Addressing the health workforce gap to achieve the Universal Health Coverage and "The Africa We Want"
Estelle Onyekachi Mbadiwe, Maryam Abdulkarim, Bonheur Dounebaine, Ntuba Mboe Ngange, Kenneth Chukwuebuka Egwu
Corresponding author: Estelle Onyekachi Mbadiwe, Department of Research and Analysis, Ducit Blue Foundation, Abuja, Nigeria 
Received: 01 Mar 2024 - Accepted: 31 Mar 2024 - Published: 03 Apr 2024
Domain: Health system development, Health policy
Keywords: Universal health coverage, health workforce, sustainable development goals, COVID-19
©Estelle Onyekachi Mbadiwe et al. PAMJ-One Health (ISSN: 2707-2800). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Estelle Onyekachi Mbadiwe et al. Addressing the health workforce gap to achieve the Universal Health Coverage and "The Africa We Want". PAMJ-One Health. 2024;13:9. [doi: 10.11604/pamj-oh.2024.13.9.43014]
Available online at: https://www.one-health.panafrican-med-journal.com/content/article/13/9/full
Essay 
Addressing the health workforce gap to achieve the Universal Health Coverage and "The Africa We Want"
Addressing the health workforce gap to achieve the Universal Health Coverage and "The Africa We Want"
Estelle Onyekachi Mbadiwe1,&, Maryam Abdulkarim1, Bonheur Dounebaine2, ![]() Ntuba Mboe Ngange1,
Ntuba Mboe Ngange1, ![]() Kenneth Chukwuebuka Egwu1
Kenneth Chukwuebuka Egwu1
&Corresponding author
African countries face numerous obstacles to achieving Universal Health Coverage (UHC). However, the continent has demonstrated a significant commitment to UHC, evident in the cornerstone incorporation of health in the African Union Agenda 2063. The existing health workforce is insufficient and confronts various challenges as exposed by the COVID-19 pandemic prompting dedication to bolster its capacity. To achieve this goal, innovative strategies should be implemented, including the introduction of new policies and interventions to motivate health workers, encourage collaboration, and enhance production and retention rates. Which, in turn, contributes to achieving UHC and Sustainable Development Goal 3. This paper explores the challenges stemming from the health workforce in Africa concerning the pursuit of UHC and provides key recommendations for capacity enhancement on the continent.
The attainment of Universal Health Coverage (UHC) by 2030 is imperative to fulfilling the Sustainable Development Goal (SDG) 3 which focuses on ensuring healthy lives and promoting well-being for all. This necessitates African nations establishing resilient and effective healthcare systems that grant the public access to essential medical services [1]. However, this ambitious goal remains a herculean task for many African nations, whose healthcare sectors face a myriad of challenges. Addressing these challenges requires an in-depth understanding of issues peculiar to health systems in Africa, which is requisite for identifying areas in need of enhancement. Standard healthcare delivery hinges upon the availability, accessibility, acceptance, and quality of services. Similarly, key constituents of robust healthcare systems encompass the equitable distribution of proficient health workers who have access to essential infrastructure for providing top-notch and culturally sensitive care [2]. This strategy aligns with the African Union's (AU) Agenda 2063, commonly referred to as "The Africa We Want" which prioritizes health as the central pillar of sustainable development across nations [3]. In addition, the “New Public Health Order for Africa” launched by the Africa Centers for Disease Control and Prevention (Africa CDC) stands as the roadmap to sustain health outcomes and health security on the continent, one of its pillars is to support the development of the health workforce [4].
Although there have been some strides towards establishing a resilient and robust healthcare system in Africa, substantial progress is lacking in terms of ensuring an adequate and fair distribution of healthcare workers regionally and nationally. The 77th UN Assembly, with the participation of the AU and the Africa CDC, highlighted the critical shortage of healthcare workers in Africa, projected to reach 6.1 million by 2030 [5]. To tackle this scarcity challenge, they discussed and reported the collaborative effort of the heads of state and Government to increase investment in the development of the health workforce in Africa that would redefine and build a fit-for-purpose health workforce, invest in the female health workforce, increase domestic financing and private sector engagement, transform and strengthen monitoring, evaluation, as well as learning for the health workforce [5].
