Factors associated with knowledge, attitude and practice towards hepatitis B infection among pregnant women attending antenatal clinic in the Kumasi Metropolis, Ghana: a multi-centre hospital-based cross-sectional study
Ivy Nsiah, Charlotte Boachie Danquah, Enoch Odame-Anto, Christian Obirikorang, William Kwame Boakye Ansah Owiredu, Emmanuel Acheampong, Yaa Obirikorang, Evans Asamoah Adu, Sampson Donkor, Agartha Odame-Anto
Corresponding author: Sampson Donkor, Department of Molecular Medicine, Kwame Nkrumah University of Science and Technology, Kumasi, Ghana 
Received: 01 Jul 2020 - Accepted: 07 Aug 2020 - Published: 25 Aug 2020
Domain: Infectious disease,Chronic disease prevention,Maternal and child health
Keywords: Pregnant women, Kumasi Metropolis, Hepatitis B infection, knowledge, attitude, practices
©Ivy Nsiah et al. PAMJ-One Health (ISSN: 2707-2800). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Ivy Nsiah et al. Factors associated with knowledge, attitude and practice towards hepatitis B infection among pregnant women attending antenatal clinic in the Kumasi Metropolis, Ghana: a multi-centre hospital-based cross-sectional study. PAMJ-One Health. 2020;2:24. [doi: 10.11604/pamj-oh.2020.2.24.24716]
Available online at: https://www.one-health.panafrican-med-journal.com/content/article/2/24/full
Research 
Factors associated with knowledge, attitude and practice towards hepatitis B infection among pregnant women attending antenatal clinic in the Kumasi Metropolis, Ghana: a multi-centre hospital-based cross-sectional study
Factors associated with knowledge, attitude and practice towards hepatitis B infection among pregnant women attending antenatal clinic in the Kumasi Metropolis, Ghana: a multi-centre hospital-based cross-sectional study
Ivy Nsiah1, Charlotte Boachie Danquah2, Enoch Odame-Anto3,4, Christian Obirikorang3, William Kwame Boakye Ansah Owiredu3, Emmanuel Acheampong3,4, Yaa Obirikorang5, Evans Asamoah Adu3, Sampson Donkor3, &, Agartha Odame-Anto6,7
&Corresponding author
Introduction: Hepatitis-B Virus (HBV) is endemic in Ghana and mother-to-child transmission has been adjudged the common contributing factor. Therefore, this study examined factors associated with the knowledge, attitude, and practice of pregnant women towards HBV infection within the Kumasi Metropolis.
Methods: a hospital-based cross-sectional study design with a multistage random sampling was used to select 362 pregnant women from four major health facilities; Suntreso, Tafo, Manhyia and Kumasi South hospitals in the Kumasi Metropolis, Ghana. The pregnant women were made to complete a structured questionnaire composed of socio-demographic characteristics, as well as questions on knowledge, attitude and practices on HBV infection.
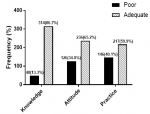
Results: majority of the pregnant women 314/362 (86.7%) had adequate knowledge of HBV infections. Also, 236/362 (65.2%) of them had positive attitudes whereas 217/362 (~60%) had good practices towards HBV infections. Respondents with no formal education were less likely to have adequate knowledge of HBV infection (OR (95% CI): 0.27 (0.11-0.65)), whereas pregnant women with tertiary education were 5.8 times more likely to have adequate knowledge on HBV (p-value <0.05). Moreover, educational level (χ2 = 22.04, p-value <0.0001), occupation (χ2 = 23.13, p-value <0.001) and marital status (χ2 = 6.64, p-value =0.036) were significantly associated with pregnant women´s attitude towards HBV infection. However, no significant association was observed between practices of HBV prevention and demographic variables (p-value >0.05).
Conclusion: pregnant women in the Kumasi Metropolis have adequate knowledge of HBV infection and its transmission mechanisms, but do not translate this into practice (do not adhere to preventive practices).
