Factors associated with poor compliance to rabies post-exposure prophylaxis among dog bite victims in Maswa District in Tanzania: a cross-sectional study
Budodi Walwa Walwa, Esther Gwae Kimaro, Emmanuel Abraham Mpolya, Maganga Sambo
Corresponding author: Budodi Walwa Walwa, Department of Health and Biomedical Sciences, School of Life Sciences and Bioengineering, Nelson Mandela African Institution of Science and Technology, P.O. Box 447, Arusha, Tanzania 
Received: 23 Feb 2024 - Accepted: 15 May 2024 - Published: 22 May 2024
Domain: Public health
Keywords: Rabies, post-exposure prophylaxis, dog bite victims, compliance, individual factors, societal factors, Maswa District, Tanzania
©Budodi Walwa Walwa et al. PAMJ-One Health (ISSN: 2707-2800). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Budodi Walwa Walwa et al. Factors associated with poor compliance to rabies post-exposure prophylaxis among dog bite victims in Maswa District in Tanzania: a cross-sectional study. PAMJ-One Health. 2024;14:2. [doi: 10.11604/pamj-oh.2024.14.2.41309]
Available online at: https://www.one-health.panafrican-med-journal.com/content/article/14/2/full
Research 
Factors associated with poor compliance to rabies post-exposure prophylaxis among dog bite victims in Maswa District in Tanzania: a cross-sectional study
Factors associated with poor compliance to rabies post-exposure prophylaxis among dog bite victims in Maswa District in Tanzania: a cross-sectional study
![]() Budodi Walwa Walwa1,2,3,&, Esther Gwae Kimaro1, Emmanuel Abraham Mpolya1, Maganga Sambo2
Budodi Walwa Walwa1,2,3,&, Esther Gwae Kimaro1, Emmanuel Abraham Mpolya1, Maganga Sambo2
&Corresponding author
Introduction: administering rabies post-exposure prophylaxis (PEP) in a timely and appropriate manner remains the most fundamental measure for preventing human rabies. However, a number of barriers to accessing and completing PEP exist.
Methods: a cross-sectional study was carried out from April to July 2022 to examine individual and societal barriers to accessing human rabies PEP in Maswa in Maswa District, Tanzania. Dog bite patients were interviewed to gather information about the circumstances of the bite, as well as the availability, affordability, and compliance with PEP. Descriptive and inferential analyses were conducted to address the research question.
Results: of the 264 bite patients, 57.6% were male and 67.2% were under 15 years old. Dog bites accounted for the highest proportion of cases 95.5% (n=252) and category-III bites were most frequently observed 63% (n=167). About 45.1% (n=119) of patients traveled over 25 kilometers (km) from their residences to reach PEP clinics. The average cost for obtaining PEP doses was USD 51.1. Only 3.8% (n=10) of patients received all five recommended PEP doses. Travel distances and costs were significant factors for poor PEP compliance. Patients who traveled by bicycle to health facilities had higher odds of PEP compliance (aOR =17.12: 95% CI: 14.12 - 23.42) than those who walked (aOR = 6.88: 95% CI: 1.28 - 26.13). Furthermore, patients who utilized buses were four times more likely to comply to PEP (aOR = 4.23, 95% CI: 1.06 - 16.46) than those using motorcycles. Bite patients from urban areas were 6 times more likely to complete the recommended PEP (aOR = 5.79, 95% CI: 1.29 - 15.20) than their rural counterparts.
Conclusion: findings from this study inform measures to improve compliance to rabies PEP among dog bite victims. These measures include subsidizing the cost of PEP, improving PEP accessibility, and raising awareness about the dangers of rabies particularly in seeking and completing the recommended PEP focusing on rural communities.
Rabies remains a major public health threat to over three billion people worldwide. The World Health Organization (WHO) estimates that 59,000 human rabies deaths occur every year; 95% of those occur in Asia and Africa [1,2]. Domestic dogs are the main source of human rabies deaths, contributing up to 99% of all rabies transmissions to humans. After bite exposure, the rabies virus enters the wound through infected saliva. It then travels along the nerves to reach the spinal cord and takes 3-12 weeks to reach the brain, depending on the amount of virus inoculated, and its proximity to the central nervous system. Once the virus reaches the brain, it undergoes rapid multiplication before spreading to the salivary glands. Subsequently, the animal starts exhibiting clinical signs of rabies [2]. Once clinical signs appear, rabies invariably progresses to fatal encephalitis [3,4]. Although rabies is fatal once symptoms appear, it can be prevented through timely administration of rabies post-exposure prophylaxis (PEP) to bite victims [5]. The PEP protocol recommended by the WHO comprises immediate bite wound washing or flushing, administration of rabies vaccine, and in case of severe wounds, additional injection of rabies immunoglobulin (RIG) in and around the wound [5-7]. Despite more than 130 years having passed since Pasteur's first human rabies vaccine was discovered, tens of thousands of deaths from rabies still occur each year [8,9].
