremendously.
Table 1: socio-demographic characteristics
Table 2: determinants of delivery site
Figure 1: sites of delivery
- Chukuezi C. Socio-cultural factors associated with maternal mortality in Nigeria. Research journal of social sciences. 2010;1(5):22-6. Google Scholar
- Buse K, Hawkes S. Health in the sustainable development goals: ready for a paradigm shift?. Globalization and health. 2015 Dec;11:13. PubMed | Google Scholar
- Shah IH, Say L. Maternal mortality and maternity care from 1990 to 2005: uneven but important gains. Reproductive Health Matters. 2007 Jan 1;15(30):17-27. PubMed | Google Scholar
- Ahmed S, Li Q, Liu L, Tsui AO. Maternal deaths averted by contraceptive use: an analysis of 172 countries. The Lancet. 2012 Jul 14;380(9837):111-25. PubMed | Google Scholar
- Gabrysch. Still too far to walk: literature review of the determinants of delivery service use. BMC Pregnancy Childbirth. 2009;9:34-10. PubMed | Google Scholar
- Kassebaum NJ, Bertozzi-Villa A, Coggeshall MS, Shackelford KA, Steiner C, Heuton KR et al. Global, regional, and national levels and causes of maternal mortality during 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. The Lancet. 2014 Sep 13;384(9947):980-1004. PubMed | Google Scholar
- Tann CJ, Kizza M, Morison L, Mabey D, Muwanga M, Grosskurth H et al. Use of antenatal services and delivery care in Entebbe, Uganda: a community survey. BMC pregnancy and childbirth. 2007 Oct 11;7:23. PubMed | Google Scholar
- United Nations Children's Fund (UNICEF). The state of the world's children 2009: maternal and newborn health. Unicef. 2008. PubMed | Google Scholar
- Benton L, Newell ML. Childbearing and the impact of HIV: the South African experience. infertility rates and population decline. Palgrave Macmillan, London. 2013;166-184. Google Scholar
- Gorrette N, Nabukera S, Salihu HM. The abortion paradox in Uganda: fertility regulator or cause of maternal mortality. Journal of obstetrics and gynaecology. 2005 Jan 1;25(8):776-80. Google Scholar
- Lawn JE, Blencowe H, Kinney MV, Bianchi F, Graham WJ. Evidence to inform the future for maternal and newborn health. Best practice & research Clinical obstetrics &gynaecology. 2016 Oct 1;36:169-83. PubMed | Google Scholar
- Fotso. Maternal health in resource-poor urban settings: how does women's autonomy influence the utilization of obstetric care services. Reproductive Health. 2009;6:9-10. PubMed | Google Scholar
- Mulusew. Preference and factors affecting mothers as to the site of delivery in Shebe town, south-western Ethiopia. Jimma University, in press. 2013.
- Bekuma TT, Firrisa B, Girmaye M, Bikila H, Kejela G. Factors Affecting choice of childbirth place among childbearing age women in Western Ethiopia: a community-based cross-sectional study. Int J Reprod Med. 2020 Apr 25;2020:4371513. PubMed | Google Scholar
- Bushenyi district Local Government. 2002 Population and housing census analytical report. Mukono. 2007.
- Singh A, Masuku M. Sampling Techniques & Determination of Sample Size in Applied Statistics Research: an Overview. IjecmCoUk. 2014;II(11):1-22.
- Oliveros. Secondary analysis of a national health survey on factors influencing women in the Philippines to deliver at home and unattended by a healthcare professional. Int J Gynecol Obstet. 2010;111(2):157-160. PubMed | Google Scholar
- Kish, Leslie. Survey Sampling. New York: John Wiley and Sons, Inc. 1965.
- Lau Y, Yin L. Maternal, obstetric variables, perceived stress and health-related quality of life among pregnant women in Macao, China. Midwifery. 2011 Oct 1;27(5):668-73. PubMed | Google Scholar
- Ababulgu FA, Bekuma TT. Delivery site preferences and associated factors among married women of child bearing age in Bench Maji Zone, Ethiopia. Ethiopian journal of health sciences. 2016;26(1):45-54. PubMed | Google Scholar
- Ouédraogo S, Koura GK, Accrombessi MM, Bodeau-Livinec F, Massougbodji A, Cot M. Maternal anemia at first antenatal visit: prevalence and risk factors in a malaria-endemic area in Benin. The American journal of tropical medicine and hygiene. 2012 Sep 5;87(3):418-24. PubMed | Google Scholar
- Jean-Bosco KM, Vivalya MN, Martial MV, Nzanzu K, Adelard KM, Juvenal PS et al. Transfusions reactions at Katwa and Kitatumba General Hospitals, in the eastern part of Democratic Republic of Congo. The Journal of Medical Research. 2020;6(3):83-6. Google Scholar
- Ewunetie AA, Munea AM, Meselu BT, Simeneh MM, Meteku BT. DELAY on first antenatal care visit and its associated factors among pregnant women in public health facilities of Debre Markos town, North West Ethiopia. BMC pregnancy and childbirth. 2018 Dec;18(1):173. PubMed | Google Scholar