Development of a digital mental health platform in the era of COVID-19 pandemic in Kenya: findings and implications
Shillah Mwavua, Carol Ngunu, Isaiah Gitonga, Alex Royea, David Henia, Boniface Chitayi, Peter Memiah, Manasi Kumar
Corresponding author: Shillah Mwaniga Mwavua, Department of Clinical, Neuro, and Developmental Psychology, Faculty of Behavioural and Movement Sciences, Vrije University, Amsterdam, The Netherlands 
Received: 24 Jan 2023 - Accepted: 05 May 2023 - Published: 13 Jun 2023
Domain: Psychiatry, Psychology
Keywords: Digital platforms, mental health, young people, adolescents, COVID-19
©Shillah Mwavua et al. PAMJ-One Health (ISSN: 2707-2800). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Shillah Mwavua et al. Development of a digital mental health platform in the era of COVID-19 pandemic in Kenya: findings and implications. PAMJ-One Health. 2023;11:7. [doi: 10.11604/pamj-oh.2023.11.7.39040]
Available online at: https://www.one-health.panafrican-med-journal.com/content/article/11/7/full
Research 
Development of a digital mental health platform in the era of COVID-19 pandemic in Kenya: findings and implications
Development of a digital mental health platform in the era of COVID-19 pandemic in Kenya: findings and implications
![]() Shillah Mwavua1,2,&, Carol Ngunu2,
Shillah Mwavua1,2,&, Carol Ngunu2, ![]() Isaiah Gitonga3,4, Alex Royea5, David Henia5, Boniface Chitayi 6, Peter Memiah7, Manasi Kumar8
Isaiah Gitonga3,4, Alex Royea5, David Henia5, Boniface Chitayi 6, Peter Memiah7, Manasi Kumar8
&Corresponding author
Introduction: COVID-19 global pandemic exposed mental health gaps that have been salient among adolescents and young people. The glaring gaps include lack of information, undefined referral systems, and inadequate human resources for mental health. We aimed to develop a digital web-based platform to support young people's mental health and psychosocial needs during the COVID-19 pandemic.
Methods: we adopted a mixed methods action research approach to design and pilot a digital mental health intervention for young people during the pandemic. We piloted the platform between Oct 2020 and July 2021, and recruited a sample of 150 young people through community gathering spaces in three informal settlements in Nairobi City County using a convenient sampling method.
Results: overall, participants reported that information provided to them via the platform was pertinent and beneficial, and that the self-assessments improved their mental health and psychosocial awareness and signposted them to available support and services. The support services consisted of informative weekly bulk emails and short motivational messages related to mental health, with a total of, 1343 short messages distributed through the short message service (SMS). Moreover, more than half the participants completed online self-assessments and participated in 19 online sessions.
Conclusion: findings from this pilot study demonstrate that digital mental health systems are feasible and have the potential to improve access to mental health and psychosocial services. This is especially crucial during times of public health crisis, such as the COVID-19 pandemic. The realization of such systems requires swift multistakeholder partnership and investment.
The global COVID-19 pandemic has exposed the mental health gaps that have been salient among adolescents and young people [1,2]. Lack of information, undefined referral systems to mental health services, and inadequate human resources have been identified as major gaps [3,4]. Technology-supported platforms have been found as possible alternatives, considering the shrinking healthcare workforce and the increasing demand for mental health and psychosocial services [2,4-6]. World Health Assembly Resolution on Digital Health, unanimously approved by the WHO Member States in May 2018, demonstrated a collective recognition of the value of digital technologies to contribute to advancing universal health coverage (UHC) and other health aims of the Sustainable Development Goals [7].
