Willingness to accept indoor residual spraying (IRS) for malaria prevention and associated factors in Southwest Ethiopia
Kamil Mohammed, Angesom Weldu, Bayu Begashaw Bekele
Corresponding author: Bayu Begashaw Bekele, Division of Public Health Sciences, Department of Surgery, Washington University School of Medicine, St. Louis, MO, USA 
Received: 02 Feb 2024 - Accepted: 16 Apr 2024 - Published: 25 Apr 2024
Domain: Entomology, Community health, Malaria control program
Keywords: Indoor residual spraying, public health, malaria elimination, Ethiopia
©Kamil Mohammed et al. PAMJ-One Health (ISSN: 2707-2800). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Kamil Mohammed et al. Willingness to accept indoor residual spraying (IRS) for malaria prevention and associated factors in Southwest Ethiopia. PAMJ-One Health. 2024;13:18. [doi: 10.11604/pamj-oh.2024.13.18.42850]
Available online at: https://www.one-health.panafrican-med-journal.com/content/article/13/18/full
Research 
Willingness to accept indoor residual spraying (IRS) for malaria prevention and associated factors in Southwest Ethiopia
Willingness to accept indoor residual spraying (IRS) for malaria prevention and associated factors in Southwest Ethiopia
&Corresponding author
Introduction: indoor residual spraying (IRS) is still a key vector control intervention for reducing malaria transmission. However, in areas with limited access to health facilities and infrastructure, willingness to accept and determinants have not been adequately evaluated. Hence, this study aimed to investigate households� willingness to accept IRS and associated factors in Bench Sheko zone, Southwest Region of Ethiopia.
Methods: a community-based cross-sectional study was conducted using 589 randomly selected household heads. A multistage sampling technique was used to recruit study participants. A face-to-face data interview was used to collect the data. Multivariate logistic regression was used to identify independent factors of willingness to accept IRS. An adjusted odds ratio with a 95% confidence interval (CI) was used to measure the strength of the association.
Results: the overall household willingness to accept IRS for malaria control was 59.4% (95% CI: 55.3%- 63.3%). Households with secondary school education and above (AOR = 4.4; 95% CI: 2.21-8.53; age ≥35 years, AOR = 3.51; 95% CI: 1.68-7.33; good knowledge about malaria, AOR = 2.28; 95% CI: 1.21-4.26; receiving sensitization program, AOR = 1.91; 95% CI: 1.05- 3.76 favored odds of accepting an IRS while perceived bedbug and flea activation, AOR= 0.44; 95% CI: 0.20-0.97 decreased likelihood of IRS acceptance after controlling for other variables.
Conclusion: the willingness to accept the IRS was moderate and it was driven by sociodemographic and behavioral aspects. Therefore, enhancing targeted community mobilization is crucial for maximizing the uptake and acceptance of the IRS.
In low- and middle-income countries (LMICs), malaria continues to be a major public health threat, causing serious illness and death [1]. Malaria accounted for an estimated 247 million cases and 619,000 related deaths in 2021. Among these, 95% of all malaria cases were attributed to African Region. This made malaria one of the top ten causes of death in LMICs [2,3]. Integrated strategies such as community engagement have helped eliminate and eradicate malaria in different parts of the world [4,5]. For instance, 75 years ago, malaria was a potential public health problem affecting more than 30 million people in China. However, China declared malaria elimination in 2021 [6]. One of the key strategies that helped the country eliminate malaria was active community engagement alongside basic research implementation. A community was actively cooperating and accepting the national public health campaign against malaria and thereby ensuring unfavorable mosquito-spreading areas [7]. Other countries, such as Algeria, Morocco, Kyrgyzstan, and Paraguay, have recently eliminated malaria through organized efforts by communities combined with other preventive strategies against the disease [8]. However, the majority of sub-Saharan African (SSA) countries have been working on malaria elimination by 2030 [9].