On the other hand, human rabies deaths are preventable through the implementation of annual mass dog vaccination campaigns to control the disease in reservoir populations (domestic dogs), and enhancing community awareness and education regarding bite prevention and the significance of vaccinating dogs against rabies [10,11]. Mass dog vaccination (MDV) has eliminated dog-mediated rabies from high-income countries and much of Latin America and the Caribbean [9]. Indeed, successful dog vaccination campaigns have been shown to reduce demand for expensive PEP [6]. Consequently, international organizations including the World Health Organization (WHO), the World Organization for Animal Health (WOAH), the Food and Agriculture Organization of the United Nations (FAO), and the Global Alliance for Rabies Control (GARC) have recognized that the elimination of dog-mediated rabies is feasible through MDV and have now launched a “United Against Rabies forum” to advocate the global human rabies elimination by 2030 [7].
The human rabies vaccine serves as the cornerstone of PEP, assisting the body in developing immunity against the rabies virus [2,5]. Regimens for PEP typically involve the administration of rabies vaccine in multiple doses, with variations such as 3 doses, 4 doses, or 5 doses [5]. The utilization and availability of PEP regimens vary among countries, with different protocols and practices in place [6,8,10]. For example, the United States of America, despite having effectively controlled rabies, still incurs substantial costs associated with PEP compared to African countries where the disease remains endemic but still spends the least on PEP [6,10]. In Tanzania, the 3-dose regimen is widely used for rabies [8,10-13].
In rabies-endemic countries, the high cost of PEP affects the health system budget and limits the capacity of health facilities to stock adequate PEP [14-17]. As a result, access to PEP is often limited, particularly in urban public and private health facilities, and is characterized by frequent shortages and high costs [11-13]. Consequently, many bite victims, especially those from marginalized and rural populations are disproportionately affected, experiencing the greatest burden with the least access to PEP [11]. As a result, they cannot afford or comply with the recommended PEP regimens [5,18-23]. In Tanzania, approximately 25% of bite patients do not seek care, and over 15% of bite patients do not initiate PEP despite reaching health facilities [13]. Additionally, lack of awareness about the dangers of rabies [14], and ignorance regarding the rabies status of biting animals act as significant factors contributing to poor access to PEP [24-28].
Maswa District, located in Tanzania, represents a setting where rabies research and control interventions have not been extensively conducted. The district has a relatively high dog-to-human ratio of 1:7, and between 2018 and 2020, approximately 906 individuals were bitten by suspected rabid animals in the district, with only 406 receiving human rabies PEP [14]. However, little is known about the individual and societal barriers that affect access to PEP and compliance with treatment regimens in this context. This study aimed to examine the individual and societal barriers to accessing human rabies PEP in Maswa District, Tanzania.
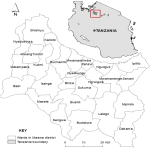
Study area: this study was conducted in Maswa District, Tanzania which lies between the latitudes 2.45 and 3.15 South of the Equator and between the longitudes of 33.00 and 34.10 east of the Greenwich Meridian (or their representatives). Maswa district comprises both rural and urban areas divided into three divisions: Mwagala, Sengerema, and Nung´hu. Situated at an altitude ranging from 1,200 to 1,300 meters above sea level, the district has a population of around 344,125 individuals, with the majority belonging to ethnic groups such as the Sukuma and Nyamwezi (Figure 1). The local economy revolves around agriculture and livestock rearing, utilizing more than 2,475 square kilometers of arable land for crop cultivation.
Study design: we used a cross-sectional study design to evaluate the proportion of animal bites and assess the compliance with post-exposure prophylaxis (PEP) vaccination to bite victims. We retrieved data from the health care registry and then followed bite victims to their homes for interviews. During interviews, we collected information on respondent´s social and individual factors, the animals responsible for bites, the circumstances of the bites, behaviors related to seeking PEP, outcomes of the bitten animals, as well as the medical and non-medical costs associated with PEP treatments at healthcare facilities.
Criteria for sample selection of animal bite patients: the inclusion criteria for sample selection were patients with a history of bite exposure from either a probable or suspected rabid animal, regardless of the patient's age. We included bite patients who fulfilled the criteria for the World Health Organization's (WHO) classification of exposure types II and III [19]. Exposure type II encompassed nibbling, minor scratches, abrasions without bleeding, or licks on broken skin caused by suspected rabid animals. Exposure type III refers to single or multiple transdermal bites or scratches with saliva contamination or bleeding. However, if a participant reported more than one exposure during the research period, only the data corresponding to the initial exposure was included. During our interviews, we inquired about individuals who were bitten by the same dogs but did not seek PEP. These additional victims were also incorporated into our study and interviewed. We excluded bite patients who had been bitten by normal dogs (not rabid animals), and bite patients with bite exposure type I. The bite exposure type I was categorized by WHO as patients who have been bitten by a normal or aggressive animal that is not suspected of being rabid, and who have not broken skin from the bite [5]. These patients may include those who have touched or fed the suspect animal but do not have any broken skin from the bite
Sample sizes: the sample size for the study was determined using the Kish and Leslie formula:
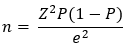
Where N represents the sample size, Z is 1.96 for a 95% confidence interval, P is the prevalence of health seeking and e is the precision level [20]. We used a precision level (marginal error) of 5% as recommended by Niang [29], and based on previous research on health-seeking behaviors in Tanzania, which indicated that approximately 75% of bite patients seek medical care [11,13,18], the value of P was therefore set at 0.75. We also used a confidence level of 95% (which corresponds to the Z = 1.96). With these values, a minimum sample size of 288 bite patients was obtained. To account for a potential non-response rate of 10%, additional 32 bite patients were added to the sample size giving a final sample size of 320 participants.