Hepatitis B infection is the world´s most common liver infection caused by a DNA-virus, the hepatitis B virus (HBV) [1]. The virus is known to contain numerous antigenic components, including hepatitis-B surface antigen (HBsAg), hepatitis-B core antigen (HBcAg), and hepatitis-B e antigen (HBeAg) [2]. HBV is relatively resilient and, in some instances, has been shown to remain infectious on environmental surfaces for more than 7 days at room temperature [1]. HBV causes a wide range of liver diseases including acute and chronic hepatitis, liver cirrhosis, and hepatocellular carcinoma [3]. The virus has several modes of transmission; contact with infected blood or semen, unsafe injections, blood transfusion, or dialysis [1,4]. According to the WHO 2019 report, the virus is most commonly transmitted from mother to child during birth [1]. In 2014, an estimated 2 billion people were reported to be infected globally with HBV and more than 350 million were chronic carriers [4]. HBV infection rates have been reported to be highest in the Western Pacific and African Region, where 6.2% and 6.1% of the adult population are infected respectively [1]. According to Naghavi, et al. [5] and WHO global report on hepatitis B infection [6], HBV infection is responsible for approximately 1.34 million deaths annually, similar to the annual number of deaths from HIV/AIDS (1.3 million), malaria (0.9 million), and tuberculosis (1.3 million). Studies in sub-Saharan Africa have reported prevalence rates ranging from 3% to 50% [7-9]. According to the Ghana Demographic Health Survey for 2013, Ghana is said to have an HBV prevalence rate between 8% and 15%, thus placing the country in the bracket of HBV endemic countries based on the WHO classification [10].
The common significant effect of HBV infection in pregnancy is perinatal or vertical transmission, especially in highly endemic areas, from an infected mother to child, and from an infected child to an uninfected child during early childhood [1,6]. In Sub-Saharan Africa including Ghana, the major mode of HBV transmission is mother-to-child transmission [6,11], and previous studies have reported a relatively high prevalence (2.4%-16.7%) of HBV infection among pregnant women in Ghana [12-18]. HBV also, has a direct adverse effect on foeto-maternal outcomes including impaired mental and physical health [19], neonatal jaundice, antepartum haemorrhage, and gestational diabetes mellitus [20, 21]. Against this background, it is vital to initiate strategies to engage women of reproductive age in the prevention of mother-to-child HBV infection transmission. Accordingly, these strategies would require women to understand the necessity of HBV testing during pregnancy, the benefits of timely infant HBV vaccination, and for infected mothers, the necessity of the newborn to complete HBV vaccine series. Unfortunately, few studies exist in Ghana [13,22,23], which have reported in parts, the knowledge, attitude and practices of pregnant women towards HBV infection. The low level of knowledge on HBV and common transmission mechanisms reported by these studies remains a missed opportunity to educate women on the effects of HBV complications on the mother and the developing foetus. This study, therefore, examined factors associated with the knowledge, attitude, and practice of pregnant women towards HBV infection within the Kumasi Metropolis.
Study population: the study population was pregnant women who attended the antenatal clinics at the four selected hospitals in the Kumasi Metropolis. Inclusion criteria for the study population were pregnant women and pregnant teenagers who had already made their first antenatal visit at one of the four selected hospitals in the Kumasi Metropolis. Pregnant women who had not yet made any antenatal visit (those who were now visiting antenatal care for the first time) were excluded from the study.
Sample size and sampling technique: from an estimated to a population of 4,141 registered pregnant women in the out-patient department records and considering 95% CI with 5% margin of error, the total estimated sample size was 365, using the formula below:
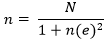
A multi-stage random sampling was used to select the participants in the proportion of total attendance per antenatal visit. Thus, the total sample consisted of 99, 82, 99 and 82 pregnant women from Suntreso, Tafo, Manhyia and Kumasi South hospitals, respectively. A systematic random sampling was used to select the subjects from each facility.