Indoor residual spraying (IRS) is a malaria control and prevention activity that involves spraying insecticides on surfaces such as internal walls, roofs, ceilings, and other indoor structures where mosquitoes reside and thereby killed by the residue of the chemical, resulting in a reduction in malaria transmission [10]. It quickly kills mosquitoes while they rest on sprayed surfaces [11]. Studies revealed that the appropriate use of an IRS effectively reduced the biting rate and the resting densities of indoor and outdoor mosquitoes [12-14]. IRS has resulted in effective malarial prevention and control in addition to long-lasting insecticide-treated nets (LLTNs) [15]. For example, it has been shown to significantly reduce malaria parasite infection by 65%, 95% CI (56-73%) [16], and morbidity [4]. The WHO recommends at least 80% IRS coverage among households in malaria-endemic areas. This helps with progress toward global malaria eradication [17], highlighting the importance of the relationship between IRS coverage and effectiveness [6]. Despite IRS paramount benefits, its effectiveness has been affected by several factors [18], which are influenced mainly by households´ acceptance of the IRS [4,19,20]. Globally, acceptance of IRS among households varies across countries. For instance, household IRS acceptance in Zambia was 87% [21], Iran´s acceptance ranged from 98-100% [22], and Ethiopia´s acceptance was 56.5% [23].
Ethiopia accounts for approximately 1.7% of global malarial cases and 1.5% of deaths per year [24]. Three-fourths of the landmasses are favorable for malaria, and seventy percent of the population live at risk of acquiring malaria [25,26]. Subsequently, Ethiopia has been implementing integrated modes of preventing and controlling malaria for prolonged periods. Since 2008, Ethiopia has been implementing IRSs and LLITNs as key vector control interventions [15,27]. According to the 2015 Ethiopian malaria indicator survey, only 29% of households had IRS in 2014 [28]. Nonetheless, among more than 800 districts in the country, only 230 districts are closing to eliminate malaria by 2030 [29]. Evidences support that higher acceptance or willing to accept IRS resulted in malarial risk reduction [21,22]. The study area (Bench Sheko) has been one high malaria burden zones in Ethiopia. So, malaria has been persistent, with a prevalence of 32.7 percent, and an increased incidence in the last five years [1,30]. To our knowledge, there is inadequate evidence and knowledge about households´ willingness to accept an implementation of intervention strategies, mainly IRS and associated factors in the study area. Hence, the objectives of this study are (1) examining the willingness to accept an IRS, and (2) associated factors with willingness to accept IRS among households in the Bench Sheko zone, southwest Ethiopia.
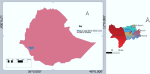
Study design, setting, and period: a community-based cross-sectional study was conducted in Bench Sheko zone, the southwestern region of Ethiopia. The zone is located 561 km southwest of Addis Ababa, which is the capital city of Ethiopia. Based on the population projection values of 2017, this zone has an estimated population of 847,168; of them, 418,213 are females, for an estimated total of 125,069 households. The population is distributed in 45 malaria-endemic kebeles (the smallest administrative unit in Ethiopia) within 5 districts, 20 of which have a history of repeated IRS practices. According to the 2023 Zonal Health Office report (unpublished), there are 1 teaching hospital, 1 primary hospital, 27 health centers, 15 medium clinics, 123 primary clinics, 35 drug stores, 128 health posts, and 5 rural drug stores, for a total of 924 health workers working within the zone. The study was conducted from April 1 to 30, 2023. The study area is illustrated by a map (Figure 1).
Population: the source population was all households located in the study area. Study population: All eligible households in randomly selected malaria kebeles of the Bench Sheko zone.
Eligibility criteria: all household heads who resided for at least six months in the selected kebeles and currently living in their homes were included in the study. Both household heads who had a history and no history of IRS were included in the study. Household heads who were unable to communicate critically ill, or did not have the willingness to respond were excluded from the study.
Sample size determination: the sample size was determined by using the single population proportion formula by assuming that the IRS acceptance rate for malaria prevention in Ethiopia was 56.5% [23], with a 95% CI and a 5% margin of error, yielding a sample size of 378.
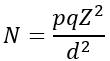
Refer to n was the sample size, p = prevalence of IRS acceptance, q = 1 - p and d = margin of error, a confidence level was assumed to be 95%, and Z was 1.96 with the two-sided test at 95% CI. To adjust for the cluster effect in the design that increases the intraclass correlation (ICC) of the study participants in the selected cluster [31], the calculated sample size is multiplied by the design effect 1.5, and a 10% nonresponse rate is added to yield the final required sample size of 624 households. ICC corresponds to the magnitude of variation in a lack of willingness to accept IRS between Kebeles which ranges from 0 to 1. When the value of ICC gets closer to 1 (but not necessarily 1) shows that there is significant dissimilarity in a lack of willingness to accept IRS across Kebeles and if closer to 0 (not necessarily zero) no difference or variation [32].