However, concerns remain if this approach will effectively address the underlying issue. Simply increasing the number of recruits might not suffice if the fundamental problem remains unaddressed. Thus, it is imperative to identify the root causes of this scarcity. Acquiring this knowledge is vital so that stakeholders and policy makers can efficiently direct their efforts toward addressing the fundamental causes of the issue. Appreciating the urgency of this solution hinges on comprehending the seriousness of the problem at hand. This evaluation aims to capture the dynamic shifts and fluctuations of the healthcare workforce's status and composition, considering both positive and negative trends.
Assessing health workforce variations in Africa: prior to the emergence of the COVID-19 pandemic, Africa was not making satisfactory progress towards attaining the health-related SDG objectives. The pandemic exacerbated this setback by pushing the continent even farther from achieving the SDG targets. Nonetheless, the pandemic shed light on the critical significance and influence of the workforce responsible for essential public health duties. This aspect had largely been disregarded or underestimated, resulting in inequalities within and among the nations. Additionally, the pandemic revealed fragmented strategies concerning public health workforce advancement in terms of policies, planning, execution, and assessment [6]. According to the National Health Workforce Data Portal for Africa, there was an increase (from 4 in 2014, to 5 in 2016) in the availability of health workforce professionals (such as Medical Doctors, Nurses, Pharmacists, Dentists, and Midwives) per 10,000 population before the COVID-19 pandemic (i.e. prior to 2019). However, the COVID-19 era reduced the available workforce (3 health professionals in 2019 and 2020), followed by a further decline after 2020 (2 health professionals in 2021) Figure 1.
These declines were exacerbated by the adverse effects of the pandemic on the continent and the healthcare system [7]. In addition to assessing the African health workforce across the periods pre-COVID, during COVID, and post-COVID, it is crucial to make a comparison between Africa and other continents. In 2020, Africa exhibited the lowest doctor-to-population ratio among regions, boasting just 2.9 non-specialist physicians per 10,000 individuals. This density was markedly more than twelve times lower than that of Europe, which boasted 36.6 doctors per 10,000 people [8]. Furthermore, when compared to regions such as Southeast Asia, the Eastern Mediterranean, the Western Pacific, Region of the Americas, and the European Region, Africa has a substantially lower density of medical doctors, nurses and midwives, dentists, and pharmacists, indicating a serious deficiency in the available healthcare workforce (Figure 2).
This scarcity of healthcare professionals per 10,000 population highlights the need for focused efforts and interventions to address the workforce shortage and ensure adequate healthcare provision across the African continent [9]. The variation of health workers density is also glaring within the region. Specifically, in 2021, the regional density of doctors, nurses, pharmacists, and midwives was at 2.11 per 10,000 people. However, certain countries exhibited appreciable densities in 2021, with Nigeria, Zambia, and South Africa surpassing 4.45 health workers (physicians, nurses, pharmacists, and midwives) at 5.02, 5.76, and 5.50 per 10,000 people. Meanwhile, Burundi, Guinea-Bissau, Kenya, and Mozambique maintained a 1-3 health worker ratio per 10,000 people. On the other end of the spectrum, Malawi, Cameroon, Chad, and Togo reported less than 1.0 health workers per 10,000 people, showing a significant disparity in healthcare resources across the region [7]. There is still a scarcity of health workers in almost all WHO African Member States, notwithstanding efforts made by the countries in the region with the support of other international organizations to grow the workforce [10]. When assessing the concentration of healthcare professionals within individual countries based on the most recent data available between 2014 and 2021, it was apparent that only Mauritius has achieved the WHO-recommended benchmark of 23 health professionals per 10,000 people. Meanwhile, Libya, Seychelles, and Tunisia have exceeded half of this recommended threshold. Countries like Seychelles achieved this through strategies like process reengineering, performance management, initiatives for staff retention and motivation, and maximizing the skills available, in both the public and private sectors [11].