Description of questionnaire and data collection technique: a close-ended structured questionnaire was used for data collection. Sections on the questionnaire included 6-items on demographics, 18-items on knowledge, 9-items on attitude and 6-items on practices. The 18-item section included knowledge on the mode of transmission, effects and symptoms of HBV. Also, questions on attitude were related to feeling towards HBV infections and vaccination. Moreover, questions on practices were related to preventive measures towards HBV infection. Questionnaires were distributed to the pregnant women who had consented to participate in the study. The participants were asked to complete the questionnaires at the hospital in a place away from the other clients. Assistance was given to participants who could not read. The questionnaires were read and explained to them and they provided their answers. The questionnaires were collected immediately after it had been completed. The reliability of the questionnaire was pre-tested with Cronbach alpha of 0.876.
Scoring of questionnaire instrument: for each of the 18 knowledge-related statements, a score of 1 was assigned when a respondent gave a correct answer and 0 was assigned otherwise. A cut-off criterion of half mark; a score of ≥10 was classified as having adequate knowledge and a score <10 as having poor knowledge. Also, the 9-Item statements on attitude were each assigned a “yes =1” or “no =0”option to be selected. Accordingly, a cut-off level of <5 was considered as poor whereas ≥5 was considered a positive attitude towards HBV infection. Similarly, the 6-Item questions on practices were each scored as “correct answer=1” or “wrong answer=0” and dichotomized into good practices (a total score ≥4) and bad practices (a total score <4).
Ethical consideration: ethical clearance was provided by the University of Cape Coast Institutional Review Board (UCCIRB). The ethical clearance identification number given for this research was UCCIRB/CHAS/2015/15. Written informed consents were obtained from the participants after the details of the study were explained to them. Participation was voluntary and anonymity and confidentiality of responses were assured. The participants were informed of withdrawal from the study at any time during their participation without any penalty.
Data analysis: data analyses was performed using SPSS v. 20. Descriptive statistics in the form of percentages and cross-tabulation were used to evaluate demographic data, knowledge, attitude and practices. Inferential statistics to examine the relationships among study variables were computed using the Pearson chi-square tests and logistic regression analysis. P-values of <0.05 were considered statistically significant.
Overall, 362 participants completed the questionnaire with a response rate of 99.9%. Table 1 shows the summary statistics of demographic data. Majority 257/362 (71.0%) of the respondents were aged between 21-29 years. The highest level of education for most of the respondents was basic school 206/362 (59.9%). Also, majority of the respondents were traders/self-employed 236/262 (65.2%), married 270/362 (74.6%) and had 0-2 previous births 283/362 (78.2%). Moreover, most 243/362 (67.1%) of the respondents obtained information of HBV from healthcare providers, 120/362 (33.1%) from family/friends/neighbours/media and 98/362 (27.1%) from religious leaders/teachers. As shown in Table 2, 352/362 (97.2%) of the respondents had heard of HBV. Regarding knowledge of HBV transmission, more than half of the respondents (>50%) correctly answered that it can be transmitted sexually, during childbirth, by sharing of a toothbrush, and eating food pre-chewed by an infected person. Also, majority of the respondents correctly answered that HBV infection has signs, which mimic cold or flu.
However, 263/362 (72.7%) and 222/362 (61.3%) answered that jaundice and nausea, vomiting and loss of appetite are not common signs of HBV, respectively. Table 3 shows a summary of responses to attitude towards HBV infection. Most 190/362 (52.5%) of the respondents never thought they could get HBV infection. Also, most 187/362 (51.7%) of them attested that they will never tell others if they have HBV infection. Most of the respondents (>50%) did not know if healthy people need vaccination and have no idea if vaccination can be free or cheap during certain programs. Furthermore, a considerable percentage did not know if they need vaccination at their age 160/362 (44.2%), have no idea of places to get HBV immunizations 159/362 (44.0%), and never thought they will need HBV vaccinations 165/362 (45.6%). Results presented in Table 4 shows that most of the respondents 211/362 (58.3%) had not been screened for the HBV. Also, majority 300/362 (82.9%) of the respondents had not participated in programs related to HBV infection. However, 233/362 (64.4%) of them usually demanded barbers to change blades and also requested for safe equipments for ear and nose piercing. Practicing of safe sex was low among the respondents 103/362 (28.4%).