A digital mental health intervention refers to information, support, and therapy for mental health conditions delivered through an electronic medium to treat, alleviate, or manage symptoms [7]. Digital mental health is part of digital health, which is rooted in e-Health, defined as “the use of information and communications technology, in support of health and health-related fields” [7]. Various digital mental health platforms have been developed to suit different populations and address specific gaps brought about by the pandemic [6,8]. Many clinicians and patients, alike, are now realizing the full potential of these digital tools, as they become the only alternative to connect at a time when face-to-face visits are restricted [9]. The majority of developed digital mental health interventions are based on Cognitive Behavioral Therapy for anxiety and depression [10], with fewer interventions aimed to improve general well-being. This suggests that researchers may be more likely, to develop interventions based on, existing clinical guidelines despite the effectiveness of tackling general well-being, in non-digital prevention interventions [11]. Kenya has a young population with, approximately three-quarters of the population aged below 30 years. On average, one in every ten people experiences a common mental disorder, with an increase in the number of one to four patients visiting outpatient clinics [12]. Depression, anxiety disorders, and alcohol use disorders are the most common, among young people [12]. The Kenya Mental Health Policy (2015-2030) provides a framework that guides mental health reforms, in the country, to ensure that all persons have access to comprehensive, integrated, and high-quality mental health care that is promotive, preventive, curative, and rehabilitative at all levels of healthcare [13]. As Kenya encounters this demographic transition, rapidly growing cities, mental health problems and extreme inequality among young people, it implies the need to focus on youth empowerment and youth-centered mental health services. In Kenya´s capital city, Nairobi, approximately 50% of the residents live in informal settlements, consisting of a heavy representation of children and adolescents below 24 years [14-16]. Young people are prone to involvement in crime, violence, and risky behaviors such as the use of psychoactive substances, and early and unintended pregnancy leading to poor mental health and social outcomes [17,18].
The COVID-19 pandemic affected different aspects of life, especially among young people living in informal settlements and university students [18-20]. Youths understand each other better and often turn to their peers first when distraught [21]. Social distancing and isolation brought about by the pandemic disrupted their routines and enjoyable activities, and their physical and social connection [22]. The inability to access their regular healthcare providers for routine face-to-face psychosocial services and support exacerbated their worry, making them very anxious and fearful [23]. Both the 2007 and the 2015-2030 mental health policy recognizes youth as a population with specialized needs within mental healthcare services [13]. The policy recommends interventions that are multi-sectoral. To respond to this crisis, relevant stakeholders involved in the provision of mental health services in the city, came together to develop a mental health platform to offer much-needed mental and psychological support during the pandemic. The objective of this study is to describe the collaborative design and development of a digital platform to support the mental health and psychosocial needs of young people during the COVID-19 pandemic.
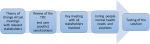
Study design: we adopted an action research approach to design and pilot the platform. Figure 1 summarizes the key steps in the project cycle. Study permission was obtained from the county health management operational research unit in January 2021. We conducted three end-user sensitizations, for youth leaders heading the youth advisory councils from the community gathering spaces, and health care providers.
Study setting: for purposes of piloting the platform, a convenient sample of one hundred and fifty young people aged between 18 and 24 years were invited to participate in the program. They were drawn from three youth gathering spaces within the informal settlements of, Mukuru and Huruma, and Amazing Minds organization. Mukuru informal settlement is located on the Eastern side of Nairobi city in Embakasi South constituency. It is one of the largest slums in Nairobi and stretches along the Nairobi/Ngong River, in the industrial area of the city. The settlement has 9 villages with a population exceeding 118,528 (2019, Kenya population census). Huruma slum is in Mathare Ward of Starehe Constituency in Nairobi, and it comprises six villages with a combined size of approximately 4 hectares with over 2,700 households and a population size of 206,564 (2019, Kenya population census). Amazing minds is a youth-led peer-to-peer organization that works with young people in colleges and universities, supporting them through peer counselling on mental health. Our previous studies [17,23-25] in these settings, indicated that young people living in the informal settings were already experiencing a higher gap in terms of access to mental health and psychosocial services, and therefore our choice of the study setting.