There is a growing acknowledgment of the significance of community healthcare workers (CHW) in reinforcing health systems and addressing the void caused by the departure and inadequate production of healthcare professionals [12]. According to a UN article, there are 3,000 Community Health Workers in Mali and more than a million across sub-Saharan Africa, all working to reduce barriers to healthcare [13]. Many countries are making CHWs a cornerstone for healthcare delivery in the community setting in order to achieve UHC [14]. For example, the Ethiopian health extension program is being optimized by connecting the Women's Development Army with Health Extension Workers [15], Kenya´s sub-national parliaments have passed bills to legally recognize and regulate community health services as part of a new strategy [16] and Zambia has a new strategic plan that outlines the costs of expanding to 5000 Community Health Assistants [17]. Although these examples showcase tremendous progress in institutionalizing community health workers, most countries have yet to establish nationally coordinated and fully operational community health strategies [17]. Nevertheless, the role of CHWs is expanding to allow more skilled personnel to devote more time to more advanced duties. The capacity for CHWs to strengthen and close the gap of the undermanned health workforce is so plausible that the integration of this system into the healthcare system of developed nations is encouraged [18]. The glaring imbalance among African countries underscores the pressing need for targeted interventions and collaborative initiatives to rectify the uneven healthcare landscape on the continent and ensure equitable access to healthcare services for all. Recognizing the urgency of addressing these disparities, it is crucial to turn our attention to the challenges that have contributed to this uneven distribution of healthcare resources.
Challenges affecting the health workforce in the African region
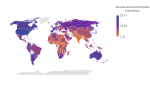
Underfunding of the healthcare system: funding significantly influences the health workforce by directly impacting its composition, capacity, and performance. Africa has consistently grappled with a significant lack of investment in the education and training of health workers, notably falling below the established threshold of approximately 23 health workers per 10,000 population [19]. A well-funded healthcare system can attract and retain skilled professionals through competitive salaries, training opportunities, and career development prospects. Adequate funding also supports the recruitment of additional staff to address shortages, therefore, enhancing the overall workforce density. A study conducted in 20 East and Southern African nations revealed that even small increases in government health spending and higher funding priorities for the health workforce, similar to the 57% global average, can increase the fiscal space for the health workforce by at least 32% in 11 nations [20]. Unlike other continents, where a substantial share (above 15%) of general government expenditure goes towards the healthcare system, ensuring satisfactory wages and salaries for healthcare workers, Africa's healthcare professionals encounter difficulties due to the notably meager allocation of government funds to healthcare. Only South Africa met and exceeded this benchmark, reserving 15.29% of their annual budget for the health sector in 2020 (Figure 3) [21]. This underfunding factor potentially contributes to the migration of healthcare workers to other continents in search of more favorable employment prospects, a phenomenon often referred to as "Japa" [21]. This contrasts with the pledge of the heads of state of African Union member countries in 2001 in Abuja to allocate a minimum of 15% of their national budget to healthcare during the Abuja Declaration [22].
Effects of the COVID-19 pandemic on the health workforce: the pandemic underscored the crucial need for a skilled and motivated workforce, while impeding progress worldwide in addressing existing gaps. According to WHO projections, between January and May 2021, the COVID-19 pandemic may have claimed the lives of up to 180,000 health and service workers [23]. Furthermore, a study conducted in Nigeria in 2021 sheds light on the absence of adequate support for healthcare workers during the pandemic [24]. This lack of support had a profound impact on the mental well-being of these professionals, consequently influencing the quality of care provided to patients. Other issues like burnout arising from the psychological strain faced by healthcare workers, which in turn contributed to a reduction in the available workforce, have been highlighted by some studies in Africa.
Brain drain: the continent faces a concerning trend: a brain drain of locally-trained health workers to developed countries, which puts pressure on its healthcare systems. This phenomenon has inflicted damage on the quality of health services in sub-Saharan Africa, as these healthcare professionals play an indispensable role in improving health outcomes. Approximately 80% of African countries are experiencing medical staff shortages and high rates of healthcare professionals leaving to work abroad. To put this into perspective, Nigeria alone witnessed the departure of 9,000 doctors to the UK, Canada, and the United States between 2016 and 2018 [25]. Adding to the concern, a UK government report in August 2022 disclosed that a staggering 13,609 healthcare workers left Nigeria for the UK in 2021, further emphasizing the scale of this issue [26]. A comprehensive study conducted in 2023 illuminated that in Africa, the principal driving forces behind this brain drain encompass factors such as job insecurity, inadequate infrastructure, subpar remuneration, lack of personal autonomy, and economic instability. Insecurity and elevated crime rates in countries like South Africa and Nigeria also amplify the inclination for migration [27].
An unsettling scenario emerged during the height of the COVID-19 pandemic, as highlighted by a 2021 report. Zimbabwe and several other nations witnessed a significant exodus of medical experts, with over 2,200 of them relocating to work in the US, the UK, and Australia. This number exceeded the prior year's count, thereby straining the already fragile healthcare systems [28]. While instances of migration of African health professionals outside the continent are well-documented, a study revealed that brain drain also occurs intra-continentally, with African professionals moving from their countries of origin to other African nations such as Botswana and South Africa. As nations across various socioeconomic strata grapple with the challenges of training, employing, deploying, retaining, and optimizing their health workforce, it is undeniable that brain drain significantly contributes to the WHO's projected shortage of 10 million health workers by 2030.