Data collection procedures: the study collected data on animal bite patients reporting injuries in health facilities within the Maswa district from March 2022 to September 2022. The names of animal bite patients were collected from the Animal Bite Registry and recorded at Maswa District Hospital, Mwagala Dispensary, and Wazazi Dispensary. These animal bite records served as the primary references for tracing bite victims. Researchers then followed bite patients to their homes for interviews and obtained fine-scale geo-referenced data on rabies incidence and transmission. The interviews collected detailed information on individual and societal factors. Individual factors included: gender, age, educational level, body part affected, wound dimensions, and means of transportation. Societal factors included: occupation, residential location, healthcare costs, usage of traditional herbal, involvement in agricultural activities, availability of PEP in medical centers, religious convictions, and proximity to medical facilities from one's home. Parents/guardians were interviewed on behalf of participants aged under 15 years.
Data analysis: a descriptive analysis was conducted to explore factors influencing the completion of PEP among bite patients. Chi-square tests were utilized to examine associations whereby the proportion of non-compliance on PEP was expressed in percentage. Logistic regression was performed to determine the determinants of non-compliance, with a binary outcome defined as completed PEP (received ≥ 3 doses, assigned as compliant) or not completed PEP (received < 3 doses, assigned as non-compliant), against individual and societal variables of the patients. From the chi-squared test, all variables with p-value < 0.05 were selected for regression analysis. Univariate and multivariate logistic regressions were conducted to obtain the effects of different predictors on the binary outcome. Results from the univariate logistic regression are summarized in odds ratios while those from the multivariate logistic regression are summarized in adjusted odds ratios.
Ethical consideration: this study was undertaken following the guidelines outlined in the Declaration of Helsinki [22]. Ethical clearance was granted by the Institutional Review Board of the Ifakara Health Institute (IHI/IRB/No. 16-2022). Additionally, necessary permissions were obtained from the District Executive Director (DED) and Village Executive Officers (VEOs) to collect data, ensuring participant rights were upheld throughout the study. To obtain medical records, the researchers obtained permission from the officer-in-charge of each health facility. Consent was obtained, and a release form was signed before collecting these medical records. Informed consent was obtained from participants after explaining the study's background and purpose. Confidentiality was maintained, and only those who provided consent and signed the informed consent forms were interviewed.
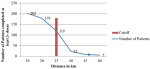
Socio-demographic characteristics of animal bite patients health seeking: we conducted a study involving 320 individuals who were bitten by animals from January 1, 2019, to June 30, 2022. Among these patients, 82.5% (n=264) met the case definition for bites caused by probable rabid animals, with 22% (n=58) in 2019, 37% (n=98) in 2020, 33% (n=87) in 2021, and 8% (n=21) in 2022. Only bite patients who met the case definition for bites caused by probable rabid animals were reported in this result section. This resulted in an annual probable bite incidence of 13 per 100,000 population in 2019, 22 per 100,000 population in 2020, and 19 per 100,000 population in 2021, with an average of 18 per 100,000 population per year. Among the 264 patients investigated, the majority were males, accounting for 56.1% (n=148). Approximately 67.0% (n=177) of the bite patients were under the age of 15, with a median age of 8.5 years (Table 1). Most of the bite victims, 87.0% (n=230) came from rural areas, and 84.1% (n=222) had primary school education, with only 1.1% (n=3) being illiterate. Furthermore, only a small percentage of patients, 3.8% (n=10), completed the WHO-recommended five-dose rabies vaccine regimen according to the Essen intramuscular protocol [23]. A total of 56.1% (n=148) successfully completed the full 3-dose regimen, indicating their compliance to the treatment plan. Following WHO guidelines, patients who completed the 3-dose regimen were considered compliant with PEP. A majority of patients (N=119) residing within a 25-kilometer (km) radius of PEP clinics completed the three doses, whereas only a few patients (n=8) living more than 60 km away from PEP clinics completed the three doses (Figure 2).