Self-assessment tools: we uploaded seven validated mental health self-assessment tools namely Patient health questionnaire (PHQ9); Cohen Psychosocial support scale; Corona Anxiety Scale; Hurt Insult Threaten Scream tool; Rosenberg scale; Generalized Anxiety Disorder scale 7 and Edinburg Postnatal Depression Scale onto the app to encourage self-assessments and instant scoring by the users. Resource materials on common mental health conditions including depression, anxiety, suicide, stress, and substance abuse were also uploaded. In the social domain, we developed messages that were distributed through the bulk SMS system on topics related to mental health, sexual reproductive health and self-awareness. We also added validated links from the Ministry of Health, Kenya and the WHO on COVID-19.
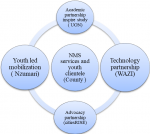
Collaborative learning and design process: the coalition drew together partners from different sectors; the County government of Nairobi, The University of Nairobi, the Youth community (end users), advocacy partners, and technology partners to help in the piloting and learning. We adopted a nonlinear iterative process involving all the listed stakeholders. We held several virtual meetings, focus group discussions and expert interviews to gather insights, share perspectives and derive consensus and ownership of the entire design process. We adopted a stepwise approach during the design thinking process to ensure that relevant stakeholders are on brought on board. Each partner had specific roles and responsibilities in the coalition, as illustrated in Figure 2. We held several engagement meetings with stakeholders including Wazi [26], the technological partner, the youth leaders, and health care workers, on what we wanted to have on the web application. The partner agreed to upgrade their existing digital mental health platform to suit the purpose of this partnership, which was informed by the learnings gained from multiple stakeholders´ engagement meetings we held. Wazi developed an end-to-end web platform that comprised key features as summarized in Figure 3.
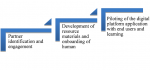
The learnings from the initial in-person meetings highlighted the preferred digital device for accessing the application as smartphones because they were easily accessible and the use of pseudo names for confidentiality. Access to information and linkage to the specific specialists/service providers served as the basis for the technology platform that was initially presented through this collaboration. Additional collaborative learnings shaped the development of additional features like the self-reported well-being score, indicator questions to help identify which gathering space they were from, and improved notifications flow to increase engagement on the application. Before this amendment, notifications needed to be turned on within the user´s account settings, hence couldn´t display for action. Wazi team also added the "join a session" and "talk now" tabs. As a development process, the team undertook extensive system testing, user acceptance tests, and demonstrations internally, with peers, and with other members of the collaborative project. Technical issues, which included login problems experienced with those using the Chrome app, site connection issues on the app leading to dropping in connection, were raised and promptly addressed. We developed rapid testing of multiple channels embedded into the digital platform, with chat rooms, e-group therapy, SMS-based mental health promotion and USSD-based testing of positive mental well-being messaging. The efforts included testing these channels and understanding the practical issues behind the roll-out of such initiatives in formal health services. The application infrastructure was designed to support fluctuations in traffic automatically by scaling specific cloud computing required resources and had reasonable policies to support the high availability of the application which allowed for a smooth user experience. Continuous Integration and Continuous Deployment (CI/CD) pipelines were automated to ensure zero downtime during this deployment lifecycle. This collaborative partnership used a multilevel implementation framework, in three tiers namely, partner identification, resource material development, and piloting of the intervention as illustrated in Figure 4.
Roles of coalition partners
Nairobi Metropolitan Service: The Nairobi Metropolitan Service (NMS) was responsible for the conceptualization of the idea, stakeholder engagement, resource mobilization, and piloting of the intervention, supervision, and documentation. It gave access to the services, information, and linkage to a specialist through the NMS structures. Additionally, NMS developed and gathered relevant information materials as per WHO and local guidelines to provide resources and materials to the young people who accessed the web application. They also carried out baseline meetings with the Youth advisory bodies and end-users, for needs assessment on their mental health needs, sensitized them on the web platform, the layout of services, and got their feedback and buy-in. They also identified pilot facilities (gathering spaces) where the end users could be accessed to participate in the pilot.
Wazi: Wazi as the technological partner was responsible for the system design and app upgrade, enriched by the discussion from the design thinking workshops with stakeholders and end users. They on boarded the peer mentors/psychologists for online therapy, piloted the web application system update, and implemented baseline and end-line assessments to assess the impact of the intervention.