Sampling procedure and techniques: a multistage sampling technique was employed. In the first stage, zones were classified into urban and rural districts to randomly select urban (one) and rural (two) districts using a lottery method. Out of 20 kebeles in selected districts, 6 kebeles were selected randomly using the lottery method. In the second stage, all eligible households within the selected kebeles were identified from the family folder in the health post. A family folder is an archive that contains each household name for a specific kebele. Subsequently, the list of all households was used as a sampling frame. Using population proportion sampling (the total sample size was proportionally allocated to the total number of households in each selected kebeles). Finally, 624 households were recruited using systematic random sampling. Finally, to reach a study unit, every kth house was selected from each kebele for the interview.
Variables: the outcome variable was the willingness to accept the IRS. The independent variables were sociodemographic variables (age, sex, marital status, residence, educational status, type of roofing, occupational status), knowledge about malaria, attitude towards IRS, and receiving information (sensitization) about IRS.
Operational definition: the willingness to accept an IRS was measured by the tendency of study participants to use malaria prevention activities, primarily IRS, which is considered appropriate depending on predicted or lived reasoning and sensitive reactions to the intervention [21]. A Likert scale ranging from 0 to four was used to measure acceptance (0, strongly disagree; 1, disagree; 2, neutral; 3, agree; and 4, strongly agree). The highest score was calculated by multiplying the highest scale value by the total number of questions. Accordingly, participants who answered 3 or more questions (? 75%) were considered to have accepted the IRS [33]. Knowledge: to assess participants´ knowledge about IRS, six knowledge measuring questions with yes, and no answers. If the respondent answered less than 3 out of six questions was categorized as poor knowledge, and three and above questions with yes answers were considered to have good knowledge [34,35].
Data collection tools and procedures: the data were collected using a structured interviewer-administered questionnaire by reviewing different studies [21,35,36]. The questionnaire was composed of sociodemographic variables, knowledge about the IRS, knowledge about malaria, and reasons for refusal to use the IRS. Four environmental science graduates collected the data, while two public health officers supervised the data collection process. Sampled household heads and wives who were absent at the time of data collection were revisited for the second time. Those who were absent during the second trial were considered to be nonrespondents.
Data quality control: the questionnaire was developed in English, translated into the Amharic language, and subsequently back-translated to English to ensure its consistency. The data collectors and supervisors received two days of training. A pretest was conducted on 31 households (5%) in the total sample outside the selected kebeles, after which necessary corrections were made. The data collection procedure was closely supervised, and the collected data were checked for completeness, consistency, and reliability.
Data processing and analysis: the data were subsequently entered into Epidata version 4.02 and exported to SPSS version 25 for further analysis. Descriptive statistics such as frequency and percentage for categorical variables and mean and standard deviation for continuous variables were computed. In the bivariate analysis, a crude odds' ratio (OR) at the 95% CI was used to measure the association between variables, and variables with a p-value less than 0.25 were included in the final multivariable model. Model fitness was tested using the Hosmer-Lemeshow goodness-of-fit test, which is nonsignificant, with a p-value of 0.647. Multiple logistic regression was employed to assess the independent predictors of IRS acceptance by controlling for potential confounders. An adjusted odds ratio with a 95% CI was used to determine an independent association between variables. The level of significance was defined as p<0.05.
Ethics approval: the study was conducted after obtaining a letter of ethical permission from Mizan Tepi University College of Medicine and Health, School of Public Health. Permission letters were obtained from the Bench Sheko zone and Woreda health offices. Informed oral consent was obtained from the heads of the households. In addition, the participants´ information was not disclosed to another person or a third party, and the participants were also informed regarding their full right to participate or refusal to participate in the study at any time.
A total of 591 respondents were successfully interviewed, yielding a response rate of 94.7%.
Sociodemographic characteristics of the participants: three hundred thirty-four (56.7%) of the respondents were male, and 347 (58.9%) were currently married. The mean (±SD) age of the study respondents was 36 (±12.2) years, with the majority 342 (58.1%) of the participants aged ≥35 years. Regarding educational status, 188 (31.9%) of the respondents had no formal education. The participants were predominantly protestant religion followers (366, 62.1%), followed by Orthodox (155, 26.3%), and Muslim (68, 11.6%). Approximately 86.1% of the study participants lived in thatch houses, whereas 13.9% lived in corrugated iron sheets (CISs) (Table 1).