Table 2, presents descriptive statistics for three variables associated with the associated costs of accessing PEP. On average, patients spent 11.38 United States Dollars (USD) on transportation, with fares ranging from 0.43 USD to 29.76 USD (depending on distance from homes to PEP clinics). The average accommodation fee (only for patients leaving away from PEP clinics) was 2.76 USD, varying between 0.85 USD and 10.62 USD (depending on the quality of the hotel and number of guests (some patients who were escorted to the hospital by their parents/relatives paid more). The mean medical costs (including PEP cost) was 36.96 USD, with prices ranging from 1.28 USD to 74.40 USD for the three PEP doses (medical costs varied depending on the wound size, those who required surgical operation paid more, and PEP cost fluctuated).
Bite characteristics and health-seeking behaviors: most animal bites (95.5%, n=252) were inflicted by dogs, while a small percentage (4.5%, n=12) were from other animals such as cats. Approximately three-quarters (74.9%, n=198) of the bites occurred from the victims' dogs. Among the animal bite victims studied, 63.3% (n=167) fell into WHO category III exposure, indicating more severe bites, while 36.7% (n=97) were classified as WHO category II bites. The majority of individuals (63.6%, n=168) were bitten away from their homes, often while fetching water or returning from school. Following the animal bite, 55.0% (n=145) of the victims reported washing the wound thoroughly with soap and running water for 15 minutes. Additionally, the majority of bite victims (87.1%, n=230) sought medical attention at health facilities within 24 hours of the bite.
Factors associated with poor compliance and accessibility to rabies PEP: the final model of multiple logistic regression was performed to analyze the individual and societal impediments impacting the accessibility to PEP and compliance. Individual factors included sex, age, patient's level of education, the body part affected, wound size, and transportation means. Societal factors comprised occupation, place of residence, cost of healthcare, utilization of herbal medicine (often influenced by cultural and societal norms), engagement in agricultural activities, PEP availability in healthcare facilities, incidents involving biting animals (linked to factors like public health policies and animal control measures), religious beliefs, and proximity from one's residence to the healthcare facility.
The final model of analysis showed that: occupation, sex, residence, means of transportation used for seeking PEP, healthcare costs, and reported reasons for non-compliance such as preference for herbal medicine, agricultural activities, and presence of PEP at the health first PEP clinic were the factors associated with patients' compliance with rabies post-exposure prophylaxis. Other factors including age, a biting animal, religion, wound size, part of body bitten, distance between residence (home) and health facility, and education level were not significantly associated with PEP compliance. Table 3 provides the individual and societal factors of rabies patients that were significantly associated with compliance with PEP in rural and urban areas.
Patients who spent low on healthcare, specifically those spent less than 36.96 USD per three doses had significantly higher compliance rates. On the other hand, the unavailability of PEP at the Health First PEP clinic had a significantly low compliance rate (aOR = 1.32, 95% CI: 1.21-6.25, p = 0.011) as patients were referred to other major hospitals for PEP. Additionally, those who opted for (preferred) herbal medicine instead of PEP and who reported being busy (occupied) with agricultural activities during bite exposure were significantly associated with low compliance rates, with odds ratios of 0.88 (95% CI: 0.06-0.98, p = 0.021) and 0.37 (95% CI: 0.21-0.98, p = 0.047) respectively. Bite patients from urban areas had substantially higher compliance (aOR = 5.79, 95% CI: 1.29-15.20, p = 0.028). For occupations, farmers exhibited higher compliance rates (aOR = 2.21, 95% CI: 1.36-6.52, p = 0.031). Females demonstrated high odds (aOR = 12.26, 95% CI: 1.18-35.38, p = 0.021) of PEP compliance than males. In terms of the mean of transport to the PEP clinics, those who used bicycles demonstrated the highest odds ratio for PEP compliance (aOR = 17.12, 95% CI: 14.12-23.42, p = 0.017), followed by feet (OR = 6.88, 95% CI: 1.28-26.13, p = 0.020).
Age-wise analysis indicates lower compliance among individuals aged 16-30 years (aOR = 0.67, 95% CI: 0.31-0.89, p = 0.428) compared to those aged 0-19 years. Likewise, patients aged 45 years above indicate low compliance with rabies PEP (aOR = 0.74, 95% CI: 0.13-0.93, p = 0.520) though statistically insignificant. Individuals bitten by cats indicate lower compliance (aOR = 0.32, 95% CI: 0.31-0.97, p = 0.220), while those with small-sized wounds show higher compliance (aOR = 2.02, 95% CI: 1.01-3.09, p = 0.182). In addition, patients living within a distance of 20-39 km from health facilities had higher compliance (aOR = 3.16, 95% CI: 2.24-7.57, p = 0.464) compared to those found within 0-19 km, while those within 40-70 km show lower compliance (aOR = 0.65, 95% CI: 0.6-0.96, p = 0.838), though not statistically significant. Patients bitten on the lower parts of the body show higher compliance (aOR = 1.26, 95% CI: 1.08-8.38, p = 0.414) compared to those bitten on the upper parts. Patients with primary school education demonstrate higher compliance with rabies PEP protocols, as indicated by high odds (aOR=1.47, 95% CI: 1.05-2.78, p = 0.171). However, religious affiliation, particularly being Muslim, shows a lower odds ratio for compliance (aOR = 0.47, 95% CI: 0.13-0.96, p = 0.923) compared to Christian religious groups, although this difference is not statistically significant.