University of Nairobi: the inspire study, through the University of Nairobi, did joint conceptualization of the paper with NMS, assisted in identifying validated and appropriate mental health screening tools, created the thematic mental health motivation weekly messages for the end users, and mobilized resources. The messages were developed in collaboration with other partners, including youth representatives, lay and professional counsellors and psychologists. They also supervised the process and manual development.
citiesRISE: citiesRise through the youth-led community groups helped in the identification of peer mentors, mobilized the youth from the community, identified indicators for measurement during the piloting and gave the financial support for the system licenses and maintenance.
Youths champions and representatives: young people drawn from the study areas were sensitized about the platform and their views sort on the design and buy in of the platform. They were instrumental on creating awareness and inviting of their peers from their safe spaces to use the platform. Their feedback as the end-users was continuously sought through user experience interviews, and focus group discussions. Which were then incorporated to improve the design and general usability of the platform. Their role and participation in the process is shown in Figure 1 and Figure 2.
The process outcomes and feasibility results are discussed below. Impact results are discussed in a separate manuscript under preparation.
Process outcomes: some of the features that emerged from the design process that were adapted into the web application were: (1) “talk now” functionality which allowed peers to join a conversation instantly with peer counselors, (2) customized mental health tools, (3) customized content modules around various topics, (4) simple booking and scheduling to allow for the booking of a future session, (5) in-application surveys to collect additional feedback from peers. Through the 10-month project (Oct 2020-July 2021) we were able to reach 150 young people (male-50, female-100) aged between 18-24 years old, across 3 gathering spaces by informing, connecting and linking them to crucial mental health information and resources in the context of the COVID-19 pandemic. They also received motivational messages through weekly bulk short messaging. Additionally, the participants accessed youth friendly services such as the Sexual Reproductive Health (SRH) services. Furthermore, 162 users conducted 140 mental health self-assessments using the tools embedded in the platform. Fifteen peers´ mentors from the three gathering spaces were on boarded onto the app and constantly supported through Whatsapp platforms. The peer mentors were able to conduct 19 group sessions addressing topics such as anxiety, depression, and tenets of self-care, coping and resilience. Individual and group video calls by the young people, assisted by the adolescent and youth champions, were held at the gathering spaces.
Feasibility results: the platform was created to increase access to mental health support services for beneficiaries, safely and easily. The key features of the web application were tested during this process to identify the feasibility of the design of the platform. The general acceptability of the platform was positive, as we had users sign up, access content, book and join sessions, as well as take assessments. This was evidenced by the high rate of uptake that was able to reach the targeted 150 users. A retention rate of 91.3% was attained, a fact attributed to the pre-piloting sensitization workshop done three months before the roll-out of the intervention.
User experience interviews: after conducting user experience interviews, participants reported that the platform was easy to use, and they didn´t need much guidance to use it. Here are some of the illustrative quotes; 'Good application, easy to use, especially being able to book a session with a therapist or joining an ongoing session. Additionally, it is able to notify you on upcoming sessions'. 'The App having the personal assessments on mental health is important, especially during this COVID-19 period. We were able to solve our anxieties that arose as a result of exposure to the pandemic'. 'Availability of articles that one may interact with on various topics revolving around mental health and the youth'. Participants reported that the platform was generally simple to use and required little to no guidance to learn how to use it.
Peer mentors/therapist onboarding sessions: we held multiple onboarding sessions with the therapists and peer mentors to ensure that they were familiar with features relevant to them, such as schedule management. Once onboarding was completed, therapists and peer mentors reported that the platform was simple to understand and use.