Knowledge, attitude, and practices towards HBV infection: majority of the respondents 314/362 (86.7%) were classified as having adequate knowledge. Also, 236/362 (65.2%) respondents were classified as having positive attitudes towards the HBV disease and 217/362 (˜60%) were classified as having good practices towards HBV infection (Figure 1).
Determinants of knowledge, attitude and practices towards HBV infection among pregnant women: the knowledge level of pregnant women towards HBV infection was significantly associated with educational status (χ2 [3] = 17.09, p-value =0.001) (Table 5). Also, educational level (χ2 [3] = 22.04, p-value <0.0001), occupation (χ2 [3] = 23.13, p-value <0.001) and marital status (χ2 [2] = 6.64, p-value =0.036) were significantly associated with respondents attitude towards HBV infection (Table 6). No significant association was observed between demographic variables and practices on HBV (p-value >0.05). In a logistic regression analysis (Table 7), respondents who had no formal education were less likely to have adequate knowledge of HBV infection (OR (95% CI): 0.27 (0.11-0.65)), whereas patients with tertiary education were 5.8 times more likely to have adequate knowledge of HBV (p-value >0.05). Also, respondents with tertiary education were 6.4 times likely to have a positive attitude towards HBV infection (p-value <0.05). While respondents who were unemployed were less likely to show positive attitude to HBV (OR (95% CI): 0.58 (0.35-0.94)), government employees were 10.7 times more likely to have a positive attitude towards HBV. Furthermore, respondents who were cohabiting were less likely to show a positive attitude towards HBV infection (OR (95%CI: 0.31 (0.12-0.75)) but more likely to show good practices towards HBV infection (OR (95%CI: 3.0 (1.00-9.07)).
This study examined the factors associated with knowledge, attitudes, and practices of pregnant women selected from four hospitals in the Kumasi Metropolis, towards HBV infection. The study found that the level of knowledge among pregnant women was relatively adequate, but this was not translated into their attitude and practices towards HBV infection. Whereas majority of the respondents had adequate knowledge of HBV infection, most of the respondents (over 30%) had poor attitudes and practices towards HBV infection. Also, this study observed that respondents who were educated up to the tertiary level were approximately 6 times more knowledgeable and showed a positive attitude towards HBV infection but not practices. On the other hand, respondents with no formal education were 73% less knowledgeable and 51% more likely to have a poor attitude but 42% more likely (but not statistically significant) to show good practices, towards HBV infection. Moreover, respondents who were cohabiting were less likely to show a positive attitude towards HBV infection but more likely to show good practices.
Previous studies conducted in Ghana regarding knowledge/awareness of pregnant women on HBV infection [13,22,23] present a common theme of low or poor knowledge, which is inconsistent with this present study. Again, a study by Cheng, et al. [22] at a teaching hospital in the Kumasi metropolis reported poor knowledge of HBV and its common transmission mechanisms which is inconsistent with our report. In this study, we observed that a reasonably high percentage of respondents were knowledgeable in sexual transmission, mother-to-child transmission and transmission through body fluids. From our findings, most of the respondents indicated that their major source of information regarding HBV infection was healthcare providers, followed by family/friends/neighbours/media and from religious leaders/teachers. This may imply that there is active HBV public awareness and educational campaigns at the primary level (at the hospitals). In other words, the possibility of consistent and accurate public sensitization by health officials on the infection during antenatal visit might be the probable explanation for the adequacy of knowledge observed in this study. Moreover, higher education was found to be a significant contributing factor for the relatively high knowledge obtained in this study. This finding is consistent with other several reports [13,22,23].