Knowledge of study participants about malaria and IRS: five hundred thirty-eight respondents (91.3%) reported that the cause of malaria was mosquito bites. The most frequently reported malaria prevention measure was removing mosquito breeding sites (89.5%), followed by using bed nets (6.4%) and IRS (4.1%), and surprisingly, 22 (3.7%) participants did not know about any prevention mechanism for malaria. In addition, 265 (45%) and 192 (32.6%) of the respondents identified under 5 children and pregnant women as the most high-risk groups, respectively (Table 2). In the present study, nearly three-fourths (72.3%) of the participants had received information about the IRS before it was sprayed by the operator. The majority of the respondents, 495 (84%), reported that the IRS spray timing was appropriate. Among all the surveyed household heads, less than half (44.7%) of the respondents reported an IRS efficacy period on sprayed walls between 3 and 6 months, 117 (19.9%) indicated an efficacy period > 6 months, and the remaining 15 (2.5%) reported an efficacy period < 3 months. In addition, two-thirds of the respondents (67.4%) had not modified their walls after spraying. Moreover, of the respondents who modified their walls after spraying, 120 (62.5%) applied painting, 36 (18.8%) used plastering, 24 (12.4%) applied decoration, and the remaining 12 (6.3%) washed their walls after spraying (Table 3).
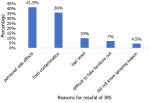
Willingness to accept of IRS: in the present study, the overall household willingness to accept of IRS was 59.42% (95% CI: 55.3-63.3). Three hundred fifty-five (60.3%) of the respondents reported that IRS spraying was beneficial, and 333 (56.5%) respondents reported that IRS could reduce malaria transmission. Nearly half (49.6%) of the respondents were willing to implement the IRS in the future. Approximately 179 (30.4%) of the respondents agreed to take precautions after spraying (Annex 1). The main reasons for IRS refusal reported by the households were perceived side effects, followed by others (Figure 2).
Factors associated with the willingness to accept of IRS: after adjusting for confounding variables in multivariable analysis, variables sex, age, educational status, knowledge about malaria, perceived bed bug production, and sensitization activities were significantly associated with the willingness to accept IRS. Respondents who had good knowledge about malaria were more than two times more likely to be willing to accept IRS than those who had poor knowledge about malaria (AOR= 2.28; 95% CI=1.21-4.26, p=0.01). Respondents older than 35 years were four times more likely to have a willingness to accept the IRS than their counterparts (AOR= 3.51; 95% CI=1.68-7.33). Participants who received sensitization activities were two times more likely to have a willingness to accept IRS than participants who did not receive sensitization activities (AOR= 1.91; 95% CI=1.05-3.76). Additionally, respondents who had completed high school and above were more than four times more likely to be willing to accept the IRS than respondents who did not attend formal education (AOR= 4.4; 95% CI= 2.21-8.53). A total of 56% of participants who perceived the IRS to be able to produce bedbugs/fleas were less likely to be willing to accept the IRS than their male counterparts (AOR= 0.44; 95% CI=0.20-0.97) (Table 4).
Due to recurrent malaria epidemics resulting in increased susceptibility, this study was conducted to investigate household acceptance of indoor residual spray and its determinant factors in the Southwest Ethiopian People´s Region. This study revealed that four out of ten households did not have willingness to accept IRS. This finding is consistent with a study conducted in the central part of Ethiopia [37]. This status was found to be unsatisfactory to achieve the WHO recommendation and Ethiopia's malaria elimination strategic plan 2021-2025, which targeted IRS coverage >80% for effective malaria elimination [8,38]. In addition, this study showed considerably lower acceptance than did reports from previous studies conducted in Iran (98-100%) [22], and other sub-Saharan countries like Nigeria (82.6%) [39], Uganda (79.9%) [40], and Rwanda (73.9%) [41]. This variation could be attributed to unstudied contextual factors, specifically cultural differences.