This process paper aimed to present a stepwise collaborative design and development of a digital mental health platform to support the mental and psychosocial needs of young people during the pandemic. Utilizing action research and collaborative design methodologies, we have demonstrated that different players can come together and develop services promptly, especially during crises. From a therapy point of view, we utilized relevant theories such as resilience theories, which argue that it is not always the nature of adversity that is most important but rather how we learn to deal with it and bounce back [27]. These theories helped to inform the areas of emphasis in terms of content development and information packages. The conceptual framework for the platform was based on mental health and information technology expert feedback, existing guidelines on youth involvement [28], a review of both academic and gray literature on mental health and psychosocial needs during the pandemic [29-33]. The opportunity in this context was increasing access to and ownership of mobile telephony by the young people in Nairobi county, which currently stands at above 70% [34,35].
Learnings from this process paper could inform the design and development of future interventions and services to respond to similar crises. Central to this process is the multi-stakeholder approach, with each stakeholder bringing on board their expertise and leveraging on partners´ strengths. Teamwork and collaborative efforts are critical in responding to humanitarian crises, such as the COVID-19 pandemic [36,37]. This has been found critical in circumventing potential challenges associated with designing complex interventions [38,39]. These could be related to expertise or resource gaps. Additionally, the design period is significantly reduced, and thus the intervention can respond to the crisis within a short time. This cannot be possible when organizations and or individuals work in silos. Such coalitions bring people together to contribute their expertise for the benefit of a shared goal or objective.
A key lesson from this collaboration is the need for user experience in the design process. User involvement in the design ensures that design teams create products that respond to the needs of the users in ways they like [39,40]. Involving youth ambassadors and young people in the design and development of this platform enabled the coalition to respond to the needs of this dynamic population. A major criticism of digital health technologies is the lack of user involvement in their design [41] which results in products either not being acceptable or impactful to the potential users [37,39-41] and potentially resulting in waste of resources used in the development of the product or platform. We attribute the high acceptability of the platform to the extensive involvement of users in the process. Moving into the future, users should be involved in the design of products and services that are responsive to their needs. This is particularly important when designing interventions/products or services for dynamic populations such as young people.
In implementation science, the concept of public and patient involvement (PPI) in research is now becoming the norm [42,43]. Involvement is not only in the utilization of the process but �meaningful engagement´ where users are involved in designing interventions meant for them [43]. This is a drastic shift from what used to be �a mere validation´ of research findings with users. In this collaborative design, PPI was central to the process, and this could have contributed to a seamless process and higher uptake/acceptability of the platform by the very users it was designed for. This approach proves that tackling issues of mental health within cities in a digital space; from information sharing, connection to services and linkage to a specialist, requires a collaborative/ multi-stakeholder approach to effectively reach the intended users. This is corroborated by studies that have demonstrated the role of perceived need and outcome expectations as factors that affect engagement with e-Health interventions [43,44]. We recommend this approach in the future design of interventions especially targeted at young people.
These findings demonstrate that digital platforms that promote therapeutic relationships have the potential to revolutionize mental health support for young people, especially during crisis situations, by providing access to information and linking them to services. Secondly, this process paper underscores the critical value of collaborative response in crisis response, especially pandemics such as the COVID-19 pandemic. Finally, the paper highlights the need for user engagement in the design of interventions, especially those involving dynamic populations such as the youth.
What is known about this topic
- There exists a high unmet need for mental health and psychosocial services among adolescents and young people;
- COVID 19 pandemic worsened the situation, considering the increased demand for mental health and psychosocial needs and shrinking mental health workforce.
What this study adds
- Digital mental health services are a viable option to increase access to mental health and psychosocial needs, especially among adolescents and young people;
- Collaborations among relevant stakeholders can lead to faster and effective innovations, especially during crisis response interventions;
- The need for user engagement in the design of interventions, especially for dynamic populations such as the youth.
The authors declare no competing interests.
Shillah Mwavua, Manasi Kumar, Carol Ngunu, Alex Royea, David Henia and Boniface Chitayi conceptualized, designed, and implemented the study. Alex Royea and David Henia provided technological expertise. Shillah Mwavua, Manasi Kumar and Isaiah Gitonga drafted the first manuscript with contributions from all Carol Ngunu, Alex Royea, David Henia and Boniface Chitayi and Peter Memiah. Peter Memiah reviewed the final draft. All the authors have read and agreed to the final manuscript.