Although most of the respondents showed a positive attitude towards HBV infections, a considerably high percentage (34.8%) also demonstrated poor attitude. That is, most of the respondents never thought they could get HBV infection; will never tell others supposing they have HBV infection; did not know if healthy people need vaccination; have no idea if vaccination can be free or cheap during certain programs; did not know if they need vaccination at their age; had no idea of places to get HBV immunizations and never thought they will need HBV vaccinations. Interestingly, the observed data showed a significant positive attitude of pregnant women with tertiary education and government employees, but a negative attitude of unemployed/housewives, respondents with no formal education and respondents who were cohabiting. This finding may be ascribed to the fact that tertiary education and government employees are more likely exposed to screening and awareness programs on HBV, thus making them more willing to accept or adhere to HBV instructions than unemployed and not formally educated respondents. These are consistent with other related studies in Pakistan [24], Ghana [22], and Vietnam [25].
Interestingly, the findings of this study indicated that, most of the respondents had not been screened for HBV; had not participated in programs related to HBV infection; did not practice safe sex, and share food or utensils with others. This was a general indication of the adoption of poor practices towards HBV infection prevention. Also, most of the respondents were aware of HBV transmission through sex and body fluids but did not put it into practice. These findings were independent of education, marital status, occupation, age and the number of previous births. A study among Vietnamese Americans [26] and Vietnamese and Chinese in Australia [27] reported that low awareness on the possible transmission through unprotected sex was observed more in people practicing unsafe sex. Unlike our study, the subjects were pregnant women, and most of them were married. Thus, protected sex was nearly impossible. Also, in the Ghanaian environment, there is less coverage of sensitive and intimate (sexual) information [28]. Moreover, the majority of the respondents were aware that HBV cannot be transmitted via the sharing of cooking items. This together, could explain our observation.
Pregnant women in the Kumasi Metropolis have adequate knowledge on HBV infection and its transmission mechanisms, but do not translate this into practice or are not willing to adhere to preventive practices. Therefore, intensive public health education, screening and testing among pregnant women during antenatal visits are warranted. This will help in the management of future transmissions as well as inform the population about the significant negative side effects of the virus and the need to adopt preventive practices quickly.
What is known about this topic
- Hepatitis B infection is the world´s most common liver infection caused by a DNA-virus;
- The common significant effect of HBV infection in pregnancy is perinatal or vertical transmission, from an infected mother to child, and from an infected child to an uninfected child during early childhood.
What this study adds
- The study was a multi-centre one, which involved four hospitals;
- Findings from the study add up to the scarce data on knowledge, attitude and practices on HBV in pregnancy in Africa; specifically Ghana;.
- The findings confirm that the observations on this topic from developed countries, are also true in a low-income country like Ghana.
The authors declare no competing interest.
Ivy Nsiah, Charlotte Boachie Danquah and Enoch Odame-Anto were involved in conceptualization and supervision of the study, and were major contributors in writing the manuscript. Christian Obirikorang, William Kwame Boakye Ansah Owiredu and Emmanuel Acheampong were involved in data methodology and data curation. Yaa Obirikorang and Evans Asamoah Adu analysed and interpreted the patient data. Sampson Donkor and Agartha Odame Anto were involved in writing and reviewing the manuscript. All authors read and approved the final manuscript.
The authors acknowledge the efforts of the management of the Suntreso, Tafo, Manhyia and Kumasi South hospitals in the Kumasi Metropolis, Ghana. Also, we are most grateful to all the pregnant women who consented to partake in the study.