On the other hand, the current status of willingness to accept IRS was higher than elsewhere Keresa, Ethiopia (27.8%) [42] and Assam, India (47.8%) [43]. The variation could be due to the study participants and culture, respectively, in those studies. Perceived side effects were a primary reason for the lower acceptance of IRS spraying. This finding is consistent with previous reports [23,36,41] in which respondents feared the health side effects of spraying. The misperception has been a long-term threat to effective malaria prevention strategies, as highlighted by other studies [44,45]. Therefore, addressing community concerns and doubts regarding the side effects of the IRS through a community sensitization campaign is crucial for further enhancing IRS acceptance and resulting reduction in malaria incidence. Notably, the role of the IRS operator in addressing the fears and misperceptions of the IRS is necessary to ensure prompt responsiveness to community needs and increase the acceptance of interventions. A higher educational level favored the willingness to accept IRS. Participants who had completed secondary education or above were more likely to accept an IRS than participants who had no formal education. This finding is consistent with studies conducted elsewhere [45,46]. A plausible explanation could be that participants with higher education levels are expected to have more knowledge and be able to utilize malaria prevention methods effectively. Similarly, previous studies supported this finding by claiming that higher education levels are associated with good knowledge of malaria prevention [35,47]
Older respondents were more likely to have a willingness to accept the IRS than their counterparts. This finding is similar to that of other studies [36,48]. This might be due to a sense of responsibility for oneself and household members, and past experiences. Moreover, this study showed that the odds of willingness to accept IRS increase among respondents who have good knowledge about malaria. This evidence was comparable with that of other previous reports [23,39,49]. This reinforces the notion that a better understanding of a given health issue enables people to improve their health by implementing preventive measures [35]. It is also clear that as their knowledge level increases, individuals tend to attend health education campaigns and follow mass media such as radio and television. This may create an opportunity to gain well-articulated information to increase the willingness to accept IRS. To improve IRS acceptance, a comprehensive approach that targets people through community mobilization, communication, and advocacy for malaria elimination is required.
Strengths and limitations of the study: as a community-based study, this approach is strong enough to produce real evidence. However, our study is not immune to limitations. The first limitation is that because of the use of cross-sectional study designs, examining the causal relationships is difficult. Another potential drawback could be that social desirability bias and recall bias could lead to an overestimation or underestimation of the acceptance of the IRS. Moreover, we did not measure the combined availability of long-lasting insecticide-treated bed nets among the study participants because it is related to the acceptance of the IRS.
The level of willingness to accept IRS for malaria control in the study area was relatively low compared to the target of the WHO and the Federal Ministry of Health for malaria control. Therefore, enhancing targeted community mobilization and sensitization in malaria-endemic areas through the continuous provision of health education is crucial for promoting the acceptance of the IRS. Additionally, clear communication with the community about the effectiveness of the IRS and its ability to reduce malaria transmission may help support IRS acceptance. The type of chemical used to eliminate mosquitos is unknown to households, which may impact their willingness to accept IRS.
What is known about this topic
- According to the World Health Organization, indoor residual spraying has been one of the most important intervention strategies for malaria elimination by 2030 in developing countries;
- Community participation and behavioral change play an integral role in implementing malaria elimination strategies.
What this study adds
- More than 40% of study participants were unwilling to accept the IRS;
- The majority of patients (41.5 percent) had refused IRS due to concerns about its side effects;
- Willingness to accept IRS was affected by knowledge level, age, sensitization program ahead of IRS implementation and education level of households.
The authors declare no competing interests.
Kamil Mohammed conceived and implemented the study, supervised the data collection, analyzed the data, and wrote the first version of the manuscript. Angesom Weldu and Bayu Begashaw Bekele supported Kamil Mohammed in conceptualizing and designing the study, participated in the data analysis and interpretation of the results and reviewed the draft manuscript. A map of the study area was constructed with the Bayu Begashaw Bekele. Angesom Weldu and Bayu Begashaw Bekele mentored the interpretation and review of the draft. Bayu Begashaw Bekele and Angesom Weldu supervised the whole work. All the authors read and approved the final manuscript.
We thank Mizan Tepi University, College of Medicine and Health Sciences for providing ethical clearance for this study and Bench Sheko zone health offices and local government officials for allowing us to conduct this study. The authors are also grateful to the participants for their participation in the study and to the data collectors and supervisors for collecting quality data.