This project was partially supported by CitiesRise under the Global Development Incubator INC. (“GDI”) _Program Initiative. We acknowledge Yvonne Ochieng, Joyce Arita, Moitreyee Sinha, Milka Muturi, and Fredrick Azariah from CitiesRISE for their roles in study implementation. We are also grateful to Julie Buku from Wazi for providing online therapy services during project implementation. Finally, we want to thank the young people through the leadership of Martha Kombe and Merci Niyibeshaho from youth advisory council, Yvonne Ochieng from CitiesRise and Samuel Talam from Amazing minds organization, who mobilized the youth and all the young people who volunteered to participate in the pilot project and provided useful feedback.
Figure 1: project cycle
Figure 2: coalition partners
Figure 3: user interphase on the Wazi platform
Figure 4: collaborative design process
- Pfefferbaum B, North CS. Mental health and the COVID-19 pandemic. N Engl J Med. 2020;383(6):510-512. PubMed | Google Scholar
- Moreno C, Wykes T, Galderisi S, Nordentoft M, Crossley N, Jones N et al. How mental health care should change as a consequence of the COVID-19 pandemic. The Lancet Psychiatry. 2020;7(9):813-824. PubMed | Google Scholar
- Dong L, Bouey J. Public mental health crisis during COVID-19 pandemic, China. Emerg Infect Dis. 2020;26(7):1616. PubMed | Google Scholar
- Di Carlo F, Sociali A, Picutti E, Pettorruso M, Vellante F, Verrastro V et al. Telepsychiatry and other cutting?edge technologies in COVID-19 pandemic: Bridging the distance in mental health assistance. Int J Clin Pract. 2021 Jan;75(1):10.1111/ijcp.13716. PubMed | Google Scholar
- Boshe J, Brtek V, Beima-Sofie K, Braitstein P, Brooks M, Denison J et al. Integrating Adolescent Mental Health into HIV Prevention and Treatment Programs: Can Implementation Science Pave the Path Forward. AIDS Behav. 2023 May;27(Suppl 1):145-161. PubMed | Google Scholar
- Feijt M, De Kort Y, Bongers I, Bierbooms J, Westerink J, IJsselsteijn W. Mental health care goes online: Practitioners´ experiences of providing mental health care during the COVID-19 pandemic. Cyberpsychology, Behav Soc Netw. 2020;23(12):860-864. PubMed | Google Scholar
- WHO. WHO guideline: recommendations on digital interventions for health system strengthening: executive summary. World Health Organization. 2019. PubMed | Google Scholar
- Drissi N, Ouhbi S, Marques G, de la Torre Díez I, Ghogho M, Janati Idrissi MA. A systematic literature review on e-mental health solutions to assist health care workers during COVID-19. Telemed e-Health. 2021;27(6):594-602. PubMed | Google Scholar
- Memiah P, Lathan-Dye M, Opanga Y, Muhula S, Gitahi-Kamau N, Kamau A et al. Highlighting a Digital Platform to Assess Young People Needs: Reaching and Engaging Adolescents and Young Adults for Care Continuum in Health Project (REACH). Adolescents. 2022;2(2):150-163. Google Scholar
- Lattie EG, Adkins EC, Winquist N, Stiles-Shields C, Wafford QE, Graham AK. Digital mental health interventions for depression, anxiety, and enhancement of psychological well-being among college students: systematic review. J Med Internet Res. 2019;21(7):e12869. PubMed | Google Scholar
- Bergin AD, Vallejos EP, Davies EB, Daley D, Ford T, Harold G et al. Preventive digital mental health interventions for children and young people: a review of the design and reporting of research. NPJ Digit Med. 2020 Oct 15;3:133. PubMed | Google Scholar
- Ministry of Health Kenya. The Taskforce on Mental Health. Nairobi; 2020. Accessed January 23, 2023.