Advancing health workforce capacity in Africa: recent developments and insights
Prioritise students with a rural background in health workforce training: the WHO has advocated for targeted admission policies that prioritize students with a rural background in health worker (HWs) training programs. This strategy aims to enhance the development, attractiveness, recruitment, and retention of HWs in rural and remote areas. Recently, this approach has gained significant attention due to its effectiveness in increasing the availability of health personnel in challenging locations like rural and underdeveloped communities. It has resulted in more rural health practitioners, improved communication between healthcare providers and community members, and positive changes in household economic and social conditions, especially for students from low-income families. Moreover, it has led to improved quality of health services, enhanced health education and promotion within rural communities, and increased motivation among community members to pursue careers in healthcare. By embracing such strategies, Africa can envision a brighter future for its health workforce and overall healthcare landscape.
Maximise investments in the healthcare systems: over time, investments in the health workforce have brought about some changes, yet they continue to be significantly insufficient to bridge the existing disparities. All African countries were urged to sign the Abuja declaration to give precedence to investing in public health. This accord stemmed from the increasing recognition that the progress of the continent in terms of human, political, and economic development hinges on the well-being of its population [29]. Foreign aid has also been a significant but not a definite intervention to strengthen the health workforce in Africa. This is highlighted by examples such as the Department of Health and Social Care of the United Kingdom in June 2023 making a fresh funding commitment of £2 million to support Ghana, Nigeria, and Kenya in developing their health workforce to achieve universal health coverage. While deliberate efforts have been made by foreign countries and international organizations to push funds to the health sector in African countries, it is imperative to address the underlying issue of limited investment share. This necessitates proactive steps to increase the allocation of the national budget towards healthcare.
Investment in training and monitoring knowledge transfer: strengthening health workforce capacity demands substantial investments in education and training, robust monitoring systems would ensure that the knowledge gained during training is effectively implemented in real-world scenarios.
Prioritisation of retention: there is a grave need to address the brain drain that has plagued our continent for far too long. Adequate incentives, career growth opportunities, and supportive working environments are essential in retaining our brightest minds within Africa. The government must demonstrate a strong commitment to enhancing the quality of work and life for healthcare professionals, thereby encouraging their retention.
Embracing innovation and technology: the trajectory of healthcare is intrinsically linked with technology and innovation. The symbiotic relationship between telemedicine and data-driven decision-making carries the potential to surpass obstacles and elevate healthcare access, quality, and efficiency. As we traverse this ever-evolving terrain, it becomes paramount to equip our healthcare professionals with the competencies required to adeptly navigate and leverage these tools. This strategic empowerment ensures that these advancements not only improve patient care but also empower healthcare providers to remain at the forefront of innovative practices, fostering a healthcare landscape that is both transformational and responsive to the dynamic needs of our societies.
Foster collaboration through Africa CDC leadership: the endeavor to construct a resilient healthcare workforce is an endeavor that demands the collective engagement of various stakeholders. Governments, Non-Governmental Organisations (NGOs), academia, and the private sector must converge, pooling their resources, knowledge, and insights to forge enduring transformations. Africa CDC as the autonomous and technical institution of the African Union is mandated to support member states to strengthen their public health workforce. As part of actions to fulfill this mandate, Africa CDC needs to take leadership in making policies encouraging health worker expansion and retention at the national and continental levels. This collaboration extends beyond domestic borders and assumes a global dimension, particularly in the context of attracting the diaspora. While recruiting new individuals might necessitate investing in training, a more sustainable approach involves tapping into the expertise of the diaspora. Collaborative efforts to create a welcoming environment for those abroad to return to their home countries become vital. By enhancing conditions and opportunities, we not only encourage repatriation but also reinforce the commitment to retain these valuable contributors within the local healthcare landscape. This collective strategy exemplifies the proactive path forward, one that capitalises on collaboration to shape a brighter future for healthcare across the continent.