Table 1: sociodemographic characteristics of the respondents in the Bench Sheko zone, Southwest Ethiopia, 2023
Table 2: knowledge of participants about causes, preventive measures, modes of transmission of malaria, and high-risk groups in the Bench Sheko Zone, Southwest Ethiopia, 2023
Table 3: participants´ knowledge about indoor residual spray in the Bench Sheko Zone, southwest Ethiopia, 2023
Table 4: factors associated with willingness to accept indoor residual spraying (IRS) for malaria control in the Bench Sheko Zone, southwest Ethiopia, 2023
Figure 1: Bench Sheko zone composed of six districts and two sub city administrations, 2023 (source of map: prepared by the authors using QGIS software)
Figure 2: reasons for refusal of indoor residual spraying (IRS) spraying reported by household heads in Bench Sheko Zone, Ethiopia, 2023
Annex 1: the proportion of respondents who agreed on the acceptance of the indoor residual spraying (IRS) in the Bench Sheko Zone, Ethiopia, 2023 (PDF - 47KB)
- Duguma T, Nuri A, Melaku Y. Prevalence of Malaria and Associated Risk Factors among the Community of Mizan-Aman Town and Its Catchment Area in Southwest Ethiopia. J Parasitol Res. 2022 Apr 12;2022:3503317. PubMed | Google Scholar
- Michaud CM. Global Burden of Infectious Diseases. Encyclopedia of Microbiology. 2009;444-454. Google Scholar
- Statista. Leading 10 causes of death in low-income countries worldwide in 2016 (in deaths per 100,000 population). WHO. Accessed Feb 2, 2024.
- Nalinya S, Musoke D, Deane K. Malaria prevention interventions beyond long-lasting insecticidal nets and indoor residual spraying in low- and middle-income countries: a scoping review. Malar J. 2022;21(1):1-13. PubMed | Google Scholar
- Musoke D, Atusingwize E, Namata C, Ndejjo R, Wanyenze RK, Kamya MR. Integrated malaria prevention in low- and middle-income countries: a systematic review. Malar J. 2023;22(1):79. PubMed | Google Scholar
- Zhou Y, Zhang WX, Tembo E, Xie MZ, Zhang SS, Wang XR et al. Effectiveness of indoor residual spraying on malaria control?: a systematic review and meta ? analysis. Infect Dis Poverty. 2022 Jul 23;11(1):83. PubMed | Google Scholar
- Zhou X-N. China declared malaria-free: a milestone in the world malaria eradication and Chinese public health. Infect Dis Poverty. 2021;10(1):98. PubMed | Google Scholar
- World Health Organization. World malaria report 2022. Geneva. Accessed Feb 2, 2024.
- Bbuye M, Muttamba W, Nassaka L, Nakyomu D, Taasi G, Kiguli S et al. Factors Associated with Linkage to HIV Care Among Oral Self-Tested HIV Positive Adults in Uganda. HIV AIDS (Auckl). 2022;14:61-72. PubMed | Google Scholar
- Pluess B, Tanser FC, Lengeler C, Sharp BL. Indoor residual spraying for preventing malaria. Cochrane database Syst Rev. 2010;2010(4):CD006657. PubMed | Google Scholar
- Pryce J, Medley N, Choi L. Indoor residual spraying for preventing malaria in communities using insecticide-treated nets. Cochrane database Syst Rev. 2022;1(1):CD012688. PubMed | Google Scholar
- Hamusse SD, Balcha TT, Belachew T. The impact of indoor residual spraying on malaria incidence in East Shoa Zone, Ethiopia. Glob Health Action. 2012;5:11619. PubMed | Google Scholar
- Loha E, Lunde TM, Lindtjørn B. Effect of Bednets and Indoor Residual Spraying on Spatio-Temporal Clustering of Malaria in a Village in South Ethiopia: A Longitudinal Study. PLoS One. 2012;7(10):e47354. PubMed | Google Scholar