- Ministry of Health. Kenya mental health policy 2015 - 2030. 2015. Nairobi. Accessed January 23, 2023.
- Ren H, Guo W, Zhang Z, Kisovi LM, Das P. Population density and spatial patterns of informal settlements in Nairobi, Kenya. Sustainability. 2020;12(18):7717. Google Scholar
- Vučković M, Adams AM. Population and Health Policies in Urban Areas. In: International Handbook of Population Policies. Springer. 2022;397-429. Google Scholar
- Wamukoya M, Kadengye DT, Iddi S, Chikozho C. The Nairobi Urban Health and Demographic Surveillance of slum dwellers, 2002-2019: Value, processes, and challenges. Glob Epidemiol. 2020;2:100024. Google Scholar
- Kumar M, Yator O, Nyongesa V, Kagoya M, Mwaniga S, Kathono J et al. Interpersonal Psychotherapy´s problem areas as an organizing framework to understand depression and sexual and reproductive health needs of Kenyan pregnant and parenting adolescents: a qualitative study. BMC Pregnancy Childbirth. 2022;22(1):940. PubMed | Google Scholar
- Wado YD, Austrian K, Abuya BA, Kangwana B, Maddox N, Kabiru CW. Exposure to violence, adverse life events and the mental health of adolescent girls in Nairobi slums. BMC Womens Health. 2022;22(1):1-11. PubMed | Google Scholar
- von Seidlein L, Alabaster G, Deen J, Knudsen J. Crowding has consequences: Prevention and management of COVID-19 in informal urban settlements. Build Environ. 2021 Jan 15;188:107472. PubMed | Google Scholar
- Nyadera IN, Onditi F. COVID-19 experience among slum dwellers in Nairobi: A double tragedy or useful lesson for public health reforms. Int Soc Work. 2020;63(6):838-841. Google Scholar
- Memiah P, Kamau A, Opanga Y, Muhula S, Nyakeriga E, Humwa F et al. Using friendship ties to understand the prevalence of, and factors associated with, intimate partner violence among adolescents and young adults in Kenya: Cross-Sectional, respondent-driven survey study. Interact J Med Res. 2020;9(4):e19023. PubMed | Google Scholar
- Xie X, Xue Q, Zhou Y, Zhu K, Liu Q, Zhang J et al. Mental Health Status Among Children in Home Confinement During the Coronavirus Disease 2019 Outbreak in Hubei Province, China. JAMA Pediatr. 2020;174(9):898-900. PubMed | Google Scholar
- Memiah P, Wagner FA, Kimathi R, Anyango NI, Kiogora S, Waruinge S et al. Voices from the Youth in Kenya Addressing Mental Health Gaps and Recommendations. Int J Environ Res Public Health. 2022;19(9):5366. PubMed | Google Scholar
- Osok J, Kigamwa P, Stoep A Vander, Huang KY, Kumar M. Depression and its psychosocial risk factors in pregnant Kenyan adolescents: A cross-sectional study in a community health Centre of Nairobi. BMC Psychiatry. 2018 May 18;18(1):136. PubMed | Google Scholar
- Tele A, Kathono J, Mwaniga S, Nyongesa V, Yator O, Gachuno O et al. Prevalence and risk factors associated with depression in pregnant adolescents in Nairobi, Kenya. J Affect Disord Reports. 2022;10:100424. PubMed | Google Scholar
- Wazi. 2022. Accessed 3 January 1988.
- Greene RR, Galambos C, Lee Y. Resilience theory: Theoretical and professional conceptualizations. J Hum Behav Soc Environ. 2004;8(4):75-91. Google Scholar
- UNESCO. Meaningfully engaging with youth: Guidance and training for UN staff. 2019. Accessed January 23, 2023.