Findings from this study indicated that more than fifty percent of dog bite victims were males and were under the age of 15 years, the majority reside in rural areas (84%) within a 25km radius of health facilities. This finding is consistent with a study conducted in the Philippines whereby most of the participants (61%) were male [16]. It was also found that a small percentage of patients 4% completed the WHO-recommended five-dose rabies vaccine regimen according to the Essen intramuscular protocol [23].
The study revealed a significant association between female gender and PEP compliance, which may be due to differences in activity patterns and cultural factors [23-24]. These findings are consistent with other research showing that females are more likely to seek timely anti-rabies treatment [5,25-27]. Women perceive the risk of rabies infection more seriously than men, leading to greater compliance with PEP protocols following animal bites or exposure incidents. This signifies a gender imbalance in PEP. To improve PEP uptake among males, it is crucial to address the barriers and challenges they face in accessing medical care after an animal bite. The study findings suggest that patients who used bicycles or walked to PEP clinics were more likely to complete the recommended PEP doses. This might be due to their proximity to health facilities and the absence of transportation costs. On the other hand, patients who had to bear transportation expenses, such as those using motorcycles, were less likely to comply with the PEP regimen, likely due to the financial burden associated with transport and other medical costs related to PEP.
Living in a rural area has been identified as a factor that increases the risk of exposure to animals carrying the rabies virus and, consequently, the likelihood of contracting human rabies [20,28,30]. In our study, we found that only less than 2% of respondents living in rural areas completed their human PEP. This finding aligns with the general relationship between residence and health outcomes, where individuals in rural areas often face challenges in accessing healthcare resources and experience higher rates of certain health conditions [11,12,31]. In rural areas, people are more likely to come into contact with wildlife such as bats, raccoons, foxes, and skunks, which are common carriers of the rabies virus [20,32]. Additionally, there may be a higher prevalence of free-roaming dogs and cats that have not been vaccinated against rabies due to the financial constraints faced by their owners [28,33-35]. These factors contribute to the increased risk of exposure to rabies in rural communities and highlight the importance of addressing the specific challenges faced by individuals living in these areas.
Occupation (farmer) was also found to be positively related to PEP compliance. In agreement with Eccles et al. [36] and Sing [37] it has been observed that particular occupations may increase individuals' susceptibility to certain diseases while also affording them improve the accessibility of treatment. Businessmen, in contrast, often experience lower access to rabies PEP when compared to livestock keepers. This disparity can be attributed to their limited exposure to animals, which reduces their awareness of the risks associated with rabies and the importance of PEP [38]. Additionally, businessmen may encounter healthcare accessibility issues, and healthcare prioritization barriers, particularly in regions with lower rabies incidence [39]. In addition, this study found that animal bite patients involved in crop farming activities were more likely to seek and complete PEP compared to those in livestock occupations. Farmers may have better access to healthcare services, including clinics and hospitals, compared to livestock keepers who may work in more remote or rural areas. As a result, individuals in these occupations may perceive themselves to be at higher risk of contracting rabies and thus may be more proactive in seeking medical care and completing PEP. On the same line, Elelu et al. [40] and Omondo et al. [41] highlighted that farmers primarily engaged in crop cultivation demonstrate to have better access to rabies PEP compared to livestock keepers, largely owing to their proximity to healthcare facilities, better financial resources, and insurance coverage.
Those who spent the low cost of healthcare, specifically those below $36.96 (medical cost) for three doses, have been associated with high compliance rates. When cost is low most people can afford but when cost rises most cannot afford it. High healthcare costs in many developing countries impose a significant economic burden on individuals and households, particularly those with low incomes. High healthcare costs in many developing countries may worsen economic strain on individuals and families, especially those with limited financial resources. When costs of healthcare are low, they are generally manageable for a larger portion of the population, but as costs rise, affordability becomes a critical issue for many. This economic burden can lead to difficult choices, such as foregoing necessary medical care or sinking into debt to cover expenses. Ultimately, the inability to afford healthcare undermines individuals' well-being and perpetuates cycles of poverty, hindering socioeconomic development in these regions. The availability of rabies PEP is significantly associated with high compliance rates. When PEP is not available patients are referred to other major hospitals for PEP. Most people couldn´t afford it due to transportation costs, accommodation costs, and other expenses. Therefore, PEP clinics need to be decentralized (make PEP locally available) to increase compliance with PEP for poor bite victims. Even if PEP is provided for free during GAVI investment if PEP will not be decentralized people will still be dying because will not afford transport and other costs To strengthen the association between availability and compliance policymakers should focus on expanding access to PEP (decentralizing PEP clinics) within the district. For example, in Maswa, PEP clinics should be decentralized to each division. This will increase access and reduce PEP-associated costs in both urban and rural areas, implementing community-based educational programs, and ensuring a reliable supply chain to prevent shortages.