Table 1: socio-demographic characteristics of the study participants
Table 2: summary of responses to knowledge on HBV infection
Table 3: summary of responses to attitude towards HBV infection
Table 4: summary of responses to questions on practices towards HBV infection
Table 5: association between socio-demographic variables and knowledge on HBV
Table 6: association between socio-demographic variables and attitudes towards HBV infection
Table 7: logistic regression analysis of socio-demographic factors associated with knowledge, attitude and practices towards HBV infection
Figure 1: knowledge, attitude, and practices towards HBV infection
- WHO. Global hepatitis report. WHO. 2019.
- Prange R. Host factors involved in hepatitis B virus maturation, assembly, and egress. Medical microbiology and immunology. 2012;201(4):449-461. PubMed | Google Scholar
- Hollinger F, Liang T. Hepatitis B Virus, In: Knipe DM et al. eds Fields Virology Philadelphia. J Clinical Microbial. 2001;37(1):68-73.
- Trépo C, Chan HL, Lok A. Hepatitis B virus infection. The Lancet. 2014;384(9959):2053-2063. PubMed | Google Scholar
- Naghavi M, Abajobir AA, Abbafati C, Abbas KM, Abd-Allah F, Abera SF et al. Global, regional, and national age-sex specific mortality for 264 causes of death, 1980-2016: a systematic analysis for the Global Burden of Disease Study 2016. The Lancet. 2017;390(10100):1151-1210. PubMed | Google Scholar
- WHO. Global hepatitis report 2017. World Health Organization. 2017.
- Amidu N, Alhassan A, Obirikorang C, Feglo P, Majeed S, Timmy-Donkoh Eet al. Sero-prevalence of hepatitis B surface (HBsAg) antigen in three densely populated communities in Kumasi, Ghana. Journal of Medical and Biomedical Sciences. 2012;1(2). PubMed | Google Scholar
- Burnett RJ, Kramvis A, Dochez C, Meheus A. An update after 16 years of hepatitis B vaccination in South Africa. Vaccine. 2012 Sep 7;30 Suppl 3:C45-51. PubMed | Google Scholar
- Ugwuja E, Ugwu N. Seroprevalence of hepatitis B surface antigen and liver function tests among adolescents in Abakaliki, South Eastern Nigeria. The Internet Journal of Tropical Medicine. 2010;6(2):1726-1732. Google Scholar
- Survey GDH. Global report on the prevention and control of Viral Hepatitis in WHO Member States. WHO. 2013. Google Scholar
- Nguyen G, Garcia R, Nguyen N, Trinh H, Keeffe E, Nguyen M. Clinical course of hepatitis B virus infection during pregnancy. Alimentary pharmacology & therapeutics. 2009;29(7):755-764. PubMed | Google Scholar
- Elsheikh RM, Daak AA, Elsheikh MA, Karsany MS, Adam I. Hepatitis B virus and hepatitis C virus in pregnant Sudanese women. Virology Journal. 2007;4:104. PubMed | Google Scholar
- Kwadzokpui PK, Akorsu EE, Abaka-Yawson A, Quarshie SS, Amankwah SA, Tawiah PA. Prevalence and Knowledge of Hepatitis B Virus Infection among Pregnant Women in the Ningo-Prampram District, Ghana. International Journal of Hepatology. 2020;2020:7965146. PubMed | Google Scholar
- Cho Y, Bonsu G, Akoto-Ampaw A, Nkrumah-Mills G, Nimo JJ et al. The prevalence and risk factors for hepatitis B surface Ag positivity in pregnant women in eastern region of Ghana. Gut and liver. 2012;6(2):235. PubMed
- Ephraim R, Donko I, Sakyi SA, Ampong J, Agbodjakey H. Seroprevalence and risk factors of hepatitis B and hepatitis C infections among pregnant women in the Asante Akim North Municipality of the Ashanti region, Ghana; a cross sectional study. African health sciences. 2015;15(3):709-713. PubMed | Google Scholar