- Torales J, O´Higgins M, Castaldelli-Maia JM, Ventriglio A. The outbreak of COVID-19 coronavirus and its impact on global mental health. International Journal of Social Psychiatry. Int J Soc Psychiatry. 2020 Jun;66(4):317-320. PubMed | Google Scholar
- Ornell F, Schuch JB, Sordi AO, Kessler FHP. “Pandemic fear” and COVID-19: mental health burden and strategies. Brazilian J Psychiatry. Braz J Psychiatry. 2020;42(3):232-235. PubMed | Google Scholar
- Wang C, Pan R, Wan X, Tan Y, Xu L, Ho CS et al. Immediate psychological responses and associated factors during the initial stage of the 2019 coronavirus disease (COVID-19) epidemic among the general population in China. Int J Environ Res Public Health. 2020 Mar 6;17(5):1729. PubMed | Google Scholar
- Chaix B, Delamon G, Guillemassé A, Brouard B, Bibault JE. Psychological distress during the COVID-19 pandemic in France: A national assessment of at-risk populations. Gen Psychiatry. 2020;33(6):1-6. PubMed | Google Scholar
- Liu S, Yang L, Zhang C, Xiang YT, Liu Z, Hu S et al. Online mental health services in China during the COVID-19 outbreak. Lancet Psychiatry. 2020 Apr;7(4):e17-e18. PubMed | Google Scholar
- Wyche S. Exploring mobile phone and social media use in a Nairobi slum: a case for alternative approaches to design in ICTD. InProceedings of the Seventh International Conference on Information and Communication Technologies and Development 2015 May 15 (pp. 1-8). Google Scholar
- Kharono B, Kaggiah A, Mugo C, Seeh D, Guthrie BL, Moreno M et al. Mobile technology access and use among youth in Nairobi, Kenya: implications for mobile health intervention design. Mhealth. 2022 Jan 20;8:7. PubMed | Google Scholar
- Arslan A, Golgeci I, Khan Z, Al-Tabbaa O, Hurmelinna-Laukkanen P. Adaptive learning in cross-sector collaboration during global emergency: conceptual insights in the context of COVID-19 pandemic. Arslan A, Golgeci I, Khan Z, Al-Tabbaa O, Hurmelinna-Laukkanen P. Adaptive learning in cross-sector collaboration during global emergency: conceptual insights in the context of COVID-19 pandemic. Multinational Business Review. 2021 Jan 7;29(1):21-42. Google Scholar
- Al-Omoush KS, Orero-Blat M, Ribeiro-Soriano D. The role of sense of community in harnessing the wisdom of crowds and creating collaborative knowledge during the COVID-19 pandemic. J Bus Res. 2021;132:765-774. PubMed | Google Scholar
- Ye X, Frens J, Hu J. Adjusting to a Distributed Collaborative Design Process During the COVID-19 Pandemic. IEEE Pervasive Comput. 2021;20(4):9-17. Google Scholar
- Cankurtaran P, Beverland MB. Using design thinking to respond to crises: B2B lessons from the 2020 COVID-19 pandemic. Ind Mark Manag. 2020;88:255-260. Google Scholar
- Bano M, Zowghi D. User involvement in software development and system success: a systematic literature review. InProceedings of the 17th International Conference on Evaluation and Assessment in Software Engineering 2013 Apr 14 (pp. 125-130). Google Scholar
- Vargo D, Zhu L, Benwell B, Yan Z. Digital technology use during COVID-19 pandemic: A rapid review. Hum Behav Emerg Technol. 2021;3(1):13-24. Google Scholar
- Holmes L, Cresswell K, Williams S, Parsons S, Keane A, Wilson C et al. Innovating public engagement and patient involvement through strategic collaboration and practice. Res Involv Engagem. 2019 Oct 21;5:30. PubMed | Google Scholar
- Essex R, Ocloo J, Rao M. The need to establish sustainable public and patient involvement in research in low and middle income countries. J R Soc Med. 2019;112(11):456-458. PubMed | Google Scholar
- Karekla M, Kasinopoulos O, Neto DD, Ebert DD, Van Daele T, Nordgreen T et al. Best practices and recommendations for digital interventions to improve engagement and adherence in chronic illness sufferers. Eur Psychol. 2019;24(1):49. Google Scholar