- Kenea O, Balkew M, Tekie H, Deressa W, Loha E, Lindtjørn B, et al. Impact of combining indoor residual spraying and long-lasting insecticidal nets on Anopheles arabiensis in Ethiopia: results from a cluster randomized controlled trial. Malar J. 2019 May 24;18(1):182. PubMed | Google Scholar
- PMI. Africa IRS (AIRS) Project Indoor Residual Spraying (IRS 2) Task Order Six. Ethiopia 2017 End of Spray Report. 2017. Google Scholar
- Tukei BB, Beke A, Lamadrid-Figueroa H. Assessing the effect of indoor residual spraying (IRS) on malaria morbidity in Northern Uganda: a before and after study. Malar J. 2017;16(1):1-9. PubMed | Google Scholar
- Spraying WI. Use of indoor residual spraying for scaling up global malaria control and elimination. Geneva: World Health Organization. 2006. Google Scholar
- Chanda E, Mzilahowa T, Chipwanya J, Mulenga S, Ali D, Troell P et al. Preventing malaria transmission by indoor residual spraying in Malawi: Grappling with the challenge of uncertain sustainability. Malar J. 2015;14(254):1-7. PubMed | Google Scholar
- Rodríguez AD, Penilla RP, Rodríguez MH, Hemingway J, Trejo A, Hernández-Avila JE. Acceptability and perceived side effects of insecticide indoor residual spraying under different resistance management strategies. Salud Publica Mex. 2006;48(4):317-324. PubMed | Google Scholar
- Sekhon M, Cartwright M, Francis JJ. Acceptability of healthcare interventions: An overview of reviews and development of a theoretical framework. BMC Health Serv Res. 2017;17(1):1-13. PubMed | Google Scholar
- Aongola M, Kaonga P, Michelo C, Zgambo J, Lupenga J, Jacobs C. Acceptability and associated factors of indoor residual spraying for malaria control by households in Luangwa district of Zambia: A multilevel analysis. PLOS Glob Public Heal. 2022;2(8):e0000368. PubMed | Google Scholar
- Sakeni M, Khorram A, Majdzadeh R, Raiesi A. Indoor Residual Spraying Coverage and Acceptability Rates to Control Malaria and the Householders´ Reasons of Acceptance or Rejection of Spraying, in South-East of Iran. Int J Infect. 2015;2(4). Google Scholar
- Mekasha W, Daba C, Malede A, Debela SA, Gebrehiwot M. The Need for Strengthening Health Information Dissemination Toward Indoor Residual Spraying for Malaria Prevention in Malarious Area of Ethiopia. Front Public Health. 2022 Jun 13;10:913905. PubMed | Google Scholar
- Bartley Adam. Evaluating goodness-of-fit for a logistic regression model using the Hosmer-Lemeshow test on samples from a large data set. The Ohio State University. 2014. Accessed Feb 2, 2024.
- Daba C, Atamo A, Debela SA, Kebede E, Woretaw L, Gebretsadik D et al. A Retrospective Study on the Burden of Malaria in Northeastern Ethiopia from 2015 to 2020: Implications for Pandemic Preparedness. Infect Drug Resist. 2023;16:821-828. PubMed | Google Scholar
- Reliefweb. Ethiopia: National Malaria Guidelines, Fourth edition - November 2017. Accessed Feb 2, 2024.
- Taffese HS, Hemming-Schroeder E, Koepfli C, Tesfaye G, Lee M, Kazura J et al. Malaria epidemiology and interventions in Ethiopia from 2001 to 2016. Infect Dis Poverty. 2018;7(1):103. PubMed | Google Scholar
- Ethiopian Public Health Institute. Ethiopia National Malaria Indicator Survey 2015. Accessed Feb 2, 2024.
- CDC. CDC in Ethiopia. 2023. Accessed Feb 2, 2024.