Limitations: it is important to acknowledge the limitations of a study as it helps to contextualize the findings and understand their limitations. In this case, the study is limited by the fact that it only includes patients who sought care in health facilities and does not include those who did not seek medical attention. This may lead to a bias in the results and conclusions, as the study is only capturing a specific subset of patients with animal bites.
Additionally, the study is limited by the lack of laboratory confirmation of rabies cases, which means that there may be some uncertainty about the diagnoses. This can affect the accuracy of the results and the conclusions drawn from the study. The reliance on patients' recollections for data on factors that affect patients´ compliance to human rabies PEP may also introduce bias, as patients may not accurately remember or report all relevant information. Furthermore, the study is cross-sectional, which means that it provides a snapshot of the situation at a specific point in time and cannot establish cause-and-effect relationships. Therefore, the findings should be interpreted with these limitations in mind and be used to inform further research.
Human rabies continues to pose a significant public health challenge in Maswa, Tanzania. Only a small percentage (3.8%) of patients completed the WHO-recommended five-dose rabies vaccine regimen. It is important to provide thorough counseling to patients seeking rabies PEP to enhance compliance. Firstly, there is a significant gender disparity in PEP compliance, with females showing higher compliance rates, therefore targeted interventions to improve male uptake of PEP are highly needed. Additionally, promoting the use of bicycles or walking as an affordable means of transportation to PEP clinics could enhance compliance, particularly among those burdened by transportation costs. Moreover, given the disproportionately low completion rates of PEP among rural residents, efforts should focus on increasing access to healthcare resources and raising awareness about the importance of timely treatment. This may include expanding healthcare infrastructure in rural areas and providing financial support to facilitate access to PEP services among rural residents. Furthermore, the positive correlation between occupation and PEP compliance suggests the need for interventions for specific occupational groups, for instance, educational outreach programs for businessmen are needed to improve their awareness of rabies risks and the importance of PEP compliance. Lastly, it is important to ensure that PEP is affordable and readily accessible while improving the efficiency of the supply chain to enable quick access and increase compliance rates.
What is known about this topic
- A very small proportion of patients (3.8%) successfully finished the recommended five-dose rabies vaccine regimen following the essen intramuscular protocol;
- There is a significant association between gender and PEP compliance in Maswa, with females being more likely to adhere to PEP protocols;
- Residents of Maswa, particularly those living in rural areas, face challenges in accessing healthcare resources and completing PEP regimens due to geographical barriers and limited healthcare infrastructure; high healthcare costs pose a significant economic burden on individuals and households in Maswa, impacting their ability to access and complete PEP regimens.
What this study adds
- This study adds valuable insights to the field of research on factors associated with patients' compliance to human rabies PEP; it identifies specific factors that influence PEP compliance, including gender, residence in rural areas, occupation, and means of transportation used to seek PEP;
- The findings highlight the need to address barriers faced by males in accessing medical care after an animal bite and the importance of targeting interventions to improve PEP uptake among this group; the study also emphasizes the challenges faced by individuals living in rural areas, such as increased exposure to rabies and limited healthcare access, calling for tailored strategies to address these unique circumstances;
- Furthermore, the study emphasizes the role of occupation in PEP compliance, showing higher compliance among livestock keepers compared to agriculturalists; this emphasizes the importance of raising awareness among agriculturalists and ensuring better access to healthcare resources for this occupational group.
The authors declare no competing interests.
this work was supported by Ifakara Health Institute (IHI) Training Department, funding awarded to Budodi Walwa Walwa as part of the MSc studentship award.
Conceptualization: Budodi Walwa Walwa, Maganga Sambo, Esther Gwae Kimaro. Data curation: Budodi Walwa Walwa. Formal analysis and investigation: Budodi Walwa Walwa, Maganga Sambo. Supervision: Maganga Sambo, Esther Gwae Kimaro, Emmanuel Abraham Mpolya. Visualization: Budodi Walwa Walwa. All the authors have read and agreed to the final manuscript.
The authors would like to acknowledge the staff of hospitals and dispensaries, and local community members, who provided invaluable assistance with data collection. We are grateful to the research assistants for their help in conducting the surveys. Many thanks to the anonymous reviewers for constructive feedback that helped improve this manuscript.