Empower youths: African youths represent our most valuable resource. By providing them with the guidance, skills, and opportunities they need to thrive, we pave the way for a healthcare landscape that is innovative, equitable, and responsive to the evolving needs of our communities. This investment is not merely an act of support; it's a deliberate choice to unlock the potential that resides within the next wave of healthcare leaders. These imperative call-to-action measures not only shed light on the critical interplay between economic circumstances and healthcare workforce challenges in Africa but also provide a roadmap for informed decision-making by policymakers and stakeholders. Healthcare transformation of this magnitude requires a concerted effort from governments, international organizations, and public and private healthcare institutions, including the NGOs, educational bodies, community leaders, healthcare workers themselves, and every single African citizen. By embracing these actions, nations can steer their healthcare systems toward a trajectory of growth and resilience, ensuring that the scarcity of healthcare professionals and related issues are effectively addressed.
The right to quality healthcare relies on accessible, available, and skilled health workers, and yet Africa faces persistent challenges in this regard. Despite some progress, the continent still grapples with brain drain, underfunding, and the pandemic's impact on the workforce. There is a need to make policies in areas such as domestic healthcare funding, healthcare worker migration, prioritizing rural backgrounds in health worker education and training; and increasing investments in developing the health workforce; the collaboration of governments, international organizations, and stakeholders is vital to addressing these disparities and ensuring equitable access to healthcare; strategies centering on education, retention, policy development, incentives, and technological innovation will contribute to a stronger and more resilient health workforce in Africa. However, as we navigate the challenges by taking proactive measures and prioritizing the health workforce, Africa can pave the way for improved healthcare access and outcomes for its population, to not only achieve UHC but make progress in line with the AU Agenda 2063 for advancing health for “The Africa we want”.
The authors declare no competing interests.
Essay conception and design: Estelle Onyekachi Mbadiwe, Bonheur Dounebaine, Kenneth Chukwuebuka Egwu, Maryam Abdulkarim and Ntuba Mboe Ngange. Essay writing was done by Estelle Onyekachi Mbadiwe, Bonheur Dounebaine, Kenneth Chukwuebuka Egwu, Maryam Abdulkarim and Ntuba Mboe Ngange. Manuscript preparation: Estelle Onyekachi Mbadiwe, Bonheur Dounebaine, Maryam Abdulkarim, Kenneth Chukwuebuka Egwu and Ntuba Mboe Ngange. The authors reviewed and approved the final version of the manuscript.
We would like to extend our heartfelt appreciation to Nancy Amandi for their invaluable contributions to the data verification process. Their meticulous efforts ensured the scientific accuracy and reliability of this essay. Additionally, we are grateful to Nonso Vincent for their assistance in designing the manuscript figures, which greatly enhanced the understanding of the discussion. We are also indebted to the support staff and administrators of the Ducit Blue Team who facilitated the smooth operation of our research activities. We are immensely grateful to all the individuals who contributed to this essay. Their dedication, expertise, and unwavering support have been instrumental in the completion of this article. Without their invaluable contributions, this essay would not have been possible.
Figure 1: density of health professionals per 10,000 population in Africa 2014-2021; data source: national health workforce accounts data portal (2014 - 2021)
Figure 2: global density of selected health professionals per 10,000 population, in the WHO regions 2014-2021; data source: world health statistics, 2023
Figure 3: global map on the distribution of percentage government healthcare expenditure (2011 - 2021); data source: global health system financing database by world health organization, 2023
- Okoroafor SC, Ahmat A, Asamani JA, Millogo JJS, Nyoni J. An Overview of Health Workforce Education and Accreditation in Africa: Implications for Scaling-up Capacity and Quality. Hum Resour Health. 2022 May 7;20(1):37. PubMed | Google Scholar
- Kunjumen T, Okech M, Diallo K, Mcquide P, Zapata T, Campbell J. Global experiences in health workforce policy, planning and management using the Workload Indicators of Staffing Need (WISN) method, and way forward. Hum Resour Health. 2022 Jan 28;19(Suppl 1):152. PubMed | Google Scholar
- Africa CDC. Ministerial meeting on strengthening community health workforce, systems and programmes In Africa. Africa CDC. 2023. Accessed Jun 7, 2023.
- Africa Centres for Disease Control and Prevention. Call to Action: Africa´s New Public Health Order. Africa CDC. 2023. Accessed Jun 7, 2023.
- Africa CDC. COMMUNIQUE: “Reimagining Health Workforce Development for Africa´s Health Security”. Africa CDC. 2022 Accessed Jul 21, 2023.