- Adjei CA, Asamoah R, Atibila F, Ti-enkawol GN, Ansah-Nyarko M. Mother-to-child transmission of hepatitis B: extent of knowledge of physicians and midwives in Eastern region of Ghana. BMC public health. 2016;16:537. PubMed | Google Scholar
- Luuse A, Dassah S, Lokpo S, Ameke L, Noagbe M, Adatara P et al. Sero-prevalence of hepatitis B surface antigen amongst pregnant women attending an antenatal clinic, Volta region, Ghana. Journal of public health in Africa. 2017 Jan 19;7(2):584. PubMed | Google Scholar
- V�lker F, Cooper P, Bader O, Uy A, Zimmermann O, Lugert R et al. Prevalence of pregnancy-relevant infections in a rural setting of Ghana. BMC pregnancy and childbirth. 2017;17(1):172. PubMed | Google Scholar
- Elinav E, Ben-Dov IZ, Shapira Y, Daudi N, Adler R, Shouval D et al. Acute hepatitis A infection in pregnancy is associated with high rates of gestational complications and preterm labor. Gastroenterology. 2006;130(4):1129-1134. PubMed | Google Scholar
- Tse KY, Ho LF, Lao T. The impact of maternal HBsAg carrier status on pregnancy outcomes: a case-control study. Journal of hepatology. 2005;43(5):771-775. PubMed | Google Scholar
- Katke R. The impact of maternal HbsAg carrier status on pregnancy outcomes: an institutional experience. Gynecol Obstet (Sunnyvale). 2015;5(288):2161-0932. Google Scholar
- Cheng A, Jose J, Larsen-Reindorf R, Small C, Nde H, Dugas L et al. A Survey Study of Pregnant Women and Healthcare Practitioners Assessing the Knowledge of Attitudes and Practices of Hepatitis B Management at a Teaching Hospital in Kumasi, Ghana, West Africa. Open Forum Infectious Diseases. 2015 Sep 1;2(4):ofv122. PubMed | Google Scholar
- Abdulai MA, Baiden F, Adjei G, Owusu-Agyei S. Low level of Hepatitis B knowledge and awareness among pregnant women in the Kintampo North Municipality: implications for effective disease control. Ghana medical journal. 2016;50(3):157-162. PubMed | Google Scholar
- ul Haq N, Hassali MA, Shafie AA, Saleem F, Farooqui M, Haseeb A, Aljadhey H. A cross-sectional assessment of knowledge, attitude and practice among Hepatitis-B patients in Quetta, Pakistan. BMC Public Health. 2013;13(1):448. PubMed | Google Scholar
- Dahlström E, Funegård Viberg E. Knowledge about hepatitis B virus infection and attitudes towards hepatitis B virus vaccination among Vietnamese university students in Ho Chi Minh City:-A quantitative study. diva-portal. 2013. Google Scholar
- Ma GX, Shive SE, Fang CY, Feng Z, Parameswaran L, Pham A, Khanh C. Knowledge, attitudes, and behaviors of hepatitis B screening and vaccination and liver cancer risks among Vietnamese Americans. Journal of Health Care for the Poor and Underserved. 2007 Feb;18(1):62-73. PubMed | Google Scholar
- Vu LH, Gu Z, Walton J, Peet A, Dean J, Dunne MP, Debattista J. Hepatitis B knowledge, testing, and vaccination among Chinese and Vietnamese adults in Australia. Asia Pacific Journal of Public Health. 2012;24(2):374-384. PubMed | Google Scholar
- Helegbe GK, Tanko F, Aryee PA, Lotsu SA, Asaarik MJ, Anaba F. High Hepatitis B Seroprevalence, Low Knowledge, and Poor Attitude towards Hepatitis B Virus Infection among Market Women in Bolgatanga Metropolis in the Upper East Region of Ghana. Journal of Tropical Medicine. 2020 May 27;2020:4219413. PubMed | Google Scholar