Table 1: summary of the socio-demographic characteristics of animal bite patients
Table 2: average costs related to accessing PEP services
Table 3: model results of an association between compliance of post-exposure rabies and societal and individual factors of animal bite patients in rural and urban areas with 95% confidence interval (CI) and p-value
Figure 1: the map of Tanzania (top left corner) and Maswa district showing the wards of the study area
Figure 2: patients' compliance to PEP against distance from health facility
- Fooks AR, Banyard AC, Horton DL, Johnson, McElhinney NLM, Jackson AC. Current status of rabies and prospects for elimination. Lancet. 2014 Oct 11;384(9951):1389-99. PubMed | Google Scholar
- Roine RO, Hillbom M, Valle M, Haltia M, Ketonen L, Neuvonen E et al. Fatal encephalitis caused by a bat-borne rabies-related virus: Clinical findings. Brain. 1988 Dec:111 ( Pt 6):1505-16. PubMed | Google Scholar
- Dacheux L, Delmas O, Bourhy H. Human rabies encephalitis prevention and treatment: progress since Pasteur's discovery. Infectious Disorders-Drug Targets (Formerly Current Drug Targets-Infectious Disorders). 2011 Jun 1;11(3):251-99. PubMed | Google Scholar
- Dimaano EM, Scholand S, Alera MTP, Belandres DB. Clinical and epidemiological features of human rabies cases in the Philippines: a review from 1987 to 2006. Int J Infect Dis. 2011 Jul;15(7):e495-9. PubMed | Google Scholar
- WHO: Rabies vaccines: WHO position paper, April 2018 - Recommendations. Vaccine. 2018;36(37):5500-5503. PubMed | Google Scholar
- Mpolya EA, Lembo T, Lushasi K, Mancy R, Mbunda EM, Makungu S et al. Toward elimination of dog-mediated human rabies: Experiences from implementing a large-scale demonstration project in Southern Tanzania. Front Vet Sci. 2017 Mar 6;4:21. PubMed | Google Scholar
- Tidman R, Thumbi SM, Wallace R, de Balogh K, Iwar V, Dieuzy-Labaye I et al. United against rabies forum: the one health concept at work. Front Public Health. 2022 Apr 13;10:854419. PubMed | Google Scholar
- Hampson K, Coudeville L, Lembo T, Sambo M, Kieffer A, Attlan M et al. Global Alliance for Rabies Control Partners for Rabies Prevention. 2015. Estimating the global burden of endemic canine rabies. PLoS Negl Trop Dis. 2015;9(4):e0003709. Google Scholar
- Hampson K, Coudeville L, Lembo T, Sambo M, Kieffer A, Attlan M et al. Estimating the Global Burden of Endemic Canine Rabies. PLoS Negl Trop Dis. 2015 Apr 16;9(4):e0003709. PubMed | Google Scholar
- Nadal D, Hampson K, Lembo T, Rodrigues R, Vanak AT, Cleaveland S. Where Rabies Is Not a Disease, Bridging Healthworlds to Improve Mutual Understanding and Prevention of Rabies. Front Vet Sci. 2022 Jun 15;9:867266. PubMed | Google Scholar
- Sambo M, Cleaveland S, Ferguson H, Lembo T, Simon C, Urassa H et al. The Burden of Rabies in Tanzania and Its Impact on Local Communities. PLoS Negl Trop Dis. 2013 Nov 7;7(11):e2510. PubMed | Google Scholar
- Lembo T, Hampson K, Haydon DT, Craft M, Dobson A, Dushoff J et al. Exploring reservoir dynamics: a case study of rabies in the Serengeti ecosystem. J Appl Ecol. 2008;45(4):1246-1257. PubMed | Google Scholar
- Changalucha J, Steenson R, Grieve E, Cleaveland S, Lembo T, Lushasi K et al. The need to improve access to rabies post-exposure vaccines: Lessons from Tanzania. Vaccine. 2019 Oct 3;37 Suppl 1(Suppl 1):A45-A53. PubMed | Google Scholar
- Mbwa-Wa-Africa. The national rabies control strategy. Accessed June 19, 2023.
- Diallo MK, Dicko A, Richard V, Espié E. Human rabies post exposure prophylaxis at the Pasteur Institute of Dakar, Senegal: trends and risk factors. BMC Infect Dis. 2019;(191). PubMed | Google Scholar
- Sengson S, Faye R. Factors affecting compliance to rabies post-exposure prophylaxis among pediatric patients seen at the research institute for tropical medicine. PIDSP J. 2013;14(2). Google Scholar
- Chuchu VM, Mutono N, Bichanga P, Kitala PM, Ksee D, Muturi M et al. Effect of phone text message reminders on compliance with rabies post-exposure prophylaxis following dog-bites in rural Kenya. Vaccines (Basel). 2023 Jun 18;11(6):1112. PubMed | Google Scholar
- Hampson K, Dobson A, Kaare M, Dushoff J, Magoto M, Sindoya E et al. Rabies exposures, post-exposure prophylaxis and deaths in a region of endemic canine rabies. PLoS Negl Trop Dis. 2008;2(11):e339. PubMed | Google Scholar
- WHO. Zero rabies by 30, the global strategic plan. 2018. Accessed June 19, 2023.