- Geshere G, Dabassa A, Petros B. Trends of malaria prevalence in Ilu Galan, BakoTibe, and Danno Districts of West Shoa Zone, Oromiya Region, Ethiopia. J Biol Chem Res. 2014;31(2):678-93. Google Scholar
- Martin JT, Hemming K, Girling A. The impact of varying cluster size in cross-sectional stepped-wedge cluster randomised trials. BMC Med Res Methodol. 2019;19(1):123. PubMed | Google Scholar
- Sommet N, Morselli D. Keep calm and learn multilevel linear modeling: A three-step procedure using SPSS, Stata, R, and MPlus. Int Rev Soc Psychol. 2021;34(1). Google Scholar
- Staniszewska S, Crowe S, Badenoch D, Edwards C, Savage J, Norman W. The PRIME project: developing a patient evidence-base. Heal Expect an Int J public Particip Heal care Heal policy. 2010;13(3):312-322. PubMed | Google Scholar
- Tairou F, Nawaz S, Tahita MC, Herrera S, Faye B, Tine RCK. Malaria prevention knowledge, attitudes, and practices (KAP) among adolescents living in an area of persistent transmission in Senegal: Results from a cross-sectional study. PLoS One. 2022;17(12):e0274656. PubMed | Google Scholar
- Abbas F, Kigadye E, Mohamed F, Khamis M, Mbaraka J, Serbantez N et al. Socio-demographic trends in malaria knowledge and implications for behaviour change interventions in Zanzibar. Malar J. 2023;22(1):1-11. PubMed | Google Scholar
- Wadunde I, Mpimbaza A, Musoke D, Ssempebwa JC, Ediau M, Tuhebwe D et al. Factors associated with willingness to take up indoor residual spraying to prevent malaria in Tororo district, Uganda: A cross-sectional study. Malar J. 2018;17(1):1-11. PubMed | Google Scholar
- Alhassan RK, Nutor JJ, Gyamerah A, Boakye-Yiadom E, Kasu E, Acquah E et al. Predictors of HIV status disclosure among people living with HIV (PLHIV) in Ghana: the disclosure conundrum and its policy implications in resource limited settings. AIDS Res Ther. 2023;20(1):84. PubMed | Google Scholar
- Ethiopia Ministry of Health. National Malaria Elimination Roadmap: 2017-2030. 2017.
- Dimas HJ, Sambo NM, Ibrahim MS, Ajayi IOO, Nguku PM, Ajumobi OO. Coverage of indoor residual spraying for malaria control and factors associated with its acceptability in Nasarawa state, north-central Nigeria. Pan Afr Med J. 2019 Jun 6:33:84. PubMed | Google Scholar
- Kassam R, Collins JB, Liow E, Rasool N. Narrative review of current context of malaria and management strategies in Uganda (Part I). Acta Trop. 2015;152:252-68. PubMed | Google Scholar
- Asingizwe D, Poortvliet PM, Koenraadt CJM, Van Vliet AJH, Ingabire CM, Mutesa L et al. Role of individual perceptions in the consistent use of malaria preventive measures: Mixed methods evidence from rural Rwanda. Malar J. 2019;18(1):1-19. PubMed | Google Scholar
- Gobena T, Berhane Y, Worku A. Women´s knowledge and perceptions of malaria and use of malaria vector control interventions in Kersa, Eastern Ethiopia. Glob Health Action. 2013 May 23:6:20461. PubMed | Google Scholar
- Ronghangpi M, Saikia AM, Ojah J, Baruah R. Factors associated with refusal of Indoor Residual Spraying in a high endemic district of Assam. Indian J Basic Appl Med Res. 2015;(December):560-564. Google Scholar
- Passah M, Nengnong CB, Wilson ML, Carlton JM, Kharbamon L, Albert S. Implementation and acceptance of government ? sponsored malaria control interventions in Meghalaya , India. Malar J. 2022;21(200):1-14. PubMed | Google Scholar
- Ediau M, Babirye JN, Tumwesigye NM, Matovu JKB, Machingaidze S, Okui O et al. Community knowledge and perceptions about indoor residual spraying for malaria prevention in Soroti district , Uganda: a cross-sectional study. Malar J. 2013 May 27;12:170. PubMed | Google Scholar
- Madani A, Soleimani-Ahmadi M, Davoodi SH, Sanei-Dehkordi A, Jaberhashemi SA, Zare M et al. Household knowledge and practices concerning malaria and indoor residual spraying in an endemic area earmarked for malaria elimination in Iran. Parasit Vectors. 2017 Dec 6;10(1):600. PubMed | Google Scholar
- Degarege A, Fennie K, Degarege D, Chennupati S, Madhivanan P. Improving socioeconomic status may reduce the burden of malaria in sub Saharan Africa: A systematic review and meta-analysis. PLoS One. 2019;14(1):1-26. PubMed | Google Scholar
- Munga S, Kimwetich Z, Atieli F, Vulule J, Kweka EJ. Knowledge and perceptions about indoor residual spray for malaria prevention in mumberes division, Nandi county in central province of Kenya. Tanzan J Health Res. 2017;19(4):1-9. Google Scholar
- Suuron VM, Mwanri L, Tsourtos G, Owusu-Addo E. An exploratory study of the acceptability of indoor residual spraying for malaria control in upper western Ghana. BMC Public Health. 2020;20(1):1-11. PubMed | Google Scholar