- African Region WHO. Enabling Sustainable Health Workforce Investments for Universal Health Coverage and Health Security for the Africa We Want. 2023. Accessed Aug 12, 2023.
- World Health Organization. Welcome National Health Workforce Accounts Data Web portal. Accessed Aug 14, 2023.
- ReliefWeb. Atlas of African Health Statistics 2022: Health situation analysis of the WHO African Region. 2022. Accessed Aug 14, 2023.
- World Health Organization. World Health Statistics. 2021. Accessed Aug 14, 2023.
- Ahmat A, Okoroafor SC, Kazanga I, Asamani JA, Millogo JJS, Illou MMA et al. The health workforce status in the WHO African Region: findings of a cross-sectional study. BMJ Global Health. 2022 May;7(Suppl 1):e008317. PubMed | Google Scholar
- World Health Organization. WHO country cooperation strategy at a glance: Seychelles. 2018. Accessed Aug 21, 2023.
- Johnson LJ, Schopp LH, Waggie F, Frantz JM. Challenges experienced by community health workers and their motivation to attend a self-management programme. Afr J Prim Health Care Fam Med. 2022 Jan 12;14(1):e1-e9. PubMed | Google Scholar
- Africa Renewal. Community Health Workers: The Unsung Heroes in Africa's COVID-19 response. 2021. Accessed Aug 21, 2023.
- Singh P, Sachs JD. 1 million community health workers in sub-Saharan Africa by 2015. Lancet. 2013 Jul 27;382(9889):363-5. PubMed | Google Scholar
- Community Health Roadmap. Community Health Roadmap. 2021. Accessed Aug 21, 2023.
- Hussein S, Otiso L, Kimani M, Olago A, Wanyungu J, Kavoo D et al. Institutionalizing Community Health Services in Kenya: A Policy and Practice Journey. Global Health: Science and Practice. 2021 Mar 15;9(Suppl 1):S25-31. PubMed | Google Scholar
- Leydon N, Kureshy N, Dini HS, Nefdt R. Country-led institutionalization of community health within primary health care: Reflections from a global partnership. J Glob Health. 2021 Mar 1;11:03037. PubMed | Google Scholar
- Mishra SR, Neupane D, Preen D, Kallestrup P, Perry HB. Mitigation of non-communicable diseases in developing countries with community health workers. Global Health. 2015 Nov 10;11:43. PubMed | Google Scholar
- Ahmat A, Asamani JA, Abdou Illou MM, Millogo JJS, Okoroafor SC, Nabyonga-Orem J et al. Estimating the threshold of health workforce densities towards universal health coverage in Africa. BMJ Glob Health. 2022 May;7(Suppl 1):e008310. PubMed | Google Scholar
- Asamani JA, Kigozi J, Sikapande B, Christmals CD, Okoroafor SC, Ismaila H et al. Investing in the health workforce: fiscal space analysis of 20 countries in East and Southern Africa, 2021-2026. BMJ Glob Health. 2022 Jun;7(Suppl 1):e008416. PubMed | Google Scholar
- World Health Organization. Health Financing. Accessed Aug 21, 2023.
- World Health Organization. The Abuja Declaration: Ten Years On 2001 Promises of commitment and solidarity. 2010. Accessed Aug 21, 2023.
- World Health Organization. The Impact of COVID-19 on Health and Care workers: a Closer Look at Deaths. 2021. Accessed Aug 21, 2023.
- Okediran JO, Ilesanmi OS, Fetuga AA, Onoh I, Afolabi AA, Ogunbode O et al. The experiences of healthcare workers during the COVID-19 crisis in Lagos, Nigeria: A qualitative study. GERMS. 2020 Dec:10(4):356-66. PubMed | Google Scholar
- Green MA, Murrin C. Africa´s Healthworker Brain Drain | Wilson Center . 2023. Accessed Jul 24, 2023.
- Lawal L, Lawal AO, Amosu OP, Muhammad-Olodo AO, Abdulrasheed N, Abdullah KR et al. The COVID-19 pandemic and health workforce brain drain in Nigeria. Int J Equity Health. 2022 Dec 5;21(1):174. PubMed | Google Scholar
- World Health Organization. Health workforce. Accessed Jul 1, 2023.
- AfricaNews. Zimbabwe hit by exodus of health professionals. 2021. Accessed Jul 24, 2023.
- SAIIA. SADC and the Abuja Declaration: Honouring the Pledge. 2021. Accessed Jul 24, 2023.