- Kish L. Survey sampling. new york: John Wesley & sons. Am Polit Sci Rev. 1965;59(4):1025. Google Scholar
- Joseph J, Sangeetha N, Khan AM, Rajoura OP. Determinants of delay in initiating post-exposure prophylaxis for rabies prevention among animal bite cases: hospital based study. Vaccine. 2013;32(1):74-77. PubMed | Google Scholar
- Shrestha B, Dunn L. The declaration of Helsinki on medical research involving human subjects: a review of seventh revision. J Nepal Health Res Counc. 2020 Jan 21;17(4):548-552. PubMed | Google Scholar
- Wu X, Li J, Zhou L, Chen J, Jin Z, Meng Q et al. A Randomized, Double-Blind, Controlled Phase III Clinical Trial to Evaluate the Immunogenicity and Safety of a Lyophilized Human Rabies Vaccine (Vero Cells) in Healthy Participants Aged 10-60 Years Following Essen and Zagreb Vaccination Procedures. Vaccines (Basel). 2023 Aug 1;11(8):1311. PubMed | Google Scholar
- Culp RH. Adolescent girls and outdoor recreation: A case study examining constraints and effective programming. J Leis Res.1998;30(3):356-379. Google Scholar
- Esmaeilzadeh F, Rajabi A, Vahedi S, Shamsadiny M, Ghelichi Ghojogh M, Hatam N. Epidemiology of Animal Bites and Factors Associated With Delays in Initiating Post-exposure Prophylaxis for Rabies Prevention Among Animal Bite Cases?: A Population-based Study. J Prev Med Public Health. 2017;50(3):210-216. PubMed | Google Scholar
- Stodolska M, Shinew KJ, Li MZ. Recreation participation patterns and physical activity among Latino visitors to three urban outdoor recreation environments. Journal of Park and Recreation Administration. 2010;28(2). Google Scholar
- Guadu T, Shite A, Chanie M, Bogale B, Fentahun T. Assessment of knowledge, attitude and practices about rabies and associated factors: in the case of Bahir Dar town. Glob Vet. 2014;13(3):348-354. PubMed | Google Scholar
- Hossain M, Ahmed K, Bulbul T, Hossain S, Rahman A, Biswas MN et al. Human rabies in rural Bangladesh. Epidemiology & Infection. 2012 Nov;140(11):1964-71. PubMed | Google Scholar
- Naing NN. Determination of sample size. Malaysian J Med Sci. 2003;10(2):84-86. PubMed | Google Scholar
- Doege T, Northrop R. Evidence for inapparent rabies infection. Lancet.1974;304(7884):826-829. PubMed | Google Scholar
- Lobo D, DeBenedet C, Fehlner-Gardiner C, Nadin-Davis S, Anderson M, Buchanan T et al. Emergency Response: Raccoon rabies outbreak in Hamilton, Ontario: A progress report. Canada Commun Dis Rep. 2018;44(5):116. PubMed | Google Scholar
- Maki J, Guiot AL, Aubert M, Brochier B, Cliquet F, Hanlon CA et al. Oral vaccination of wildlife using a vaccinia-rabies-glycoprotein recombinant virus vaccine (RABORAL V-RG�): a global review. Vet Res. 2017 Sep 22;48(1):57. PubMed | Google Scholar
- Rocha SM, De Oliveira SV, Heinemann MB, Gonçalves VSP. Epidemiological profile of wild rabies in Brazil (2002-2012). Transbound. Emerg. Dis. 2017;64(2):624-633. PubMed | Google Scholar
- Tiwari HK, Vanak AT, Dea MO, Robertson ID. Knowledge, attitudes and practices towards dog-bite related rabies in para-medical staff at rural primary health centres in Baramati, western India. PLoS One. 2018 Nov 16;13(11):e0207025. PubMed | Google Scholar
- Slater MR. The role of veterinary epidemiology in the study of free-roaming dogs and cats. Prev Vet Med. 2001;48(4):273-286. PubMed | Google Scholar
- Eccles J. Gendered educational and occupational choices: Applying the Eccles et al. model of achievement-related choices,” Int J Behav Dev. 2011;35(3):195-201. Google Scholar
- Singh BB, Kaur R, Gill GS, Gill JPS, Soni RK, Aulakh RS. Knowledge, attitude and practices relating to zoonotic diseases among livestock farmers in Punjab, India. Acta Trop. 2019 Jan;189:15-21. PubMed | Google Scholar
- Kissinga HD. Assessment of knowledge and practice towards rabies and determinants of dog rabies vaccination in Sumbawanga municipality. Muhimbili University of Health and Allied Sciences. 2019. Google Scholar
- Kenko DBN, Mekone AE, Ekaineck JM. Trends in poisoning and bites among patients referred to the Limbe Regional Hospital, South-West Cameroon. Eur Sci J. 2021;17:104-120. PubMed | Google Scholar
- Elelu N, Aiyedun JO, Mohammed IG, Oludairo OO, Odetokun IA, Mohammed KM et al. Neglected zoonotic diseases in Nigeria: Role of the public health veterinarian. Pan Afr Med J. 2019;32(1). PubMed | Google Scholar
- Omodo M, Ar Gouilh M, Mwiine FN, Okurut ARA, Nantima N, Namatovu A et al. Rabies in Uganda: rabies knowledge, attitude and practice and molecular characterization of circulating virus strains. BMC Infect Dis. 2020;20:1-12. PubMed | Google Scholar